## Distinguishing Follicular and Luteal Phases ### Key Structural and Hormonal Differences | Feature | Follicular Phase | Luteal Phase | |---------|-----------------|---------------| | **Duration** | ~14 days (variable) | ~14 days (fixed) | | **Dominant Structure** | Growing graafian follicle | Corpus luteum | | **Primary Hormone** | Estrogen (rising then peak) | Progesterone (elevated) | | **Endometrial State** | Proliferative | Secretory | | **Basal Body Temperature** | Lower (~36.4°C) | Higher (~36.8°C) | | **Cervical Mucus** | Abundant, clear, stretchable | Scant, thick, cellular | **Key Point:** The presence of a functional corpus luteum and sustained elevation of progesterone (>5 ng/mL) is the pathognomonic feature of the luteal phase. The corpus luteum develops only after ovulation and produces progesterone for 14 days unless pregnancy occurs. **High-Yield:** The luteal phase has a fixed duration (~14 days), whereas the follicular phase is variable. This is why cycle length variation is due to follicular phase variation, not luteal phase variation. **Clinical Pearl:** Progesterone causes the characteristic biphasic basal body temperature rise (~0.4°C) that occurs 1–2 days after ovulation — a practical marker of ovulation in infertility workup. ### Why Other Options Are Incorrect - **Rising estrogen with dominant follicle growth:** This occurs during the follicular phase, not as a distinguishing feature between phases. - **Declining FSH and rising LH:** The LH surge occurs at the transition between phases (ovulation trigger), not within a single phase. - **Endometrial proliferation and increased vascularity:** Proliferation occurs in the follicular phase; secretory changes (with increased vascularity and edema) occur in the luteal phase — not a single distinguishing feature. [cite:Ganong's Review of Medical Physiology 26e Ch 23] 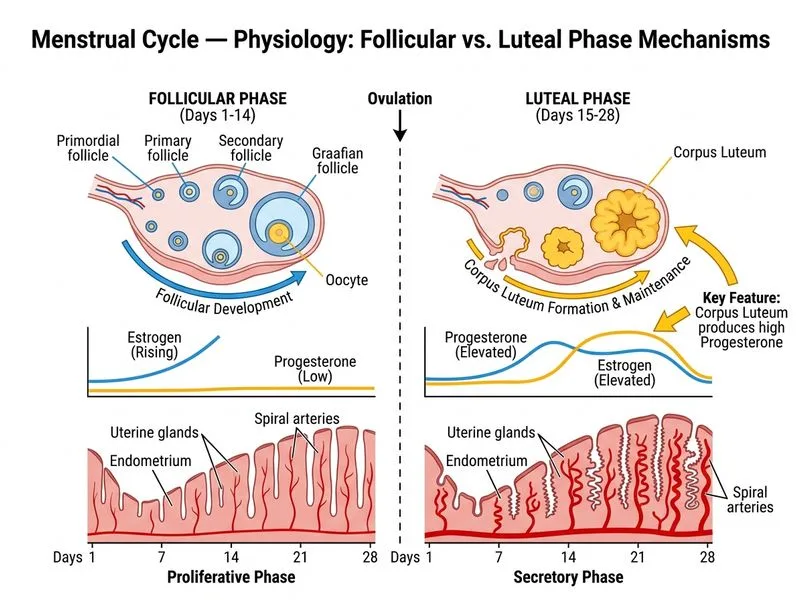
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.