## Post-MI Pericarditis and Hemorrhagic Pericardial Effusion ### Clinical Scenario: Dressler Syndrome vs. Early Post-MI Pericarditis This patient presents with pericarditis on day 5 post-MI. The timing and hemorrhagic nature of the effusion point to **early post-infarction pericarditis**, a direct consequence of myocardial necrosis. ### Pathological Mechanism **Key Point:** Post-MI pericarditis occurs when the infarct transmurally extends to the epicardium, causing inflammation and fibrin deposition on the visceral pericardium. ### Sequence of Events 1. Anterior wall MI → transmural necrosis extending to epicardium 2. Direct inflammatory response to myocardial necrosis 3. Fibrinous pericarditis develops (typically days 2–7 post-MI) 4. Pericardial effusion accumulates 5. Effusion may become hemorrhagic due to: - Inflammatory capillary injury - Bleeding from inflamed pericardial vessels - Myocardial rupture (in severe cases) ### Composition of Pericardial Fluid in Post-MI Pericarditis | Feature | Post-MI Pericarditis | Infectious Pericarditis | Dressler Syndrome | |---------|----------------------|------------------------|-----------| | **Appearance** | Hemorrhagic/serosanguineous | Purulent (bacterial) or serous (viral) | Serous to serosanguineous | | **Cell type** | Fibrin, RBCs, neutrophils | PMNs (bacterial) or lymphocytes (viral) | Lymphocytes, macrophages | | **LDH** | Elevated (myocardial origin) | Elevated (infection) | Mildly elevated | | **Troponin** | **Elevated** (leaked from infarcted myocardium) | Normal | Normal | | **Protein** | High (exudate) | High (exudate) | High (exudate) | | **Glucose** | Normal | Low (bacterial) | Normal | | **Culture** | Sterile | Positive | Sterile | | **Timing** | 2–7 days post-MI | Variable | 1–12 weeks post-MI | **High-Yield:** The presence of **elevated troponin in pericardial fluid** is pathognomonic for post-MI pericarditis because it reflects spillage of cardiac biomarkers from the adjacent infarcted myocardium. ### Clinical Features Supporting This Diagnosis - **Pericardial friction rub**: hallmark of fibrinous pericarditis - **Timing (day 5)**: classic for early post-MI pericarditis - **Hemorrhagic effusion**: reflects inflammatory capillary injury - **Diastolic right atrial collapse**: indicates tamponade physiology requiring drainage - **Anterior wall MI**: transmural infarction with epicardial involvement **Clinical Pearl:** Post-MI pericarditis is a common complication (occurring in ~5–10% of transmural MIs) and is distinct from Dressler syndrome (immune-mediated, occurs weeks to months later). Early recognition and pericardiocentesis prevent progression to tamponade. ### Management Implications - NSAIDs or colchicine for inflammation - Pericardiocentesis for hemodynamic compromise (as done here) - Avoid anticoagulation if possible (risk of hemorrhage) - Serial echocardiography to monitor effusion 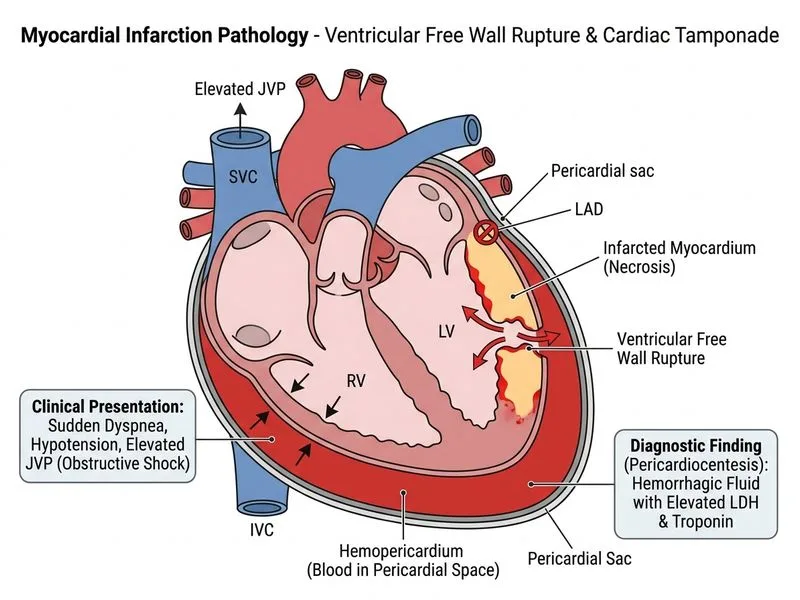
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.