## Management of Nasopharyngeal Angiofibroma: Preoperative Embolization ### Clinical Context **Key Point:** This patient has a Stage III nasopharyngeal angiofibroma (intracranial extension) with significant vascularity. The critical management principle is **preoperative embolization before any surgical intervention** to minimize life-threatening hemorrhage. ### Why Preoperative Embolization is Mandatory | Aspect | Rationale | |--------|----------| | **Vascularity** | NAF is supplied by maxillary artery branches; blood supply is rich and extensive | | **Hemorrhage risk** | Intraoperative bleeding can be catastrophic without embolization | | **Embolization timing** | Performed 24–48 hours before surgery to allow collateral circulation development | | **Embolization agent** | Polyvinyl alcohol (PVA), gelatin sponge, or coils | | **Blood loss reduction** | Decreases operative blood loss by 50–80% | | **Surgical approach** | Endoscopic resection for Stage I–II; open approach (e.g., Weber-Ferguson) for Stage III–IV | **High-Yield:** Preoperative embolization is the standard of care for all but the smallest NAF tumors. Attempting resection without embolization risks massive hemorrhage and mortality. ### Management Algorithm for NAF ```mermaid flowchart TD A[Diagnosed NAF]:::outcome --> B[Imaging: CT + MRI + Angiography]:::action B --> C{Staging & Vascularity Assessment}:::decision C -->|Stage I-II, moderate vascularity| D[Preoperative Embolization 24-48 hrs before surgery]:::action C -->|Stage III-IV, high vascularity| E[Preoperative Embolization 24-48 hrs before surgery]:::action D --> F{Surgical Approach}:::decision E --> F F -->|Stage I-II| G[Endoscopic resection]:::action F -->|Stage III-IV| H[Open approach ± endoscopic assistance]:::action G --> I[Postoperative surveillance]:::outcome H --> I ``` ### Preoperative Embolization: Technical Details **Clinical Pearl:** Embolization is performed via selective catheterization of the maxillary artery and its branches (sphenopalatine, greater palatine arteries). The goal is to reduce tumor blood flow without causing tissue necrosis or stroke. ### Surgical Approaches by Stage | Stage | Extent | Surgical Approach | |-------|--------|------------------| | **I** | Nasopharynx + nasal cavity | Endoscopic resection | | **II** | + Pterygopalatine fossa ± sinuses | Endoscopic resection (transnasal endoscopic) | | **III** | + Infratemporal fossa, orbit, skull base | Open approach (Weber-Ferguson, Le Fort I) ± endoscopic assistance | | **IV** | Intracranial extension | Multidisciplinary approach; may require neurosurgical involvement | **Key Point:** This patient (Stage III with intracranial extension) will likely require an open approach after embolization, possibly combined with endoscopic techniques. ### Why Each Alternative Is Incorrect **Immediate endoscopic resection without embolization:** - Risks catastrophic intraoperative hemorrhage - Standard of care mandates embolization first - Mortality and morbidity are significantly higher **Hormonal therapy (testosterone antagonists) alone:** - May slow growth but does NOT resolve the mass - Epistaxis and obstruction persist - Not definitive treatment; only adjunctive in select cases - Indicated post-puberty or for recurrent tumors **Radiotherapy as definitive treatment:** - NAF is radioresistant; external beam radiation is ineffective - Reserved for unresectable, recurrent, or palliative cases - Surgery is the gold standard for primary treatment ### Postoperative Surveillance **High-Yield:** Recurrence rate is 10–30% depending on completeness of resection and stage. Endoscopic surveillance every 3 months for the first year, then every 6 months for 2 years. [cite:Harrison 21e Ch 409; Robbins 10e Ch 16] 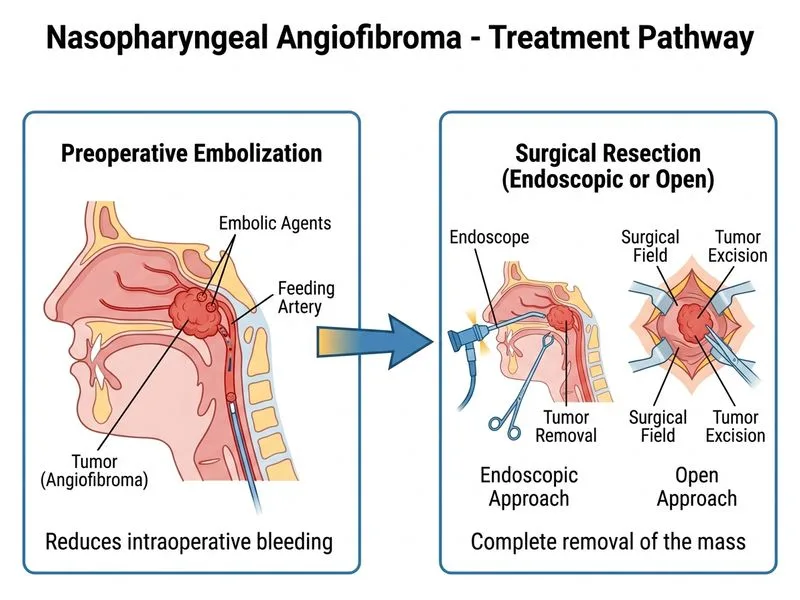
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.