## Staging Investigation for Melanoma ### Clinical Context This patient has a **Stage IIB melanoma** (Breslow thickness 2.8 mm, Clark level IV, no mention of ulceration). The critical next step is to determine regional lymph node involvement, which is the most important prognostic factor after tumour thickness. ### Why Sentinel Lymph Node Biopsy (SLNB) is Correct **Key Point:** SLNB is the investigation of choice for all melanomas with Breslow thickness ≥1 mm or Clark level ≥III, as it: - Accurately stages regional lymph nodes - Identifies occult nodal disease in 15–20% of clinically node-negative patients - Provides the most important prognostic information - Guides adjuvant therapy decisions (interferon, checkpoint inhibitors) - Has high sensitivity (>90%) and specificity (>95%) when performed by experienced teams **High-Yield:** SLNB is **mandatory** for: - Breslow thickness 1–4 mm (intermediate-risk) - Clark level IV–V - Presence of ulceration - High mitotic rate (≥1 mitosis/mm²) ### Staging Algorithm for Melanoma ```mermaid flowchart TD A[Melanoma diagnosed on biopsy]:::outcome --> B{Breslow thickness?}:::decision B -->|< 1 mm, no high-risk features| C[Clinical observation only]:::action B -->|1-4 mm OR Clark IV-V| D[Sentinel Lymph Node Biopsy]:::action B -->|> 4 mm OR palpable nodes| E[SLNB + Imaging]:::action D --> F[Node-negative?]:::decision F -->|Yes| G[Stage IIA/IIB]:::outcome F -->|No| H[Stage IIIA/IIIB/IIIC]:::outcome E --> I[Assess for distant metastases]:::action ``` ### Role of Other Investigations | Investigation | Indication | Timing | | --- | --- | --- | | **SLNB** | All intermediate/high-risk melanomas | After primary excision | | **Chest X-ray + Abdomen US** | Baseline imaging if node-positive or thick (>4 mm) | After SLNB result | | **MRI of primary site** | Not routine; consider for desmoplastic or neurotropic variants | Rarely needed | | **PET-CT** | Only if clinical/radiological evidence of stage III/IV disease | Not for staging stage II | **Clinical Pearl:** In stage IIB melanoma, SLNB changes management in ~15–20% of patients by identifying occult nodal disease, potentially upgrading them to stage III and justifying adjuvant systemic therapy. **Warning:** Do NOT order whole-body imaging (PET-CT, brain MRI) for asymptomatic stage II melanoma — the yield is <5% and is not cost-effective. Imaging is reserved for stage III (node-positive) or symptomatic patients. 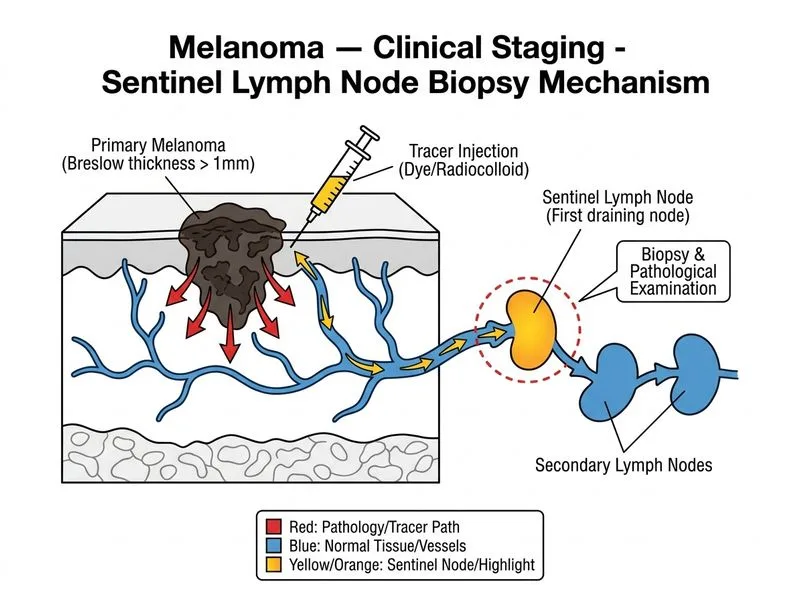
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.