## Diagnosis: Nodular Melanoma with Adverse Prognostic Factors ### Clinical and Histopathologic Features of Nodular Melanoma **Key Point:** Nodular melanoma is characterized by rapid growth, a raised/nodular appearance, lack of a significant radial growth phase, and predominantly vertical (dermal/subcutaneous) invasion. ### Why This Case is Nodular Melanoma 1. **Rapid growth:** 3-month history (vs. years for LMM or SSM) 2. **Raised, nodular appearance:** Classic presentation 3. **Minimal intraepidermal component:** Predominantly dermal/subcutaneous invasion 4. **Homogeneous dermoscopic pattern:** Lacks the architectural detail of SSM or reticular pattern of LMM 5. **Ulceration and brisk mitotic activity:** Signs of aggressive behavior ### AJCC Prognostic Factors in Melanoma | Prognostic Factor | Impact on Prognosis | Breslow Thickness Correlation | |-------------------|-------------------|-------------------------------| | **Breslow thickness** | Most important independent predictor | > 4 mm = Stage IIIB/C | | **Mitotic rate** | High rate (≥ 1/mm²) = worse prognosis | Incorporated into T stage | | **Ulceration** | Upstages lesion by one T category | Present in 10–15% of melanomas | | **Clark level** | Less important than Breslow | Mainly historical | | **Lymphovascular invasion** | Associated with worse outcome | Indicates higher risk | **High-Yield:** Breslow thickness > 4 mm is the single most powerful prognostic factor in this case. It places the patient at high risk for lymph node involvement and distant metastasis (5-year survival ~50%). ### Mnemonic for Melanoma Subtypes: **"SLNA"** **S** = Superficial Spreading (most common, intermediate prognosis) **L** = Lentigo Maligna (sun-exposed, best prognosis) **N** = Nodular (worst prognosis, rapid) **A** = Acral Lentiginous (worst prognosis, late diagnosis) ### Why Nodular Melanoma Has Worst Prognosis **Clinical Pearl:** Nodular melanoma lacks a prolonged radial growth phase, allowing rapid invasion into the dermis and subcutis before clinical detection. This results in thick lesions at diagnosis and higher rates of lymph node involvement. ### Breslow Thickness Staging ```mermaid flowchart TD A[Melanoma]:::outcome --> B{Breslow Thickness}:::decision B -->|< 0.8 mm| C[Stage IA]:::outcome B -->|0.8-1.0 mm| D[Stage IB]:::outcome B -->|1.01-2.0 mm| E[Stage IIA]:::outcome B -->|2.01-4.0 mm| F[Stage IIB/IIC]:::outcome B -->|> 4.0 mm| G[Stage IIIB/C]:::urgent G --> H[High risk: SLN biopsy + adjuvant therapy]:::action ``` **Key Point:** A Breslow thickness of 4.2 mm places this patient at Stage IIIB/C and mandates sentinel lymph node biopsy and consideration of adjuvant immunotherapy (interferon or checkpoint inhibitors). [cite:Robbins 10e Ch 25] 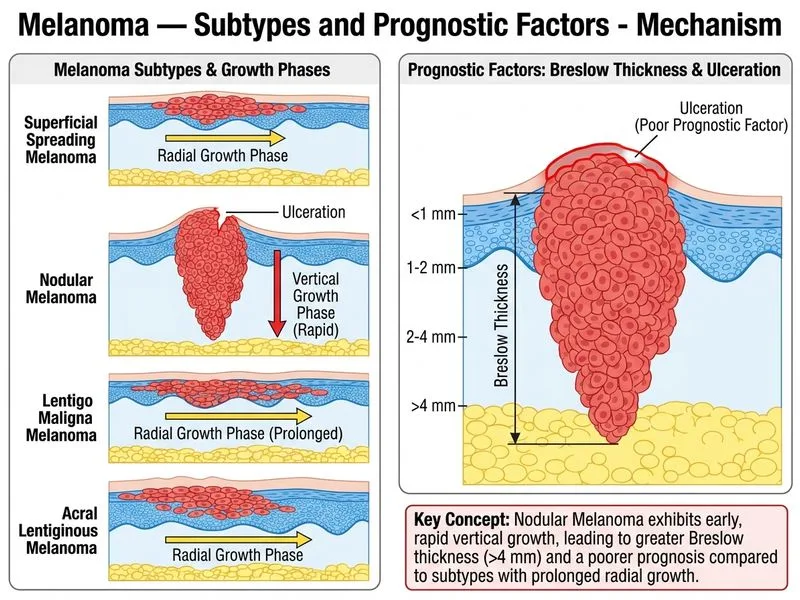
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.