## Investigation of Choice for Melanoma Diagnosis **Key Point:** Excisional biopsy with adequate margins is the gold standard for diagnosing melanoma and determining histological subtype, Breslow thickness, mitotic rate, and ulceration status — all critical prognostic factors. ### Why Excisional Biopsy? 1. **Diagnostic accuracy**: Provides full-thickness specimen allowing complete histological evaluation 2. **Prognostic assessment**: Enables measurement of Breslow thickness (most important prognostic factor) 3. **Margin assessment**: Determines adequacy of excision in one procedure 4. **Subtype classification**: Allows identification of superficial spreading, nodular, lentigo maligna, or acral lentiginous melanoma ### Breslow Thickness — Key Prognostic Factor | Thickness | 5-Year Survival | Stage | |-----------|-----------------|-------| | < 1.0 mm | 95% | IA | | 1.0–2.0 mm | 80–90% | IB–IIA | | 2.0–4.0 mm | 60–75% | IIB–IIC | | > 4.0 mm | < 50% | III–IV | **High-Yield:** Excisional biopsy is recommended with 2–3 mm margins for suspected melanoma (not punch or shave biopsy, which may miss depth assessment). **Clinical Pearl:** Once melanoma is confirmed, sentinel lymph node biopsy (SLNB) is performed for staging in tumors ≥ 1 mm Breslow thickness or with high-risk features (ulceration, high mitotic rate). ### Other Investigations — Supportive Roles - **Dermoscopy**: Aids clinical suspicion but cannot replace histology - **Punch/shave biopsy**: Inadequate for depth measurement; risks understaging - **FNAC**: Poor sensitivity; not recommended for melanoma - **RCM**: Emerging technology; not yet standard for diagnosis [cite:Robbins 10e Ch 25] 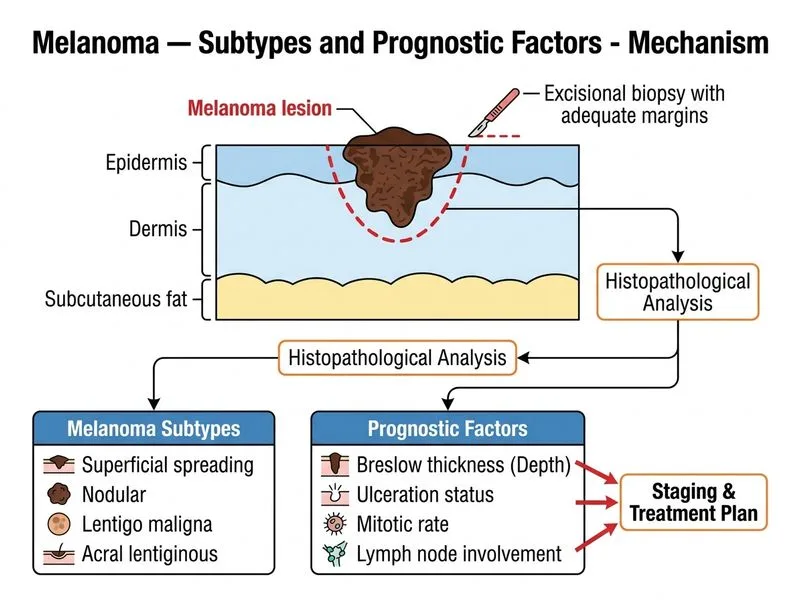
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.