## Prognostic Indicators in Cutaneous Melanoma ### Current AJCC Staging and Prognostic Factors **Key Point:** According to the **AJCC 8th Edition (2017)** and standard dermatology/oncology references (Fitzpatrick's Dermatology, Harrison's Principles of Internal Medicine), **Breslow thickness** is the **single most important and most accurate prognostic indicator** for localized cutaneous melanoma. ### Breslow Thickness — The Primary Prognostic Factor Breslow thickness (measured in millimeters from the granular layer to the deepest invasive tumor cell) directly correlates with risk of metastasis and overall survival: | Breslow Thickness | 5-Year Survival | AJCC T Category | |---|---|---| | ≤ 1.0 mm | ~95% | T1 | | 1.01–2.0 mm | ~85–90% | T2 | | 2.01–4.0 mm | ~70–80% | T3 | | > 4.0 mm | ~50–60% | T4 | In this patient, Breslow thickness of **1.8 mm** places the tumor in the **T2 category**, and this single measurement is the most accurate and reproducible prognostic indicator available. ### Why Not Clark Level Combined with Mitotic Rate (Option A)? **Clinical Pearl:** Clark level was historically used as a prognostic factor but has been **removed as a standalone or combined primary prognostic criterion** in the AJCC 8th Edition. Clark level is now only used as a secondary criterion for T1 melanomas (≤ 1 mm) when mitotic rate cannot be assessed. Combining Clark level with mitotic rate does **not** constitute the most accurate prognostic indicator — Breslow thickness alone outperforms this combination in reproducibility and prognostic accuracy. Mitotic rate is an important **modifier** (particularly for T1 lesions) but does not replace or outperform Breslow thickness as the primary prognostic factor. ### Why Not Diameter and Color Variegation (Option B)? Diameter and color variegation are components of the **ABCDE clinical detection criteria** and are useful for identifying suspicious lesions. However, once histopathology is available, these clinical features are **not independent prognostic factors** and do not predict survival or metastatic risk. ### Why Not Atypical Nevi History (Option C)? A history of atypical (dysplastic) nevi is a **risk factor** for developing melanoma (phenotypic marker) but has **no prognostic value** for an already-established melanoma. It does not influence staging, survival, or treatment decisions. ### AJCC 8th Edition Summary for This Case - **Breslow thickness 1.8 mm** → T2 melanoma - **Mitotic rate 3/mm²** → High-risk feature, modifies management (sentinel lymph node biopsy recommended) - **No ulceration** → Favorable modifier - **Clark level IV** → Noted but not a primary prognostic determinant per current guidelines **High-Yield:** The question asks for the **most accurate prognostic indicator** — this is unambiguously **Breslow thickness**, as established by decades of evidence and codified in AJCC staging. All other factors (mitotic rate, ulceration, Clark level) are secondary modifiers. **Reference:** Fitzpatrick's Dermatology, 9th Edition; AJCC Cancer Staging Manual, 8th Edition (2017); Harrison's Principles of Internal Medicine, 21st Edition. 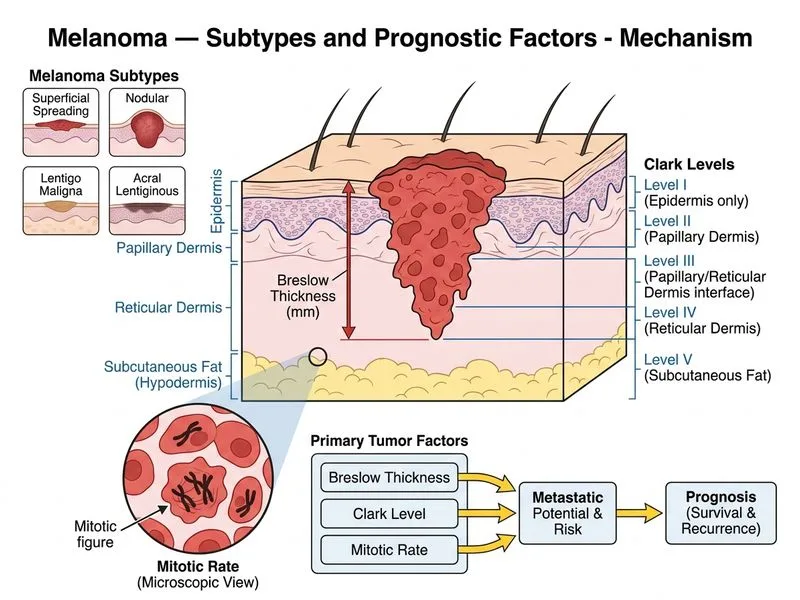
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.