## Management of Refractory Meniere Disease ### Clinical Context This patient has **refractory Meniere disease** — inadequate symptom control despite conservative therapy (dietary modification and diuretics for 3 months). The next step in the management ladder is **intratympanic pharmacotherapy**. ### Management Ladder for Meniere Disease ```mermaid flowchart TD A[Meniere Disease Diagnosed]:::outcome --> B[Step 1: Conservative Therapy]:::action B --> C[Low-salt diet, diuretics, vestibular rehab] C --> D{Response?}:::decision D -->|Good| E[Continue, monitor]:::outcome D -->|Poor| F[Step 2: Intratympanic Pharmacotherapy]:::action F --> G{Hearing preserved?}:::decision G -->|Yes| H[Intratympanic steroid or gentamicin]:::action G -->|No| I[Step 3: Ablative Surgery]:::action H --> J{Vertigo controlled?}:::decision J -->|Yes| K[Continue intratympanic therapy]:::outcome J -->|No| I I --> L[Labyrinthectomy or vestibular nerve section]:::action L --> M[Definitive symptom control]:::outcome ``` **Key Point:** The management of Meniere disease is **stepwise and symptom-driven**, not diagnosis-driven. Hearing preservation is the critical decision point at each step. ### Intratympanic Pharmacotherapy: Indications & Options | Agent | Mechanism | Efficacy for Vertigo | Hearing Risk | Use Case | |-------|-----------|----------------------|--------------|----------| | **Dexamethasone** | Anti-inflammatory; reduces endolymphatic hydrops | 60–70% | Minimal | First-line intratympanic agent; hearing preserved | | **Gentamicin** | Aminoglycoside; ablates vestibular hair cells | 80–90% | Moderate (ototoxic) | Refractory cases; hearing already compromised | | **Betahistine (oral)** | Histamine analogue; improves microcirculation | 50–60% | None | Adjunct to conservative therapy | **High-Yield:** **Intratympanic dexamethasone** is the preferred second-line agent when hearing is preserved because it controls vertigo without significant ototoxicity. **Gentamicin** is reserved for cases where hearing is already poor or vertigo is refractory to steroids. ### Why Dexamethasone Is Correct Here 1. **Hearing preserved** — the patient has no mention of hearing loss, so ototoxic gentamicin is not yet justified. 2. **Refractory to conservative therapy** — 3 months of diet and diuretics have failed; escalation is warranted. 3. **Intratympanic route** — delivers high drug concentration to the inner ear while minimizing systemic side effects. 4. **Evidence-based** — intratympanic steroids reduce vertigo frequency by 60–70% in refractory Meniere disease. **Clinical Pearl:** Intratympanic injection is performed via **myringotomy or tympanostomy tube** placement. The steroid is instilled into the middle ear, where it diffuses across the round window membrane into the perilymph and endolymph. ### Dosing & Administration - **Dexamethasone** 24 mg/mL, 0.4–0.5 mL per injection - **Frequency:** Weekly to monthly injections (typically 4 injections over 1 month) - **Onset:** Improvement may take 2–4 weeks - **Success rate:** 60–70% achieve significant vertigo reduction ### Mnemonic for Intratympanic Therapy Selection **SHAG** — **Steroids (dexamethasone) if Hearing is preserved; Ablative (gentamicin) if Hearing is already gone.** ## Why Other Options Are Incorrect ### Option 2: Immediate Labyrinthectomy **Reason:** Labyrinthectomy is a **destructive surgical procedure** that permanently ablates vestibular function. It is reserved for: - **Refractory vertigo** despite medical and intratympanic therapy - **Hearing already lost** in the affected ear (labyrinthectomy causes complete hearing loss) This patient still has preserved hearing and has not exhausted intratympanic options. Jumping to surgery is premature and violates the principle of stepwise escalation. **Clinical Pearl:** Labyrinthectomy is **contraindicated if hearing is preserved** because it causes complete sensorineural hearing loss in the operated ear. ### Option 3: Increase Diuretic Dose and Add Betahistine **Reason:** This represents a **continuation of conservative therapy**, not escalation. The patient has already failed 3 months of diet and diuretics. Simply increasing the diuretic dose or adding betahistine (which has modest efficacy, ~50–60%) is unlikely to control vertigo attacks occurring 3–4 times per week. This delays definitive treatment. ### Option 4: Vestibular Nerve Section **Reason:** Vestibular nerve section is a **highly invasive neurosurgical procedure** reserved for: - **Refractory vertigo** despite all medical, intratympanic, and ablative options - **Hearing preservation** is the goal (unlike labyrinthectomy, VNS preserves cochlear function) This patient has not yet tried intratympanic therapy. VNS is far too aggressive as a second-line intervention and carries significant morbidity (craniotomy, anesthesia risk). ## Summary Table: Escalation in Refractory Meniere Disease | Step | Intervention | Hearing Impact | When to Use | |------|--------------|----------------|-------------| | 1 | Diet, diuretics, vestibular rehab | Preserved | First-line | | 2 | Intratympanic dexamethasone | Preserved | Failed step 1 | | 2b | Intratympanic gentamicin | Ablated | Failed dexamethasone + hearing poor | | 3 | Labyrinthectomy | Ablated | Refractory + hearing already lost | | 3 | Vestibular nerve section | Preserved | Refractory + hearing must be preserved | **High-Yield:** The decision tree hinges on **hearing status**. Preserved hearing → intratympanic steroids. Lost hearing → ablative surgery (labyrinthectomy or gentamicin). 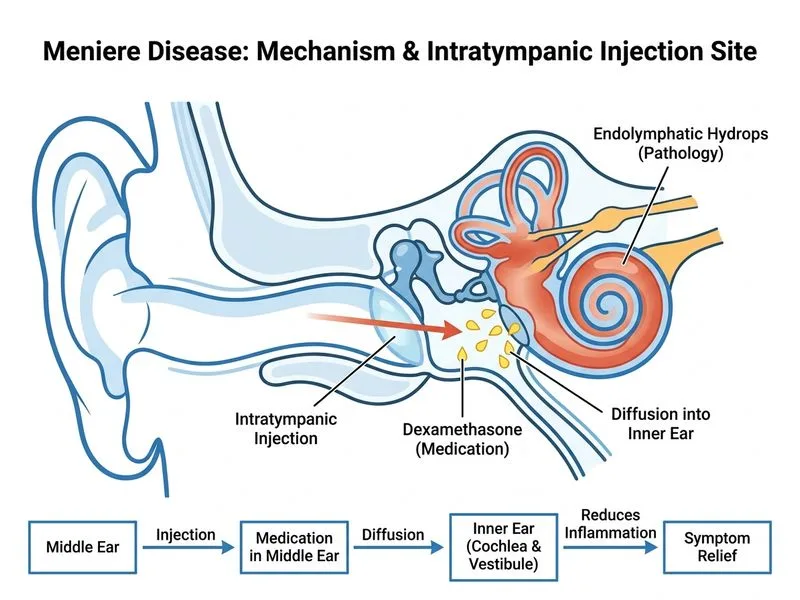
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.