## Clinical Context This is a **complicated presentation of Meconium Aspiration Syndrome (MAS) with secondary pneumothorax** — a life-threatening complication requiring urgent intervention. The infant has failed CPAP therapy and developed a tension physiology. ## Why This Infant Has Worsened | Finding | Mechanism | |---------|----------| | Progressive RR (82/min), severe retractions | Increased work of breathing; CPAP inadequate | | SpO₂ 82% on CPAP + FiO₂ 0.6 | Refractory hypoxemia | | PaCO₂ 68, pH 7.18 | Severe respiratory acidosis | | Pneumothorax on CXR | Air leak from over-distended alveoli (barotrauma from MAS + CPAP) | | HR 165/min | Compensatory tachycardia; possible tension physiology | **Key Point:** Pneumothorax in MAS occurs due to **ball-valve obstruction** by meconium → air trapping → alveolar rupture → pneumothorax. This is a known complication in ~5–10% of MAS cases. ## Management of Pneumothorax in MAS ```mermaid flowchart TD A[Pneumothorax on CXR in MAS]:::outcome --> B{Tension physiology?}:::decision B -->|Yes: hypotension, bradycardia, cyanosis| C[Needle aspiration immediately]:::urgent B -->|No: stable, SpO₂ manageable| D{Size & symptoms?}:::decision C --> E[Intubate + mechanical ventilation]:::action E --> F[Chest tube placement]:::action D -->|Small, asymptomatic| G[Observe, high FiO₂ to promote reabsorption]:::action D -->|Large or symptomatic| H[Chest tube placement]:::action F --> I[Manage underlying MAS]:::action H --> I ``` ## Why Needle Aspiration First? **High-Yield:** In a **symptomatic, deteriorating infant with pneumothorax**: 1. **Needle aspiration (22–24 G needle into 2nd intercostal space, midclavicular line)** provides **immediate relief** of tension physiology 2. Allows time for **intubation preparation** without further deterioration 3. Converts tension pneumothorax → simple pneumothorax 4. Buys time for definitive chest tube placement **Clinical Pearl:** Needle aspiration is a **temporizing measure**. Definitive management requires: - **Intubation** (to protect airway, control ventilation, prevent further air leak) - **Mechanical ventilation** (with lower peak pressures initially, then adjusted to prevent recurrent barotrauma) - **Chest tube placement** (for ongoing air leak and lung re-expansion) ## Why This Infant Needs Intubation **Key Point:** Indications for intubation in this case: 1. **Refractory hypoxemia** — SpO₂ 82% despite CPAP + FiO₂ 0.6 2. **Severe respiratory acidosis** — PaCO₂ 68, pH 7.18 (not compatible with CPAP alone) 3. **Severe respiratory distress** — RR 82, severe retractions 4. **Pneumothorax requiring chest tube** — intubation reduces ongoing air leak and allows controlled ventilation ## Ventilation Strategy Post-Intubation **Warning:** Avoid high peak inspiratory pressures (PIP) in MAS — this caused the pneumothorax in the first place. Use: - **Gentle ventilation** with permissive hypercapnia (target PaCO₂ 45–55 mmHg initially) - **Lung-protective strategies** (low tidal volumes 6–8 mL/kg, PEEP 5–8 cm H₂O) - **Surfactant** — consider exogenous surfactant in intubated MAS to counteract meconium-induced inactivation - **Avoid excessive FiO₂** — wean toward SpO₂ 90–95% ## Why Not Continue CPAP? **Reasoning:** CPAP has **failed** — SpO₂ 82% despite FiO₂ 0.6, PaCO₂ 68, severe distress. Increasing FiO₂ to 1.0 and observing risks: - Continued hypoxemia and hypercarbia - Worsening acidosis - Potential tension pneumothorax if air leak continues - Oxygen toxicity from prolonged FiO₂ 1.0 Spontaneous reabsorption of pneumothorax occurs over days to weeks — this infant cannot wait. 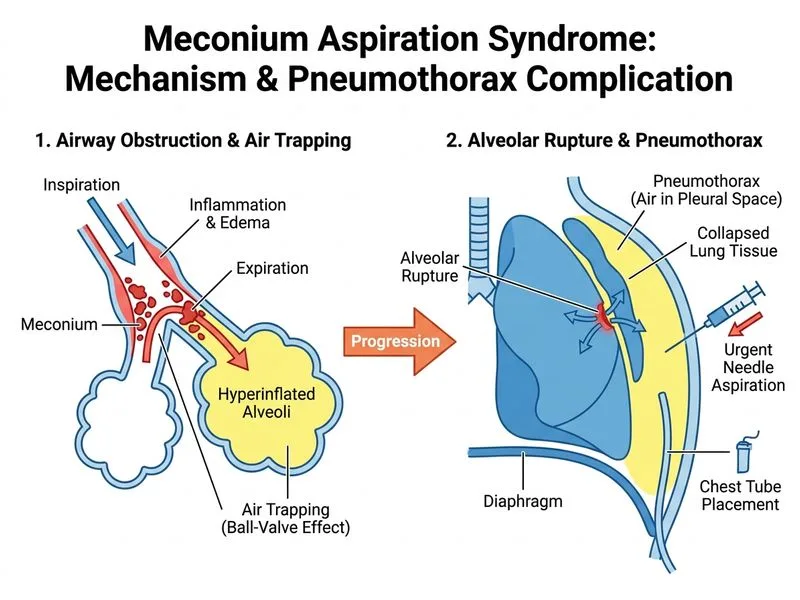
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.