## Diagnosis: Subchondral Cyst ### Clinical Context The patient has rheumatoid arthritis with imaging findings consistent with secondary osteoarthritis (joint space narrowing, marginal erosions). Subchondral cysts are common secondary findings in osteoarthritis and rheumatoid arthritis, arising from synovial fluid intrusion into bone through cartilage defects. ### MRI Characteristics of Subchondral Cyst | Feature | Subchondral Cyst | |---------|------------------| | **Location** | Immediately beneath articular cartilage (subchondral bone) | | **T1 Signal** | Low (fluid) | | **T2 Signal** | High (fluid) | | **Gadolinium Enhancement** | Peripheral rim enhancement (synovial lining) | | **Size** | Usually 0.5–2 cm | | **Associated Findings** | Joint space narrowing, cartilage loss, marginal osteophytes | ### Pathophysiology Subchondral cysts develop through: 1. Cartilage degradation and focal defects (from RA or OA) 2. Synovial fluid pressure forces fluid into subchondral bone 3. Cyst formation with peripheral synovial lining (explains rim enhancement) 4. Progressive enlargement with mechanical stress **Key Point:** The combination of **peripheral gadolinium enhancement** (synovial membrane) with **central T2 hyperintensity** (fluid) is pathognomonic for subchondral cyst. ### Why This Case Points to Subchondral Cyst - RA history → predisposes to secondary OA and cyst formation - Location: medial femoral condyle (weight-bearing, high-stress area) - Imaging: low T1, high T2, peripheral enhancement = fluid with synovial lining - Size: 1.2 cm is typical for symptomatic subchondral cyst **Clinical Pearl:** Subchondral cysts in RA can cause mechanical symptoms (locking, catching) if they expand or rupture into the joint space. [cite:Harrison 21e Ch 313] 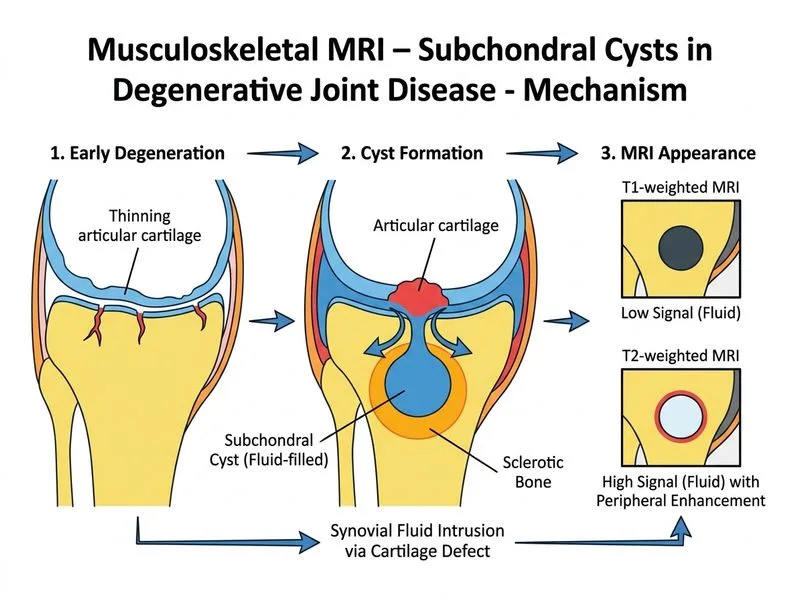
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.