## Investigation of Choice for Acute STEMI Confirmation ### Clinical Context The patient presents with classic acute STEMI features: chest pain, ST elevation on ECG in an inferior territory distribution. However, troponin is negative at 0 and 3 hours. ### Why Coronary Angiography is Correct **Key Point:** In acute STEMI with diagnostic ECG changes, coronary angiography is the gold standard investigation and serves dual purpose—diagnostic confirmation AND therapeutic intervention (primary PCI). **High-Yield:** The presence of ST elevation on ECG is sufficient to diagnose acute MI; troponin negativity at early timepoints (0–3 hours) does NOT exclude MI. Troponin rises after 3–4 hours and peaks at 24–48 hours. Waiting for troponin rise delays reperfusion therapy, which is time-critical. **Clinical Pearl:** In STEMI, the ECG diagnosis takes precedence over biomarkers. Coronary angiography should be performed urgently (within 90 minutes of first medical contact) for primary PCI, which is the preferred reperfusion strategy. ### Pathophysiology of Troponin Kinetics | Timepoint | Troponin Status | Clinical Implication | | --- | --- | --- | | 0–3 hours | Negative | May be falsely negative; do NOT delay angiography | | 3–4 hours | Begins to rise | Becomes detectable | | 24–48 hours | Peak elevation | Maximum diagnostic sensitivity | | 7–14 days | Still elevated | Remains positive; cannot date MI | ### Why Angiography Beats Other Options 1. **Diagnostic:** Directly visualizes coronary occlusion and thrombus. 2. **Therapeutic:** Enables immediate PCI and stent placement, restoring blood flow and salvaging myocardium. 3. **Prognostic:** Identifies extent of disease and collateral flow. 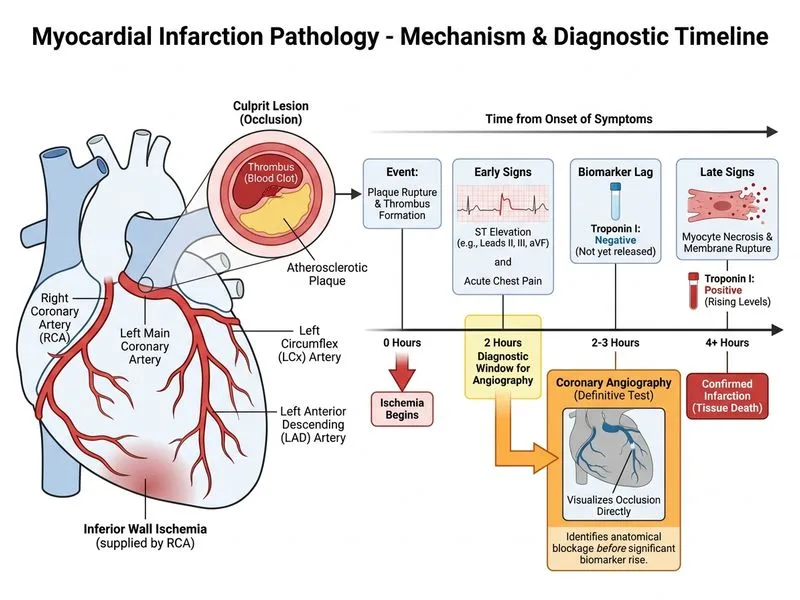
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.