## Clinical Context: B12 Deficiency in Crohn's Disease **Key Point:** Crohn's disease causes B12 deficiency primarily through **malabsorption in the terminal ileum**, where the intrinsic factor–B12 complex is absorbed. This is the most common mechanism of B12 deficiency in inflammatory bowel disease. ## Why Terminal Ileum Matters for B12 Absorption | Step | Location | Function | Affected in Crohn's? | |------|----------|----------|---------------------| | B12 binding to intrinsic factor | Stomach | Gastric parietal cells secrete IF | No (stomach usually spared) | | Transit through small bowel | Duodenum, jejunum | Passive transit | Possibly, if inflamed | | **Absorption of IF–B12 complex** | **Terminal ileum** | **Specific receptor-mediated uptake** | **YES — primary site of Crohn's involvement** | | Enterohepatic circulation | Ileum | Reabsorption of B12 from bile | Disrupted in Crohn's | **High-Yield:** Crohn's disease **classically affects the terminal ileum** (ileitis). This is the site of B12 absorption, making malabsorption the primary mechanism — not intrinsic factor deficiency. ## Pathophysiology of B12 Deficiency in IBD ```mermaid flowchart TD A[Crohn's disease]:::outcome --> B[Chronic inflammation of terminal ileum]:::action B --> C[Damage to ileal epithelium]:::action C --> D[Loss of IF-B12 receptor expression]:::action D --> E[Impaired B12 absorption]:::urgent E --> F[Serum B12 depletion]:::outcome F --> G[Megaloblastic anemia]:::outcome F --> H[Neurological manifestations]:::outcome H --> I[Subacute combined degeneration]:::urgent ``` ## Clinical Features Supporting B12 Deficiency 1. **Neurological signs**: Loss of vibration sense, positive Lhermitte sign → posterior/lateral column disease (subacute combined degeneration) 2. **Megaloblastic anemia**: MCV 105 fL, bone marrow shows megaloblastic erythropoiesis with giant metamyelocytes 3. **Serum B12 frankly low**: 95 pg/mL (normal >200) 4. **Serum folate normal**: 6.2 ng/mL (>5.4) — rules out pure folate deficiency 5. **Crohn's disease with terminal ileal involvement**: Classic risk factor for B12 malabsorption **Clinical Pearl:** In Crohn's disease, B12 deficiency is often **asymptomatic hematologically** but presents with **neurological symptoms first** (cognitive slowing, paresthesias, ataxia). This is because neurological damage accumulates silently and becomes apparent only when stores are severely depleted. ## Why NOT the Other Mechanisms **Intrinsic factor deficiency** (pernicious anemia): - Requires autoimmune destruction of gastric parietal cells - Associated with atrophic gastritis, not Crohn's disease - Stomach is **rarely involved** in Crohn's (usually terminal ileum) - Would require positive intrinsic factor antibodies **Folate deficiency**: - Serum folate is **normal** (6.2 ng/mL) - Folate deficiency causes megaloblastic anemia but NOT neurological manifestations - Crohn's can cause folate malabsorption, but this patient's folate is replete **Parietal cell autoimmunity**: - Not associated with Crohn's disease - Would cause pernicious anemia, not Crohn's-related B12 deficiency - No mention of autoimmune markers **Mnemonic: CROHN'S B12 — C.R.O.H.N.'S = Cobalamin Reabsorption Occurs Here; Necroinflammation Stops absorption** - The terminal ileum is the **primary site of B12 absorption** - Crohn's inflammation destroys this site → malabsorption ## Management - **IM B12 injections** (parenteral route bypasses malabsorption) - Oral B12 supplementation is ineffective in malabsorption - High-dose oral B12 (1000–2000 μg daily) may work if some ileal function remains - Treat underlying Crohn's disease (5-ASA, biologics) to reduce inflammation [cite:Harrison 21e Ch 100; Robbins 10e Ch 14] 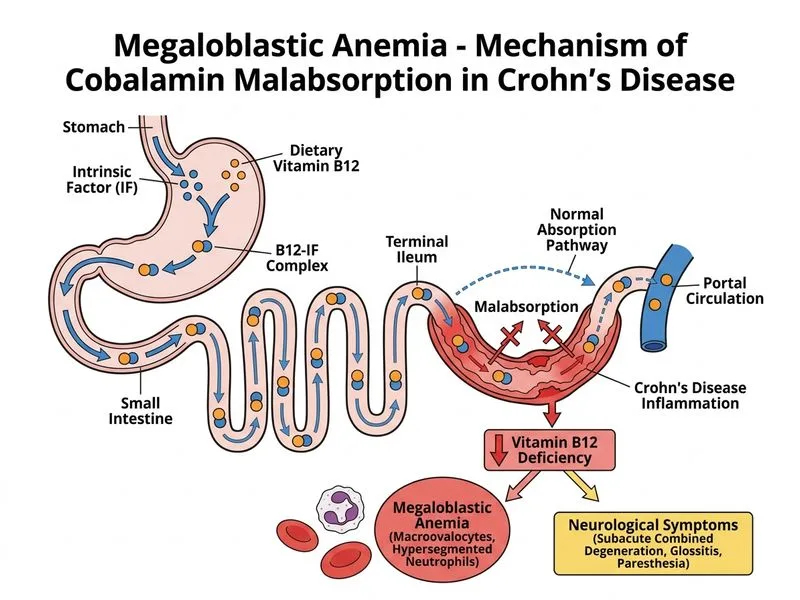
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.