## Clinical Diagnosis: Inadequate Follicular Development ### Analysis of Cycle Physiology **Key Point:** The preovulatory estradiol level of 180 pg/mL is SUBOPTIMAL (normal preovulatory peak: 200–400 pg/mL), despite regular cycles and confirmed ovulation. This indicates inadequate follicular development and estrogen production. ### Normal Follicular Phase Physiology ```mermaid flowchart TD A[Day 1: FSH surge]:::action --> B[Follicular recruitment]:::action B --> C[Granulosa cell proliferation]:::action C --> D[Aromatase activity increases]:::action D --> E[Estradiol rises progressively]:::action E --> F{Estradiol > 200 pg/mL<br/>for 48 hrs?}:::decision F -->|Yes| G[LH surge triggered]:::action F -->|No| H[Delayed/weak ovulation]:::urgent G --> I[Ovulation at 36 hrs]:::outcome H --> J[Suboptimal corpus luteum]:::urgent ``` ### Why This Patient Has Inadequate Estradiol 1. **Suboptimal follicular development:** - Estradiol 180 pg/mL is below the threshold (200 pg/mL) required for positive feedback - Indicates fewer granulosa cells or reduced aromatase activity - Smaller dominant follicle at ovulation 2. **Consequences for fertility:** - **Inadequate endometrial proliferation:** Estrogen drives endometrial thickening; low estrogen = thin endometrium - **Weak LH surge:** Subthreshold estradiol may trigger a delayed or weak LH surge - **Poor corpus luteum:** Smaller follicle → fewer luteal cells → lower progesterone production - **Impaired oocyte maturation:** Reduced estrogen may compromise meiotic competence ### Differential Diagnosis | Feature | Inadequate Estradiol | Premature LH Surge | Luteal Defect | Cervical Hostility | |---------|-------------------|------------------|--------------|-------------------| | **Preovulatory E2** | Low (<200 pg/mL) | Normal/high | Normal | Normal | | **Follicle size at ovulation** | Small (<18 mm) | Normal (18–25 mm) | Normal | Normal | | **Progesterone (day 21)** | Often low | Normal/high | Low | Normal | | **Sperm in cervical mucus** | Present (mucus quality OK) | Present | Present | Absent/immotile | | **BBT rise** | Delayed/weak | Normal | Normal | Normal | | **Mechanism** | Poor follicular growth | Premature gonadotropin surge | Corpus luteum insufficiency | Immune rejection | **Clinical Pearl:** A preovulatory estradiol <200 pg/mL is a red flag for poor follicular development, even if ovulation occurs. The oocyte from a small follicle has reduced developmental potential. ### Management Implications - **Confirm diagnosis:** Transvaginal ultrasound on day 12 to measure dominant follicle diameter (should be ≥18 mm) - **FSH stimulation:** Consider low-dose gonadotropins to enhance follicular development - **Monitoring:** Repeat estradiol and ultrasound to ensure adequate follicular growth before ovulation - **Prognosis:** With optimized follicular development, implantation and pregnancy rates improve significantly **High-Yield:** NEET PG tests the relationship between preovulatory estradiol, follicle size, and fertility. A patient with ovulation but low preovulatory estradiol has inadequate follicular development—not a luteal defect or cervical problem. 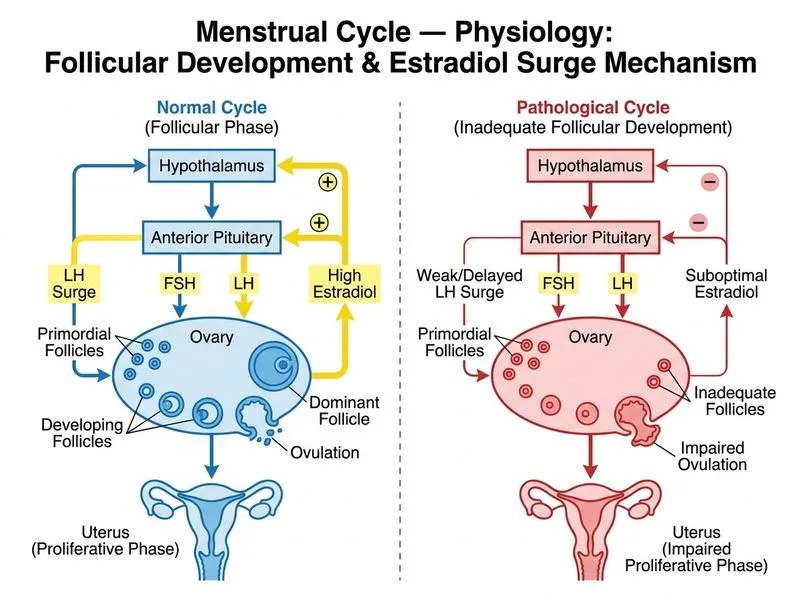
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.