## Investigation of Choice for Melanoma Diagnosis ### Role of Excisional Biopsy **Key Point:** Excisional biopsy with full-thickness histopathological examination is the gold standard for diagnosing melanoma and determining critical prognostic factors. ### Why Histopathology is Essential Histopathological examination provides: 1. **Definitive diagnosis** — Confirms melanoma vs. benign nevus 2. **Breslow thickness** — Most important prognostic factor; measured in millimeters from granular layer to deepest tumor cell 3. **Clark level** — Depth of invasion relative to skin layers (I–V) 4. **Ulceration** — Present/absent; worsens prognosis significantly 5. **Mitotic rate** — Number of mitoses per mm²; high rate indicates poor prognosis 6. **Margin assessment** — Ensures adequate clearance 7. **Lymphovascular invasion** — Predicts nodal metastasis risk **High-Yield:** Breslow thickness >4 mm, presence of ulceration, and high mitotic rate (≥1/mm²) are the three strongest independent prognostic factors in melanoma. ### Excisional vs. Incisional Biopsy | Feature | Excisional | Incisional | |---------|-----------|----------| | **Recommended for** | All suspicious pigmented lesions | Large lesions where excision not feasible | | **Margin clearance** | Assessed | Not assessed | | **Breslow thickness** | Accurate | May be underestimated | | **Staging accuracy** | Complete | Incomplete | **Clinical Pearl:** Incisional or punch biopsy should be avoided for suspected melanoma because sampling error may miss the deepest (thickest) portion, leading to understaging. ### Timing of Staging Investigations Once melanoma is confirmed histologically: - **Stage I–II (Breslow ≤4 mm, no ulceration):** Clinical examination + optional sentinel lymph node biopsy - **Stage III (nodal involvement):** Sentinel lymph node biopsy - **Stage IV (metastatic):** CT chest/abdomen/pelvis ± PET-CT **Mnemonic:** **BUMP** — **B**reslow thickness, **U**lceration, **M**itotic rate, **P**rognostic factors all determined by histopathology. 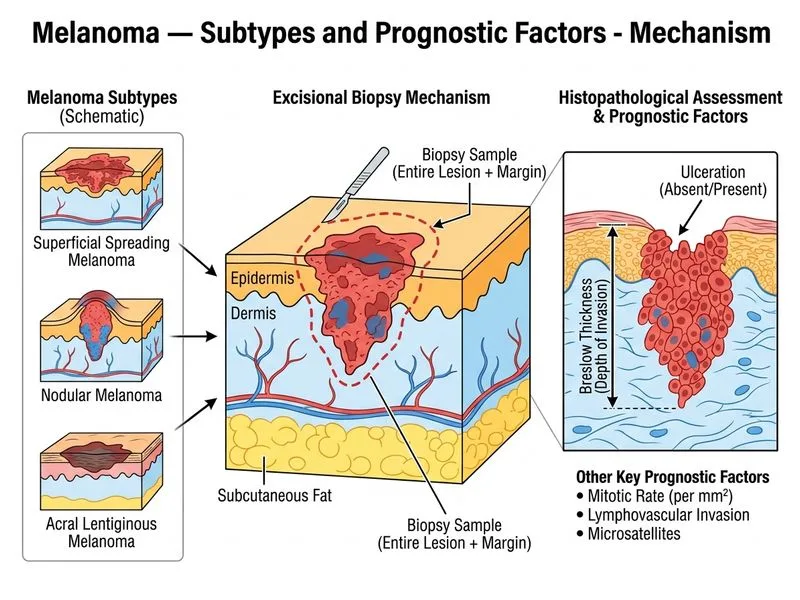
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.