## Clinical Assessment This patient presents with a clinically suspicious melanoma based on ABCDE criteria (Asymmetry, irregular Border, Color variation, Diameter >6 mm, Evolving). The next step is tissue diagnosis via excisional biopsy. ## Management Algorithm for Suspected Melanoma ```mermaid flowchart TD A[Clinically suspicious pigmented lesion]:::outcome --> B{Diagnosis confirmed?}:::decision B -->|No| C[Excisional biopsy with narrow margins]:::action C --> D[Histopathology: Breslow thickness, mitotic rate, ulceration]:::outcome D --> E{Breslow thickness & stage?}:::decision E -->|≤1 mm, no ulceration| F[Wide local excision 1 cm margin]:::action E -->|1-4 mm or high-risk features| G[Wide local excision 2 cm margin + SLNB consideration]:::action E -->|>4 mm or stage III/IV| H[Wide local excision 2-3 cm + SLNB + staging]:::action ``` ## Key Point: **Excisional biopsy is the gold standard for diagnosis of suspected melanoma.** It must include the full thickness of the lesion (dermis) and a narrow margin (2 mm) of normal skin to allow accurate histopathological assessment of Breslow thickness, mitotic rate, ulceration, and Clark level — all critical prognostic factors. ## High-Yield: - **Excisional biopsy** is diagnostic AND therapeutic for lesions <2 cm - Histopathology determines Breslow thickness, which is the **single most important prognostic factor** in melanoma - Sentinel lymph node biopsy (SLNB) is indicated AFTER diagnosis and staging, not before - Staging investigations (CT/PET) are reserved for stage IB or higher (Breslow >1 mm with ulceration, or ≥2 mm) ## Clinical Pearl: **Do not delay tissue diagnosis with imaging.** Systemic staging is performed only after histological confirmation and risk stratification based on Breslow thickness. ## Mnemonic: **ABCDE of melanoma** — Asymmetry, Border irregularity, Color variation, Diameter >6 mm, Evolving (changing). 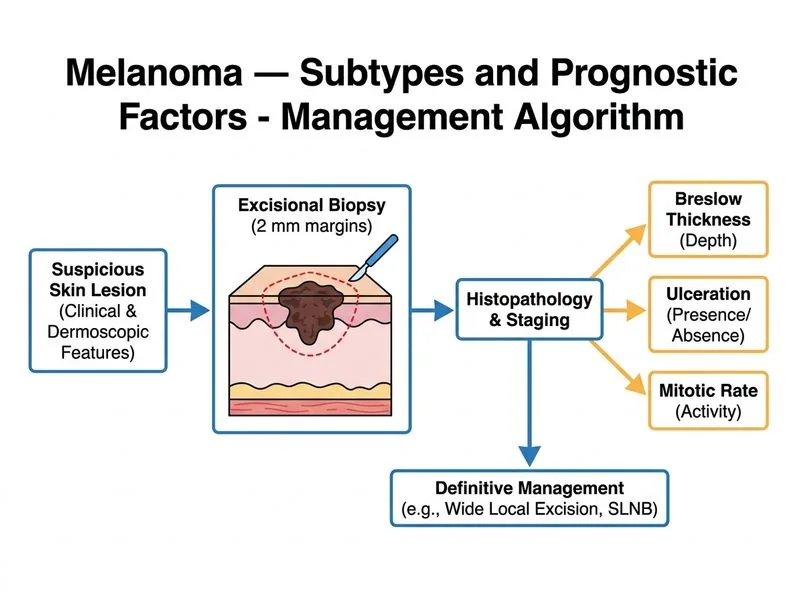
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.