## Diagnosis: Inverted Papilloma (Inverted Schneiderian Papilloma) ### Pathology & Clinical Significance **Key Point:** Inverted papilloma is a benign but locally aggressive tumor with significant malignant transformation potential (5–15% risk). The inverted growth pattern (intact epithelium overlying intact mucosa with intact respiratory epithelium) is pathognomonic. ### Defining Features of Inverted Papilloma | Feature | Inverted Papilloma | Allergic Polyps | Fungal Sinusitis | |---------|-------------------|-----------------|------------------| | **Laterality** | Unilateral (90%) | Bilateral | Often unilateral | | **Appearance** | Friable, bleeding, granular | Pale, smooth, glistening | Thick, opaque secretions | | **Histology** | Intact epithelium inverted into submucosa | Edematous mucosa with eosinophils | Fungal hyphae + eosinophilic infiltrate | | **Bone Erosion** | Yes (40–60%) | No | Yes | | **Malignant Potential** | 5–15% (SCC, adenocarcinoma) | None | Rare | | **Management** | Surgical excision + surveillance | Medical (steroids) ± FESS | Medical + antifungal ± FESS | **High-Yield:** Unilateral friable polyp + bone erosion + inverted histology = Inverted papilloma until proven otherwise. Requires aggressive surgical management and lifelong surveillance. ### Surgical Management Algorithm ```mermaid flowchart TD A[Inverted papilloma confirmed on histology]:::outcome --> B[Wide local excision with adequate margins]:::action B --> C[Remove involved periosteum and bone]:::action C --> D[Cauterize/ablate surgical bed]:::action D --> E[Endoscopic surveillance every 3-6 months for 2 years]:::action E --> F{Recurrence detected?}:::decision F -->|Yes| G[Re-excision + consider adjuvant therapy]:::action F -->|No| H[Extend surveillance intervals to annual]:::action I[Malignant transformation suspected]:::urgent --> J[Imaging + biopsy confirmation]:::action J --> K[Radical surgical resection ± radiotherapy/chemotherapy]:::urgent ``` ### Surgical Principles 1. **Wide Local Excision** — Remove tumor with 5–10 mm margin of normal mucosa 2. **Periosteal Removal** — Ablate periosteum where tumor contacted bone to reduce recurrence 3. **Complete Clearance** — Ensure no residual disease at margins 4. **Cauterization/Ablation** — Cauterize surgical bed with monopolar cautery or laser to destroy residual epithelial nests **Clinical Pearl:** Recurrence occurs in 10–30% of cases despite adequate surgery; inadequate margin clearance and failure to remove involved periosteum are the primary causes of recurrence. ### Surveillance Protocol **Key Point:** Lifelong endoscopic surveillance is mandatory because of recurrence risk and malignant transformation potential. - **Months 1–24:** Endoscopy every 3–6 months - **Year 3 onwards:** Annual endoscopy indefinitely - **Imaging:** CT or MRI at 6–12 months post-op to assess for early recurrence - **Biopsy:** Any suspicious area (bleeding, growth, color change) requires biopsy to exclude malignancy **Warning:** Do NOT observe inverted papilloma without surgery. The malignant transformation risk (5–15%) and locally aggressive nature mandate definitive surgical treatment. ### Why Radiotherapy Is Not First-Line - Radiotherapy is reserved for **recurrent, unresectable, or malignant-transformed** cases - Primary radiotherapy does not prevent recurrence and increases risk of secondary malignancy - Surgery remains the gold standard for initial management [cite:Krouse JH. Development of a staging system for inverted papilloma. Laryngoscope. 2000 Jul;110(7):1095-9. Also: Park 26e Ch 21, Harrison 21e Ch 393] 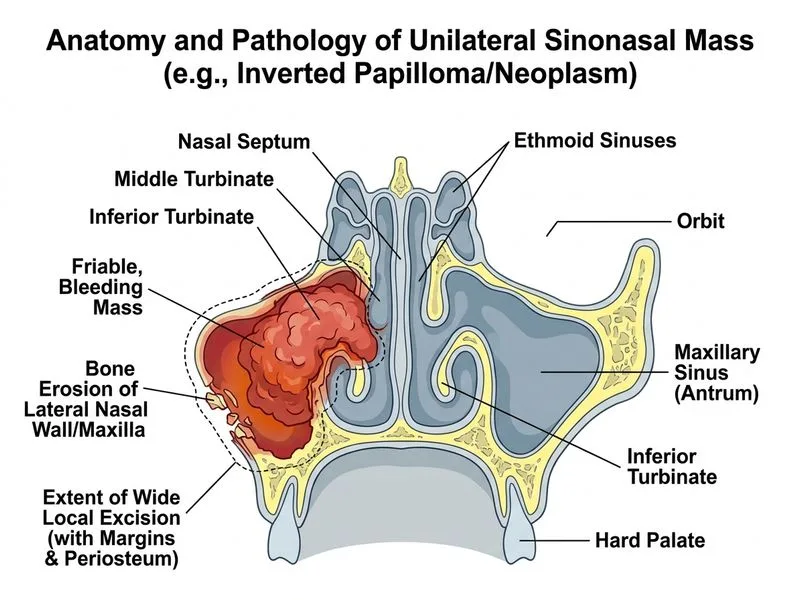
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.