## Diagnosis: Meniere Disease ### Clinical Presentation This patient presents with the classic tetrad of Meniere disease: **Key Point:** The four cardinal features are: 1. Episodic vertigo (20 min to several hours) 2. Fluctuating sensorineural hearing loss (low frequencies initially) 3. Tinnitus 4. Aural fullness (sensation of pressure in the ear) ### Audiometric Findings **High-Yield:** Early Meniere disease shows sensorineural hearing loss at **low frequencies (500–1000 Hz)**, which is pathognomonic. This contrasts with noise-induced or age-related hearing loss, which affects high frequencies first. ### Vestibular Findings **Clinical Pearl:** The horizontal nystagmus with fast component toward the right (away from the affected left ear) is consistent with left-sided vestibular hypofunction. Caloric testing showing reduced response on the left confirms peripheral vestibular involvement. ### Pathophysiology **Key Point:** Meniere disease results from endolymphatic hydrops—abnormal accumulation of endolymph within the membranous labyrinth. This causes: - Distortion of the basilar membrane (hearing loss) - Displacement of the cupula (vertigo) - Increased pressure sensation (aural fullness) ### Diagnostic Criteria (Modified Diagnostic Criteria for Meniere Disease) | Feature | Meniere Disease | BPPV | Acoustic Neuroma | |---------|-----------------|------|------------------| | **Vertigo duration** | 20 min–several hrs | Seconds to minutes | Rarely vertigo | | **Hearing loss** | Fluctuating, low-freq | Normal | Progressive, high-freq | | **Tinnitus** | Present | Absent | Often unilateral | | **Aural fullness** | Yes | No | No | | **Nystagmus** | Horizontal/rotatory | Positional | Rare | **Mnemonic:** FAINT = **F**luctuating hearing loss, **A**ural fullness, **I**ntermittent vertigo, **N**ystagmus, **T**innitus ### Investigations 1. **Audiometry:** Sensorineural pattern, low-frequency loss 2. **Caloric test:** Reduced vestibular response on affected side 3. **MRI:** Rules out retrocochlear pathology; may show endolymphatic hydrops on 3D-FLAIR sequences 4. **Electrocochleography (ECG):** Elevated summating potential/action potential ratio (supportive but not diagnostic) ### Management Approach ```mermaid flowchart TD A[Meniere Disease Suspected]:::outcome --> B{Acute Attack?}:::decision B -->|Yes| C[Acute Management]:::action C --> C1[Antiemetics: Prochlorperazine/Metoclopramide] C --> C2[Vestibular suppressants: Diazepam] C --> C3[Rest in dark room] B -->|No| D[Maintenance Therapy]:::action D --> D1[Dietary sodium restriction] D --> D2[Diuretics: Hydrochlorothiazide] D --> D3[Betahistine] D --> D4[Vestibular rehabilitation] A --> E{Refractory?}:::decision E -->|Yes| F[Intratympanic Gentamicin/Corticosteroids]:::action E -->|Still Refractory| G[Surgical: Endolymphatic sac decompression]:::action E -->|Severe| H[Labyrinthectomy/Vestibular neurectomy]:::urgent ``` **High-Yield:** First-line management is **conservative**: sodium restriction, diuretics (hydrochlorothiazide 25 mg daily), and betahistine (16 mg TID). Intratympanic gentamicin or corticosteroids are reserved for refractory cases. 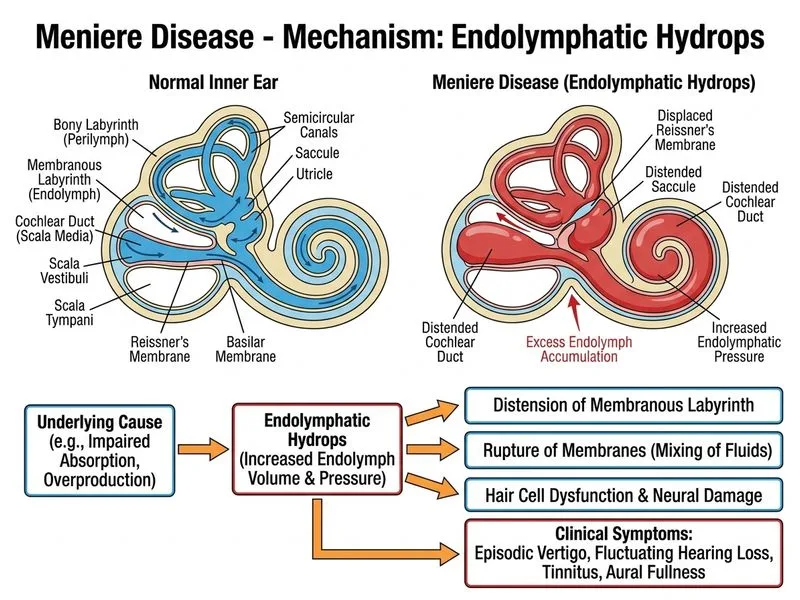
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.