## Diagnosis of Suspected Nodal Melanoma Recurrence ### Clinical Scenario This patient has a **recurrent melanoma** presenting as a solitary axillary node 2 years after primary treatment. Confirmation of melanoma metastasis is essential before committing to lymphadenectomy and adjuvant systemic therapy. ### Why Ultrasound-Guided Core Needle Biopsy? **Key Point:** CNB is the gold standard for diagnosing nodal metastases in melanoma. It provides adequate tissue for histopathology, immunohistochemistry (IHC), and molecular testing (BRAF, NRAS mutations) to guide targeted therapy. ### Advantages of CNB Over Alternatives | Feature | FNAC | CNB | Excisional Biopsy | |---|---|---|---| | **Diagnostic accuracy** | 60–70% | 90–95% | 100% (but invasive) | | **Tissue for IHC** | Limited | Adequate | Adequate | | **Molecular testing** | Poor | Good | Good | | **Morbidity** | Minimal | Minimal | Lymphedema risk, surgical delay | | **Cost** | Low | Moderate | High | | **Ultrasound guidance** | Possible | Standard | Not applicable | **High-Yield:** CNB under ultrasound guidance allows: 1. Real-time visualization and precise needle placement 2. Multiple passes for adequate cellularity 3. Immunohistochemistry for **S100** (sensitive, 95%), **HMB-45** (specific, 80%), and **Melan-A** (sensitive and specific) 4. BRAF V600E mutation testing → eligibility for targeted therapy (vemurafenib, dabrafenib) 5. PD-L1 expression assessment → eligibility for checkpoint inhibitors (pembrolizumab, nivolumab) ### Diagnostic Criteria for Melanoma Metastasis **Clinical Pearl:** Histopathology shows: - Nests of atypical melanocytes within lymph node parenchyma - Increased mitotic activity - Loss of maturation (cytologic atypia persists toward hilum) - IHC: S100+, HMB-45+, Melan-A+ **Mnemonic:** **SHIM** — **S**100, **H**MB-45, **I**mmunostaining, **M**elanoma confirmation. ### Why Not the Other Options? **Option 0 (FNAC):** - Sensitivity only 60–70% for nodal metastases - Insufficient tissue for IHC and molecular testing - Cannot reliably distinguish melanoma from reactive hyperplasia or benign nevi - Higher false-negative rate; may delay diagnosis **Option 2 (Excisional biopsy):** - Unnecessarily invasive for diagnostic purposes - Risk of lymphedema if node is in axilla (surgical dissection) - Delays systemic therapy initiation - Reserved for therapeutic lymphadenectomy after CNB confirmation **Option 3 (PET-CT followed by observation):** - PET-CT has limited sensitivity for small nodal metastases (<1 cm) - Observation without tissue diagnosis is unacceptable; delays treatment - Cannot assess BRAF/NRAS status or PD-L1 expression - Misses opportunity for targeted or immunotherapy planning ### Management Algorithm After CNB ```mermaid flowchart TD A[Axillary nodule suspected melanoma]:::outcome --> B[Ultrasound-guided CNB]:::action B --> C{Histology + IHC}:::decision C -->|Melanoma confirmed| D[BRAF/NRAS testing]:::action D --> E{Mutation status?}:::decision E -->|BRAF V600E+| F[Targeted therapy: Vemurafenib/Dabrafenib]:::action E -->|WT or NRAS+| G[Immunotherapy: Pembrolizumab/Nivolumab]:::action E -->|Adjuvant only| H[Consider lymphadenectomy + adjuvant]:::action C -->|Benign/reactive| I[Clinical surveillance]:::outcome ``` 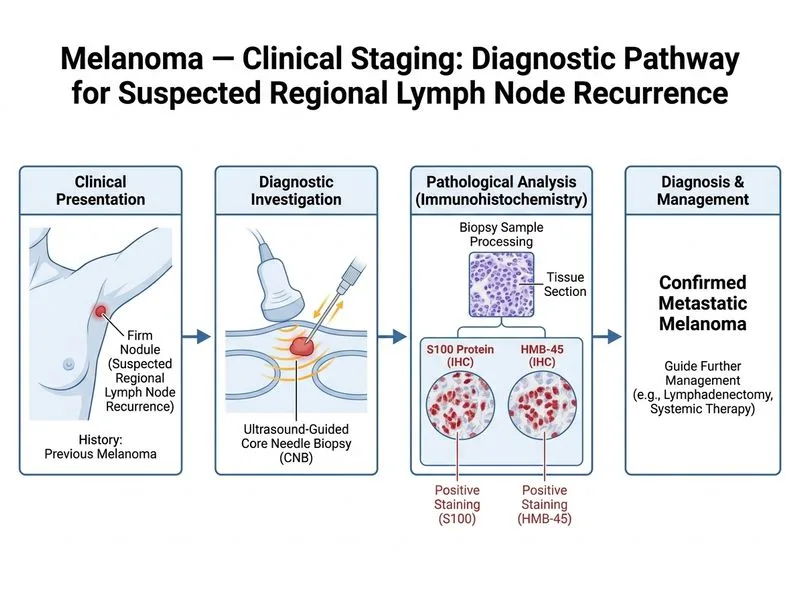
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.