## Clinical Context This 6-hour-old infant with meconium aspiration syndrome is on mechanical ventilation with: - Hypoxemia (PaO₂ 65 mmHg on FiO₂ 0.6) - Hypercapnia (PaCO₂ 52 mmHg) - Respiratory acidosis (pH 7.28) - Bilateral patchy infiltrates (confirmed MAS) - No pneumothorax ## Pathophysiology of MAS ```mermaid flowchart TD A[Meconium aspiration]:::outcome --> B[Airway obstruction + inflammation]:::outcome B --> C[Ventilation-perfusion mismatch]:::outcome C --> D[Hypoxemia + hypercarbia]:::outcome D --> E{Severe hypoxemia?}:::decision E -->|Yes| F[Surfactant deficiency + inactivation]:::outcome F --> G[Surfactant replacement]:::action E -->|Moderate| H[Optimize conventional ventilation]:::action D --> I{Persistent hypoxemia despite FiO₂ 0.8-1.0?}:::decision I -->|Yes| J[Consider iNO or ECMO]:::action I -->|No| K[Continue supportive care]:::action ``` ## Key Point: **Exogenous surfactant is indicated in MAS when mechanical ventilation is required with persistent hypoxemia.** Meconium inactivates and depletes surfactant, worsening atelectasis and ventilation-perfusion mismatch. Surfactant replacement: 1. Reduces surface tension in alveoli 2. Improves lung compliance 3. Enhances oxygenation and ventilation 4. Reduces need for high FiO₂ and airway pressures ## High-Yield: **Surfactant use in MAS is evidence-based and recommended by major guidelines** (AAP, ACOG, European Respiratory Society) when: - Infant requires mechanical ventilation - Persistent hypoxemia despite FiO₂ ≥ 0.6 - Bilateral infiltrates on CXR This infant meets ALL criteria. Surfactant administration is the next step before escalating to HFOV or iNO. ## Clinical Pearl: **Meconium-stained amniotic fluid contains substances that inactivate surfactant**, including free fatty acids, bile salts, and proteases. This is why MAS often presents with surfactant deficiency despite term gestation. Early surfactant replacement improves outcomes and reduces need for ECMO. ## Ventilation Strategy After Surfactant After surfactant administration: 1. **Optimize conventional ventilation** (gentle ventilation strategy to avoid volutrauma) 2. Monitor ABG in 15–30 minutes 3. Wean FiO₂ and pressures as oxygenation improves 4. Reserve HFOV for failure of conventional ventilation 5. Consider iNO if pulmonary hypertension develops (right-to-left shunting) ## Why NOT Increase FiO₂ to 1.0 Immediately? While supplemental oxygen is needed, jumping to FiO₂ 1.0 without addressing underlying surfactant deficiency is ineffective. Surfactant replacement addresses the ROOT cause (surfactant inactivation), whereas high FiO₂ alone treats only the symptom (hypoxemia). Additionally, prolonged high FiO₂ increases risk of oxygen toxicity. 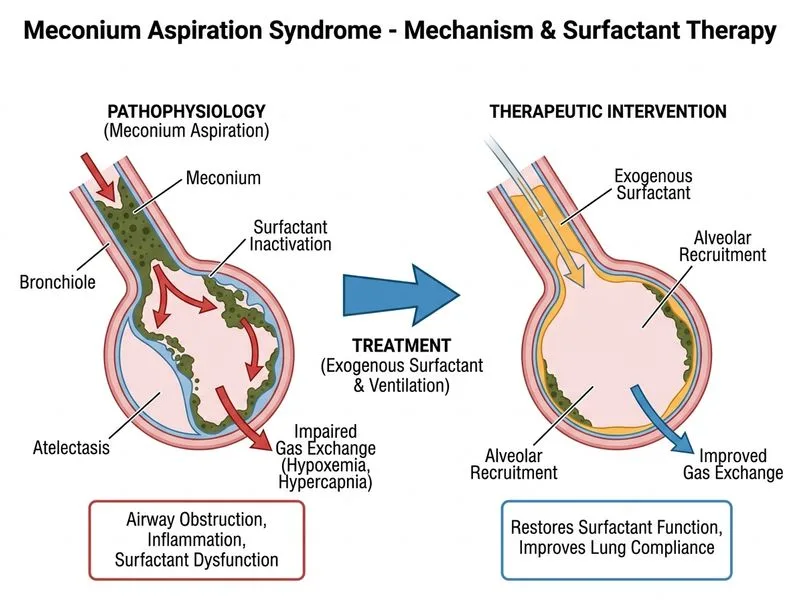
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.