## Clinical Context: Gadolinium Retention and NSF Risk A patient with advanced chronic kidney disease (eGFR 28 mL/min/1.73m²) and prior linear GBCA exposure faces cumulative gadolinium retention risk and potential nephrogenic systemic fibrosis (NSF). ## Gadolinium Retention and NSF Pathophysiology **Key Point:** Linear gadolinium-based contrast agents (GBCAs) are more prone to transmetallation and gadolinium ion release in patients with renal impairment. Gadolinium deposits in skin, bone, and organs, causing NSF in severe renal disease (eGFR <30). Gadolinium deposition is **irreversible**, and **no proven treatment exists** for established gadolinium deposition disease or NSF — chelation therapy (Option A) has not been validated as standard management and should not be routinely offered. **High-Yield:** NSF risk is highest with: - Linear GBCAs (gadodiamide, gadopentetate, gadoversetamide) - eGFR <30 mL/min/1.73m² (AKI or CKD stage 4–5) - Repeated or high-dose GBCA exposure ## Risk Stratification in This Patient | Risk Factor | Present? | Significance | |-------------|----------|---------------| | **Linear GBCA prior exposure** | Yes (gadodiamide) | Highest transmetallation risk | | **eGFR <30** | Yes (28 mL/min) | Stage 4 CKD; NSF threshold | | **Cumulative gadolinium burden** | Yes | Prior dose + proposed new dose | | **Time since prior GBCA** | 3 months | Gadolinium persists in tissues; renal clearance is negligible at this eGFR | | **Asymptomatic status** | Yes | Does NOT exclude subclinical gadolinium deposition | ## Why Each Option Is Correct or Incorrect - **Option A (Chelation therapy):** Incorrect. Chelation therapy is **not a validated or standard treatment** for gadolinium deposition or NSF. No proven pharmacological intervention reverses gadolinium tissue accumulation. This option is a distractor. - **Option B (Macrocyclic GBCA with monitoring):** Incorrect. While macrocyclic agents (gadoteridol, gadobutrol) have a lower NSF risk profile than linear agents, they are still **not recommended** when eGFR <30 and the patient has already received a linear GBCA. The cumulative gadolinium burden is the limiting factor, not just agent type. - **Option C (Macrocyclic GBCA; prior linear exposure carries no residual risk):** Incorrect. This is factually wrong. Gadolinium from linear agents persists in tissues for months to years, especially in patients with severe renal impairment. The prior exposure carries **significant residual risk**, not negligible or zero risk. - **Option D (Avoid all GBCA; use unenhanced MRI or alternative modality):** **Correct.** Per ACR guidelines, patients with eGFR <30 who have received prior linear GBCA should avoid all further GBCA exposure. Unenhanced MRI (T2-weighted sequences) is excellent for retroperitoneal fibrosis, and CT or ultrasound are viable alternatives. ## Management Algorithm **Clinical Pearl:** Once a patient with eGFR <30 has received a linear GBCA, the risk-benefit ratio of ANY future GBCA is unfavorable. Gadolinium accumulation is irreversible, NSF is incurable, and no proven treatment exists for gadolinium deposition disease. ## Recommended Imaging Alternatives - **Unenhanced MRI:** Excellent for retroperitoneal fibrosis (T2-weighted sequences show fibrous tissue as low-signal periaortic/periureteric mass) - **CT without contrast:** Useful for anatomical delineation; consider radiation dose - **Ultrasound:** First-line for renal assessment; operator-dependent **Mnemonic: AVOID-G** — Avoid gadolinium in eGFR <30, Omit linear agents, Investigate alternatives, Defer contrast if possible, Gadolinium deposits are irreversible [Cite: ACR Manual on Contrast Media 2023; ACR-ASNR Position Statement on Gadolinium Retention 2018; Radiology NSF Consensus Statement 2018; KDIGO CKD Guidelines] 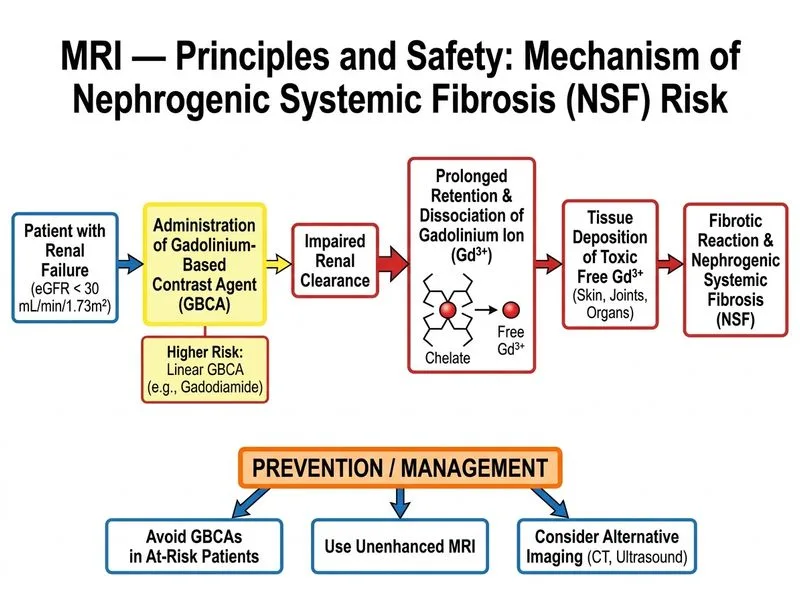
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.