## Clinical Diagnosis: MEN 1 Syndrome **Key Point:** This patient has MEN 1 (Menin mutation-associated), characterized by the **3 P's**: Parathyroid tumours (primary hyperparathyroidism), Pituitary adenomas, and Pancreatic neuroendocrine tumours. The RET mutation finding is unusual here — this should prompt clarification, but the clinical triad (primary hyperparathyroidism + prolactinoma + family history implications) is classic MEN 1. **High-Yield:** MEN 1 is autosomal dominant; **all first-degree relatives must be screened** with serum calcium, PTH, prolactin, and genetic testing. Early identification allows preventive surgery and surveillance. ### Management Algorithm ```mermaid flowchart TD A[MEN 1 Diagnosis Confirmed]:::outcome --> B[Symptomatic Primary HPT?]:::decision B -->|Yes| C[Parathyroidectomy]:::action B -->|No| D[Monitor calcium, PTH] A --> E[Prolactin-secreting Adenoma?]:::decision E -->|Yes| F[Dopamine agonist or Surgery]:::action E -->|No| G[Imaging surveillance] A --> H[Screen First-Degree Relatives]:::action H --> I[Genetic counselling & RET/MENIN testing]:::action ``` ### Why This Answer 1. **Symptomatic hyperparathyroidism** (kidney stones, elevated calcium) → parathyroidectomy is indicated. 2. **Prolactinoma** → pituitary surgery or dopamine agonist; this patient needs both interventions. 3. **Genetic diagnosis** → **mandatory screening of all first-degree relatives** with biochemical tests and genetic testing. 4. This is the standard-of-care approach per international MEN 1 guidelines. **Clinical Pearl:** Parathyroidectomy in MEN 1 often requires **subtotal resection or total parathyroidectomy with autotransplantation** (not simple adenomectomy) because hyperplasia is common and recurrence rates are high (up to 50% at 10 years). [cite:Harrison 21e Ch 397] 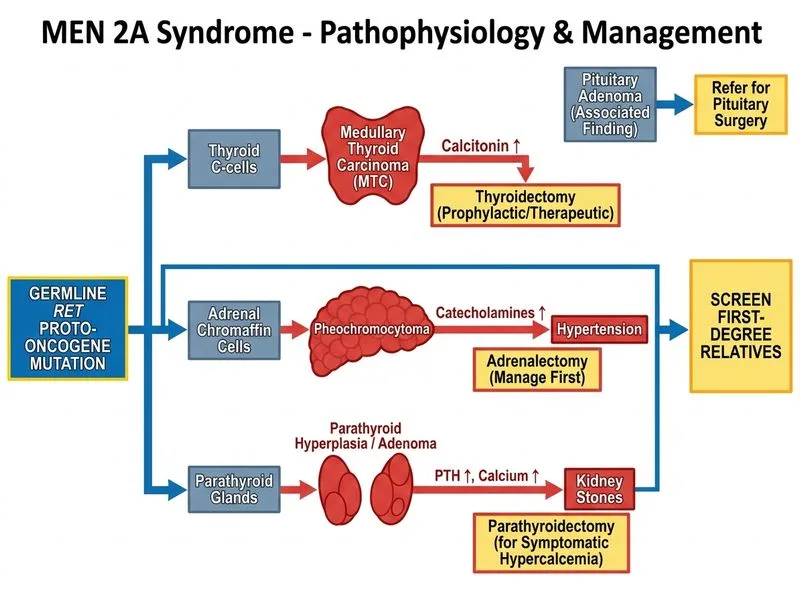
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.