## Preoperative Management of Nasopharyngeal Angiofibroma ### Clinical Context **Key Point:** This patient has a classic presentation of nasopharyngeal angiofibroma (NAF) with imaging confirmation. The next critical step is **preoperative angiographic embolization** to reduce intraoperative blood loss and improve surgical safety. ### Why Embolization Before Surgery? ### Rationale for Embolization | Aspect | Rationale | |--------|----------| | **Vascularity** | NAF is highly vascular, fed primarily by the sphenopalatine artery (branch of maxillary artery) | | **Hemorrhage risk** | Intraoperative bleeding can be life-threatening; embolization reduces blood supply by 60–80% | | **Surgical access** | Reduced bleeding improves visualization and allows safer endoscopic resection | | **Transfusion avoidance** | Embolization decreases need for massive transfusion | | **Recurrence** | Proper embolization of all feeding vessels reduces recurrence risk | ### Preoperative Angiography & Embolization Protocol 1. **Selective angiography** of bilateral maxillary arteries and ascending pharyngeal artery to identify all feeding vessels 2. **Embolization** using particles (polyvinyl alcohol, gelatin sponge) or coils 24–48 hours before surgery 3. **Post-embolization imaging** to confirm vessel occlusion and assess residual blood supply 4. **Endoscopic resection** performed within 24–48 hours of embolization (before collateral circulation develops) ### Management Algorithm for NAF ```mermaid flowchart TD A[Suspected NAF on clinical + imaging grounds]:::outcome --> B[Confirm diagnosis with MRI/CT]:::action B --> C{Extent of disease?}:::decision C -->|Small, limited| D[Consider direct endoscopic resection]:::action C -->|Large, extensive, highly vascular| E[Preoperative angiography]:::action E --> F[Selective embolization of feeding vessels]:::action F --> G[Wait 24-48 hours for stabilization]:::action G --> H[Endoscopic resection under GA]:::action H --> I[Histopathology confirms benign angiofibroma]:::outcome I --> J{Residual disease on postop imaging?}:::decision J -->|No| K[Follow-up at 6-12 months]:::action J -->|Yes| L[Consider repeat embolization + resection]:::action ``` ### Why Other Options Are Incorrect **High-Yield:** **Never perform biopsy of a suspected NAF** — the risk of severe hemorrhage is unacceptable. Diagnosis is made on imaging (CT/MRI) and confirmed on histology after resection. **Clinical Pearl:** Immediate resection without embolization in a highly vascular NAF can result in intraoperative hemorrhage requiring emergency transfusion, airway compromise, or conversion to open approach. Embolization is the standard of care in most centers. ### Hormonal Therapy **Key Point:** Testosterone antagonists (e.g., flutamide, bicalutamide) have been studied as adjuvant therapy for recurrent or unresectable NAF, but they are **not primary treatment** and have variable efficacy. Surgery (with embolization) remains the definitive treatment. ### Outcomes & Follow-up - **Recurrence rate:** 10–30% after endoscopic resection (higher if incompletely resected) - **Imaging follow-up:** MRI at 6–12 months postoperatively - **Late recurrence:** Can occur years later; long-term surveillance recommended - **Malignant transformation:** Extremely rare; NAF remains benign even if recurrent 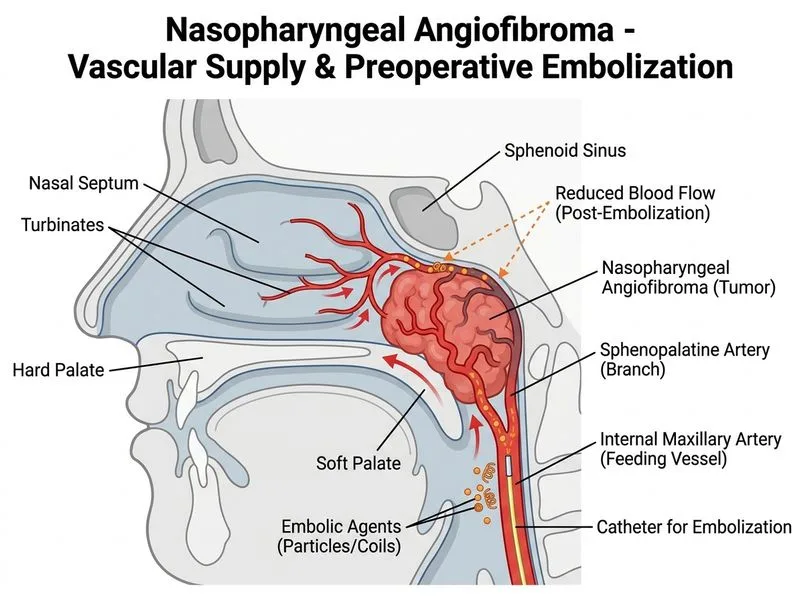
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.