## Prognostic Stratification This patient has a **stage IIB melanoma** based on Breslow thickness (3.5 mm) and high mitotic rate (8/mm²) without ulceration. This is an intermediate-to-high-risk lesion requiring staging and consideration of adjuvant therapy. ## Melanoma Staging by Breslow Thickness and Ulceration | Breslow Thickness | No Ulceration | With Ulceration | |---|---|---| | ≤1 mm | Stage IA | Stage IB | | 1.01–2 mm | Stage IB | Stage IIA | | 2.01–4 mm | Stage IIA | Stage IIB | | >4 mm | Stage IIB | Stage IIC | **This patient: 3.5 mm, no ulceration = Stage IIA; with 8 mitotic figures/mm² (high risk) = Stage IIB equivalent.** ## Management Algorithm for Stage IIB Melanoma ```mermaid flowchart TD A[Stage IIB melanoma: Breslow 3.5 mm, no ulceration, high mitotic rate]:::outcome --> B[SLNB indicated?]:::decision B -->|Yes: Breslow ≥1 mm or high-risk features| C[Sentinel Lymph Node Biopsy]:::action C --> D{SLNB positive?}:::decision D -->|Negative| E[Staging: CT chest/abdomen/pelvis]:::action D -->|Positive| F[Complete lymph node dissection + staging]:::action E --> G[Consider adjuvant therapy based on stage]:::action F --> G G --> H[Nivolumab or pembrolizumab if stage III]:::action ``` ## Key Point: **SLNB is indicated for melanomas with Breslow thickness ≥1 mm OR high-risk features (ulceration, high mitotic rate, young age, lymphovascular invasion).** This patient meets both criteria and requires SLNB for accurate staging and prognostic information. ## High-Yield: - **Breslow thickness** is the single most important prognostic factor - **SLNB is staging, not therapeutic** — it does not improve survival but provides critical prognostic information - **Adjuvant immunotherapy (nivolumab, pembrolizumab)** is indicated for stage III melanoma (node-positive) and improves recurrence-free survival - **Interferon-alpha** is largely replaced by checkpoint inhibitors in modern practice - **Re-excision** is not indicated if margins are already clear ## Clinical Pearl: **High mitotic rate (≥1/mm²) is an independent adverse prognostic factor** and strengthens the indication for SLNB even in thinner lesions. This patient's 8 mitotic figures/mm² is significantly elevated and warrants complete staging. ## Mnemonic: **SLNB Indications (Breslow ≥1 mm OR any of these):** - **U**lceration present - **M**itotic rate ≥1/mm² - **L**ymphatic invasion - **Y**oung age (<40 years) - **C**lark level IV–V 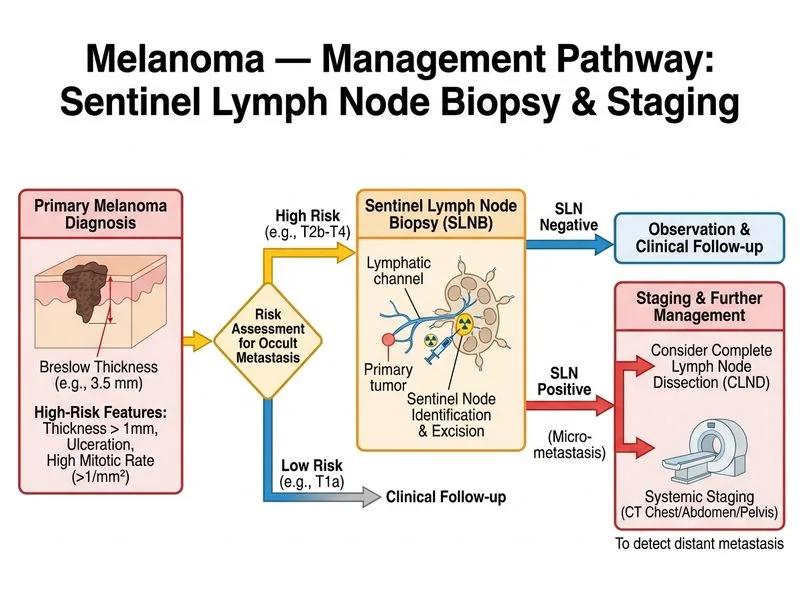
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.