## Clinical Context This patient has **secondary amenorrhea** with: - Normal FSH (rules out primary ovarian failure) - Normal prolactin (rules out hyperprolactinemia) - Normal TSH (rules out thyroid dysfunction) - **Negative progestin challenge test** (no withdrawal bleeding) The negative progestin challenge test indicates **inadequate endogenous estrogen** or **endometrial pathology**. This is a critical diagnostic finding. ## Interpretation of Progestin Challenge Test **Key Point:** The progestin challenge test distinguishes between: 1. **Adequate estrogen + normal endometrium** → withdrawal bleed occurs (positive test) 2. **Low estrogen OR endometrial pathology** → no withdrawal bleed (negative test) Since this patient's endometrium is normal on ultrasound, the negative test indicates **hypoestrogenism**. ## Diagnostic Algorithm for Hypoestrogenic Amenorrhea ```mermaid flowchart TD A[Secondary amenorrhea]:::outcome --> B[Check FSH, prolactin, TSH]:::action B --> C{All normal?}:::decision C -->|Yes| D[Progestin challenge test]:::action D --> E{Withdrawal bleed?}:::decision E -->|Yes| F[Adequate estrogen - likely anovulation]:::outcome E -->|No| G[Low estrogen - measure serum estradiol]:::action G --> H{Estradiol low?}:::decision H -->|Yes| I[Progesterone-estrogen challenge test]:::action I --> J{Withdrawal bleed?}:::decision J -->|Yes| K[Central hypogonadism - check LH, MRI pituitary]:::action J -->|No| L[Asherman syndrome or endometrial pathology]:::action H -->|No| M[Androgen excess - check testosterone, DHEA-S]:::action ``` ## Why Progesterone-Estrogen Challenge Test? **High-Yield:** The progesterone-estrogen challenge test (conjugated estrogens 1.25 mg daily × 21 days + medroxyprogesterone 10 mg daily × 5 days of estrogen) determines whether the endometrium can respond to hormones: | Test Result | Interpretation | Next Step | |-------------|----------------|----------| | **Withdrawal bleed occurs** | Endometrium is normal; amenorrhea is due to **central hypogonadism** (low LH/FSH despite normal FSH level, or inadequate pulsatile GnRH) | Check LH; consider MRI pituitary for structural lesion | | **No withdrawal bleed** | Endometrial pathology (Asherman syndrome, fibrosis) despite normal ultrasound appearance | Hysteroscopy to visualize endometrium | ## Why Not the Other Options? **Warning:** Do NOT repeat the progestin challenge with higher dose — the test result is clear and reproducible. Dose escalation does not change interpretation. | Option | Reason | |--------|--------| | **Repeat progestin challenge** | The test result is already informative. Repeating with higher dose does not change the diagnosis; it wastes time. | | **MRI pituitary immediately** | Premature. First confirm hypoestrogenism with serum estradiol and assess endometrial response with progesterone-estrogen challenge. MRI is indicated only if the challenge test is positive (suggesting central hypogonadism). | | **Start HRT and refer** | Premature and non-diagnostic. HRT masks the underlying pathology. The diagnosis must be established before treatment. | ## Clinical Pearl **The progestin-estrogen challenge test is the diagnostic bridge** between a negative progestin challenge and the identification of central vs. peripheral (endometrial) pathology. It is essential in the workup of hypoestrogenic amenorrhea. [cite:Williams Obstetrics 26e Ch 32; Yen & Jaffe's Reproductive Endocrinology 8e Ch 9] 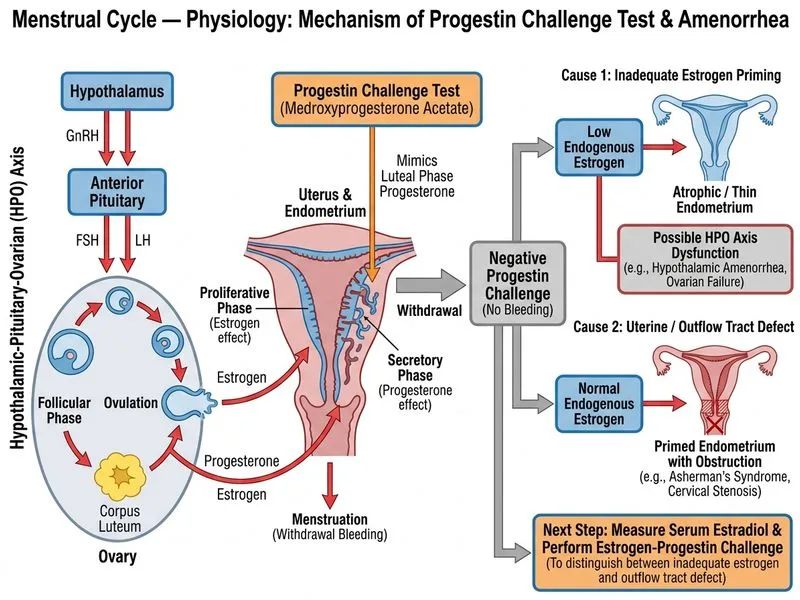
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.