## Staging Investigation for Intermediate-Risk Melanoma ### Risk Stratification and Breslow Thickness **Key Point:** Breslow thickness is the single most important prognostic factor in melanoma and determines the need for sentinel lymph node biopsy (SLNB). ### Breslow Thickness Classification | Breslow Thickness | Stage | Risk of Nodal Metastasis | SLNB Indicated? | |-------------------|-------|--------------------------|----------------| | ≤1.0 mm | IA | <5% | No | | 1.01–2.0 mm | IB | 5–10% | Consider | | 2.01–4.0 mm | IIA–IIB | 10–25% | **Yes** | | >4.0 mm | IIC | >25% | **Yes** | | Any thickness + ulceration | IB–IIC | Increased | **Yes** | **High-Yield:** Breslow thickness 2.8 mm places this patient in stage IIA (intermediate-risk) melanoma, where SLNB is recommended to assess occult nodal disease and guide adjuvant therapy decisions. ### Sentinel Lymph Node Biopsy: Indications & Technique 1. **Indications:** - Breslow thickness 1.0–4.0 mm (intermediate-risk) - Breslow >4.0 mm (high-risk) - Ulceration present - High mitotic rate (≥1/mm²) - Lymphovascular invasion 2. **Technique:** - Intradermal injection of radioactive tracer (technetium-99m) and blue dye near primary tumor - Lymphoscintigraphy to identify sentinel node(s) - Intraoperative gamma probe and visual identification - Histopathological examination (including immunohistochemistry for S-100, Melan-A) 3. **Prognostic value:** - Sentinel node positivity → Stage III (nodal disease) → Adjuvant therapy (nivolumab, pembrolizumab, or interferon-α) - Sentinel node negativity → Stage II → Observation or adjuvant therapy based on other risk factors **Clinical Pearl:** SLNB is both diagnostic (identifies occult nodal disease) and prognostic (upstages 15–20% of clinically node-negative intermediate-risk melanomas), making it essential for treatment planning. ### Why Other Investigations Are Not Appropriate ```mermaid flowchart TD A[Melanoma diagnosed]:::outcome --> B{Breslow thickness?}:::decision B -->|≤1.0 mm| C[Stage I<br/>No SLNB]:::action B -->|1.01-4.0 mm| D[Stage II<br/>Consider/perform SLNB]:::action B -->|>4.0 mm| E[Stage III/IV<br/>SLNB + staging CT]:::action C --> F[Clinical follow-up]:::action D --> G[SLNB for nodal staging]:::action E --> H[SLNB + Imaging<br/>CT/PET-CT]:::action G --> I{SLNB positive?}:::decision I -->|Yes| J[Adjuvant systemic therapy]:::action I -->|No| K[Observation ± adjuvant]:::action ``` **Mnemonic:** **SLNB for Stage II** — Sentinel Lymph Node Biopsy is the staging investigation of choice for intermediate-risk (Breslow 1–4 mm) melanoma. 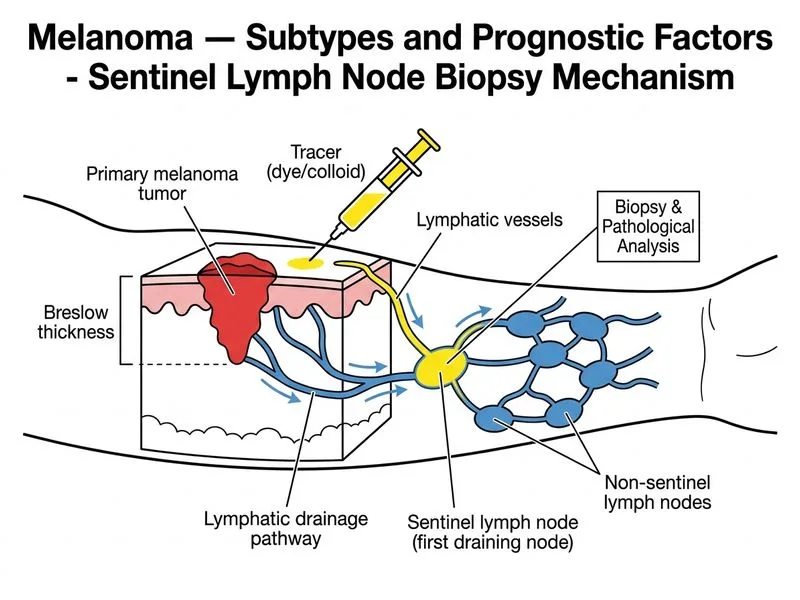
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.