## Clinical Scenario Analysis This patient has a **complete acute median nerve transection** at the wrist level, evidenced by: - Loss of **thumb opposition** (Opponens pollicis — recurrent motor branch of median nerve) - Loss of **flexion of index and middle finger DIP joints** (Flexor digitorum profundus to digits 2–3 — anterior interosseous nerve, a branch of median nerve) - **Sensory loss in the distribution of median nerve** (thumb, index, middle, lateral ring finger) - **Acute mechanism** (knife laceration) with **contaminated wound** ## Immediate Management Priorities ```mermaid flowchart TD A[Acute Median Nerve Laceration at Wrist]:::outcome --> B[Immediate First Aid]:::action B --> C["1. Stop bleeding, elevate limb<br/>2. Irrigate wound with saline<br/>3. Tetanus prophylaxis<br/>4. Broad-spectrum antibiotics"] C --> D{Contaminated wound?}:::decision D -->|Yes| E["Infection control priority<br/>Do NOT attempt primary repair yet"]:::urgent E --> F[Urgent referral to peripheral nerve surgeon]:::action F --> G["Assessment within 6-8 hours<br/>Plan repair after infection risk managed"]:::action D -->|No| H[Clean wound, consider immediate repair]:::action G --> I[Delayed primary or secondary repair]:::outcome ``` ## Why NOT Immediate Primary Repair? **High-Yield:** Although the **golden period for nerve repair is 6–12 hours**, a **contaminated wound takes priority**. Attempting primary repair in a contaminated field risks: - Catastrophic infection (necrotizing fasciitis, osteomyelitis) - Graft failure - Loss of limb function or limb itself **Key Point:** The correct sequence is: 1. **Infection control first** — irrigation, debridement, antibiotics, tetanus prophylaxis 2. **Urgent specialist referral** — peripheral nerve surgeon or hand surgeon 3. **Delayed primary or secondary repair** — once infection risk is minimized (typically 24–72 hours) **Clinical Pearl:** In contaminated wounds, **delayed primary repair** (within 3 weeks) has outcomes nearly equivalent to immediate primary repair, but with far lower infection morbidity. The nerve ends can be tagged with a suture to prevent retraction if time permits. ## Correct Management Sequence 1. **Immediate (at presentation):** - Hemostasis and elevation - Copious irrigation with normal saline - Tetanus prophylaxis (if indicated) - Broad-spectrum antibiotics (e.g., amoxicillin-clavulanate + gentamicin for contaminated wounds) - Dressing with sterile, non-adherent material 2. **Urgent (within 6–8 hours):** - Referral to peripheral nerve surgeon or hand surgeon - Assessment of wound, nerve, and surrounding structures - Decision on timing of repair (delayed primary vs. secondary) 3. **Surgical (24–72 hours):** - Formal debridement under anesthesia - Nerve repair under operating microscope (if infection risk controlled) - Tension-free, epineurial or fascicular repair ## Why NOT the Other Options? **Immediate primary repair without infection control** is dangerous — the contaminated wound is a contraindication to immediate repair. Infection will compromise the repair and may lead to permanent disability or amputation. **Conservative dressing with observation for 2 weeks** is inappropriate — the nerve ends will retract and become scarred, making later repair technically difficult or impossible. The patient will have progressive denervation atrophy during this period. **EMG at this stage** is premature and unnecessary — the clinical diagnosis is clear. EMG is useful for prognostication or detecting partial injuries, but it should not delay urgent surgical referral. EMG is typically done at 2–3 weeks post-injury to assess for denervation. ## Prognosis With appropriate delayed primary repair, recovery of median nerve function is good — sensory recovery is often excellent, and motor recovery (thumb opposition) is fair to good if repair is performed within 3 weeks. 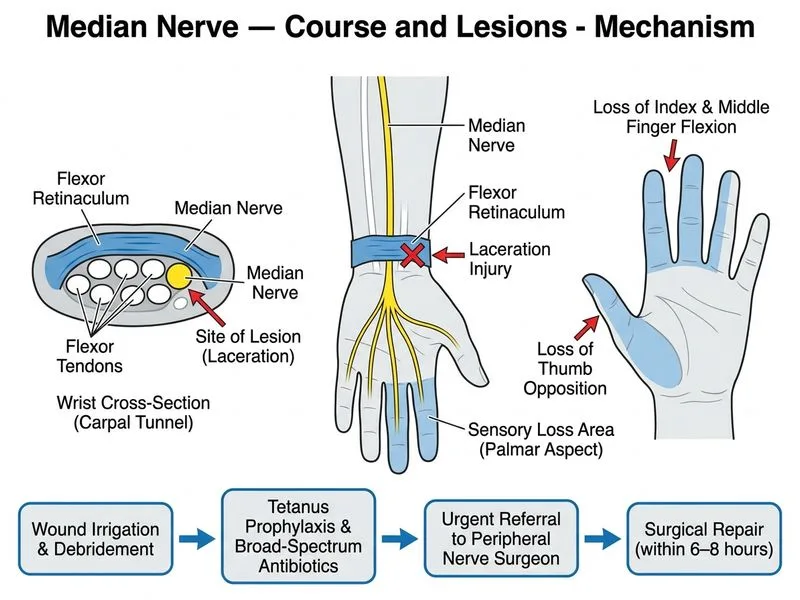
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.