## Echocardiography in MAS-Associated Pulmonary Hypertension **Key Point:** Echocardiography is the investigation of choice for assessing right ventricular function, estimating pulmonary artery pressure, and detecting pulmonary hypertension in neonates with severe meconium aspiration syndrome. ### Pathophysiology of Pulmonary Hypertension in MAS Meconium aspiration causes: 1. **Airway obstruction** → air trapping → increased intrathoracic pressure 2. **Hypoxemia and hypercarbia** → pulmonary vasoconstriction 3. **Inflammation** → release of vasoactive mediators (endothelin, leukotrienes) 4. **Increased pulmonary vascular resistance (PVR)** → right ventricular strain 5. **Right-to-left shunting** → worsening hypoxemia (vicious cycle) Pulmonary hypertension occurs in 10–15% of MAS cases and is associated with poor prognosis. ### Echocardiographic Assessment **High-Yield:** Echocardiography provides: | Parameter | What It Shows | Clinical Significance | |-----------|---------------|----------------------| | **RV systolic function** | RV dilatation, reduced contractility, flattened interventricular septum | Indicates RV afterload mismatch and severity of PH | | **Tricuspid regurgitation (TR) jet** | Velocity of TR allows estimation of RVSP via Bernoulli equation: RVSP = 4(V²) + RAP | Estimates systolic pulmonary artery pressure non-invasively | | **Septal flattening** | Bowing of IVS into LV during systole | Indicates RV pressure ≥ LV pressure (severe PH) | | **Ductal shunting** | Right-to-left shunt across PDA or foramen ovale | Confirms right-to-left shunting and severe PH | | **Pericardial effusion** | Fluid around heart | Sign of RV failure | ### Diagnostic Criteria for Pulmonary Hypertension - **RVSP > 40 mmHg** (estimated from TR jet) = moderate-to-severe PH - **Right-to-left shunting** on color Doppler = severe PH with hemodynamic compromise - **RV dysfunction** = poor prognosis, high mortality **Clinical Pearl:** Bedside echocardiography can be performed within minutes in the NICU, allowing rapid assessment and guiding escalation to inhaled nitric oxide (iNO) therapy, which is the cornerstone of PH management in MAS. ### Why Echocardiography Is Superior - **Non-invasive:** No radiation, no catheterization risk - **Real-time assessment:** Can be repeated serially to monitor response to therapy - **Functional information:** Assesses RV contractility and shunt direction, not just pressure estimates - **Guides therapy:** Presence of severe PH with right-to-left shunting is an indication for iNO ## Why Other Options Are Incorrect - **Cardiac catheterization:** Invasive, carries risk of perforation and arrhythmia in neonates. Reserved for cases where non-invasive assessment is inconclusive or for therapeutic intervention (e.g., balloon atrial septostomy in refractory cases). Not first-line. - **Pulmonary function testing:** Not feasible in acutely ill neonates and does not assess cardiac function or estimate pulmonary artery pressure. - **CT chest:** Exposes the neonate to significant radiation and requires transport out of the NICU. Not indicated for acute assessment of PH; reserved for ruling out structural lung disease in stable patients. 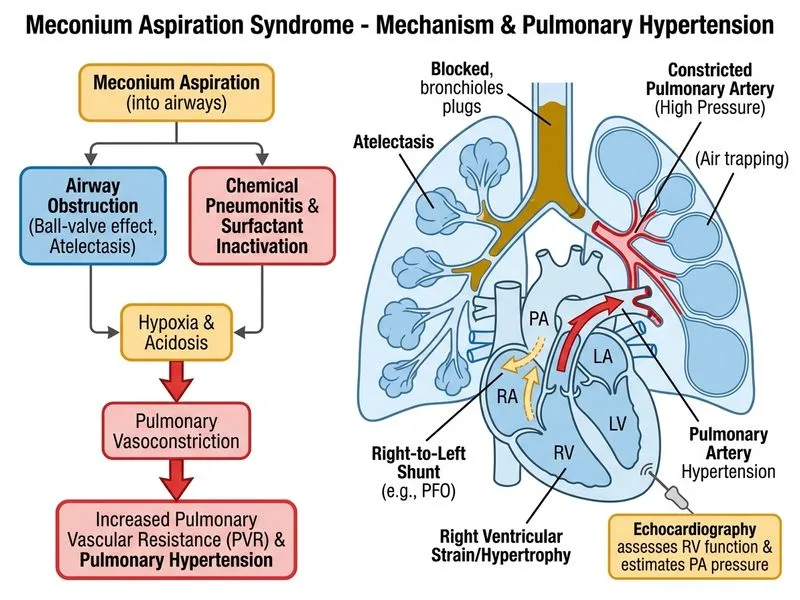
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.