## Clinical Analysis The patient presents with **irregular cycle length (21–45 days), heavy menstrual bleeding, and low progesterone on day 21 of cycle** despite being in the expected luteal phase. The key finding is a **16 mm follicle on day 21**, which indicates the follicular phase is still ongoing rather than having transitioned to the luteal phase. ### Hormonal and Ultrasound Interpretation **Key Point:** On day 21 of a normal 28-day cycle, ovulation should have occurred ~14 days prior, and the corpus luteum should be producing progesterone (5–20 ng/mL). A progesterone of 2.1 ng/mL indicates **no corpus luteum is present**. The presence of a 16 mm follicle on day 21 suggests: 1. Ovulation has **not yet occurred** in this cycle 2. The follicular phase is **prolonged** (normally 10–14 days) 3. Without ovulation, no corpus luteum forms, and progesterone remains low 4. Eventually, when the follicle regresses without ovulating, menstruation occurs (anovulatory bleeding) This pattern of **prolonged follicular phase without ovulation** is **anovulation**. ### Why Anovulation Causes Irregular Cycles **High-Yield:** Anovulatory cycles have **unpredictable duration** because: - The follicular phase is prolonged and variable (can last 21–45+ days) - No LH surge occurs, so no ovulation - No corpus luteum forms, so progesterone remains low - Endometrial proliferation continues unopposed by progesterone - Eventually, estradiol withdrawal or endometrial breakdown triggers bleeding - The next cycle begins unpredictably **Clinical Pearl:** **Heavy menstrual bleeding in anovulatory cycles** occurs because: 1. Prolonged estrogen stimulation → thick, disorganized endometrium 2. Lack of progesterone → no secretory changes or endometrial stabilization 3. Irregular shedding → prolonged, heavy bleeding ### Differential Diagnosis | Condition | Cycle Length | Progesterone (Luteal) | Ultrasound Findings | FSH | |---|---|---|---|---| | **Anovulation (correct)** | **Irregular (21–45+ days)** | **Low (<5)** | **Persistent follicles, no CL** | **Normal** | | POF | Irregular | Low | Few/no follicles | **High (>40)** | | PCOS | Irregular | Low/normal | Multiple small follicles | Normal/high | | Luteal defect | Regular | Low | Normal CL, small | Normal | **Mnemonic:** **ANOVULATION = No Ovulation = No Corpus Luteum = No Progesterone = Irregular Cycles + Heavy Bleeding** ## Pathophysiology ```mermaid flowchart TD A[Hypothalamic-Pituitary Dysfunction]:::action --> B[Inadequate or irregular GnRH/FSH pulsatility]:::action B --> C[Follicle growth is slow and prolonged]:::action C --> D[No LH surge occurs]:::outcome D --> E[No ovulation]:::urgent E --> F[No corpus luteum formation]:::urgent F --> G[Progesterone remains low]:::urgent G --> H[Unopposed estrogen stimulation of endometrium]:::action H --> I[Heavy, prolonged, irregular bleeding]:::outcome J[Cycle length varies: 21–45+ days]:::outcome E --> J ``` **Why not the other options:** - **POF (Premature Ovarian Failure):** Would show **elevated FSH (>40 mIU/mL)**, indicating ovarian exhaustion. This patient's FSH is not mentioned as elevated, and the clinical picture is more consistent with anovulation. - **PCOS:** While PCOS can present with irregular cycles and anovulation, the ultrasound description (single 16 mm follicle) does not fit the typical PCOS pattern of **multiple (≥12) small follicles (2–9 mm) in each ovary**. - **Luteal defect:** Would require **normal ovulation** (evidenced by prior corpus luteum formation and adequate progesterone rise), followed by inadequate luteal support. Here, there is no evidence of prior ovulation in this cycle. [cite:Guyton & Hall Textbook of Medical Physiology 14e Ch 81; Harrison 21e Ch 417] 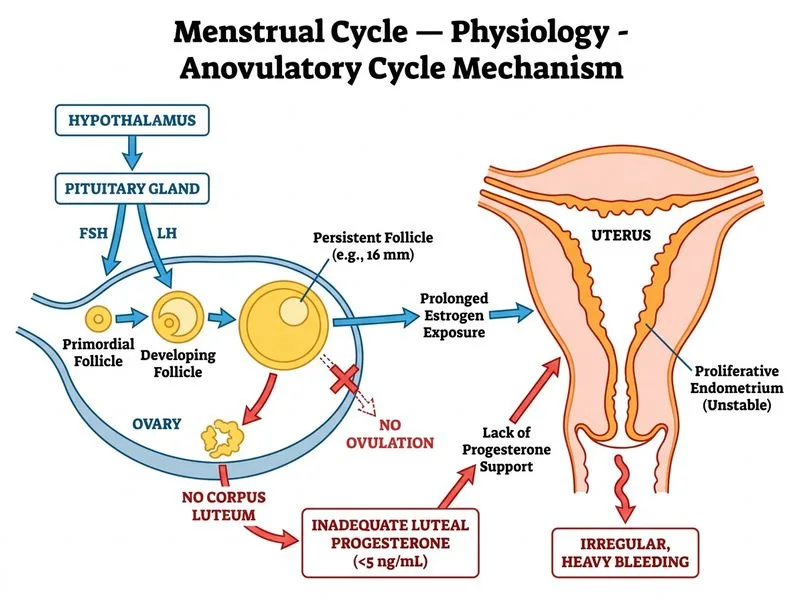
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.