## Pathophysiology of Meniere Disease **Key Point:** Endolymphatic hydrops — abnormal accumulation of endolymph within the membranous labyrinth — is the hallmark pathophysiological finding in Meniere disease. ### Mechanism The exact etiology remains unclear, but the leading hypothesis involves: 1. **Increased endolymph production** — excessive secretion by the stria vascularis 2. **Decreased endolymph reabsorption** — impaired drainage through the endolymphatic duct and sac 3. **Mechanical consequence** — distension of the membranous labyrinth (cochlea, vestibule, semicircular canals) ### Structural Consequence Endolymphatic hydrops causes: - **Cochlear dysfunction** → sensorineural hearing loss (low frequencies initially) - **Vestibular dysfunction** → vertigo, nystagmus, postural imbalance - **Rupture of Reissner membrane** → mixing of endolymph and perilymph, triggering acute attacks **High-Yield:** The triad of vertigo, fluctuating hearing loss, and tinnitus is pathognomonic for Meniere disease and directly results from endolymphatic hydrops. **Clinical Pearl:** Histopathological examination of temporal bones from Meniere patients consistently shows endolymphatic hydrops, confirming this as the primary mechanism. ### Why Other Options Are Wrong - **Ossicular discontinuity** → causes conductive hearing loss, not the fluctuating sensorineural loss of Meniere - **Oval window rupture** → presents as perilymphatic fistula with sudden hearing loss and vertigo, but not the recurrent episodic pattern of Meniere - **Vestibular neuritis** → viral inflammation causes acute vertigo but not the triad of hearing loss, tinnitus, and aural fullness characteristic of Meniere 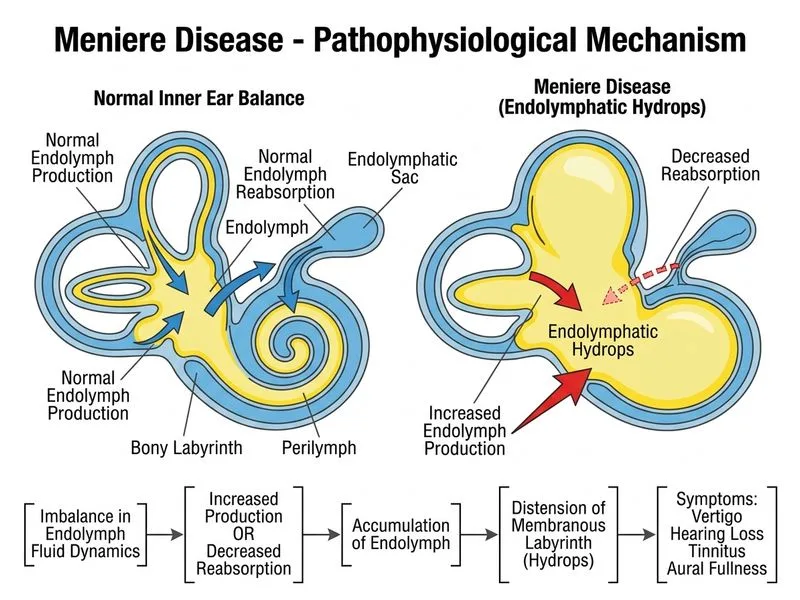
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.