## Management of Failed ORIF in Displaced Intracapsular Femoral Neck Fracture ### Clinical Scenario This patient has a **displaced Garden IV intracapsular fracture** with **poor bone quality** and **failed internal fixation attempt**. The surgeon has intraoperatively determined that cannulated screws cannot achieve stable fixation—a critical finding that mandates conversion to arthroplasty. ### Why Hemiarthroplasty? **Key Point:** When internal fixation is technically impossible (poor bone quality, unstable reduction, or failed fixation attempt), conversion to **hemiarthroplasty** is the standard of care. This eliminates the risk of AVN and non-union and allows immediate weight-bearing. **High-Yield:** Hemiarthroplasty is indicated in: - Displaced intracapsular fractures in patients >65–70 years with poor bone quality - Failed ORIF attempts (as in this case) - Fractures with significant comminution - Patients with dementia or poor compliance (early mobilization is critical) **Clinical Pearl:** Cemented hemiarthroplasty is preferred over uncemented in elderly osteoporotic patients because cement provides immediate stability and reduces the risk of early loosening and subsidence. ### Why Other Options Are Incorrect | Option | Why Inappropriate | |---|---| | **DHS + side plate** | DHS is for **extracapsular** (intertrochanteric/subtrochanteric) fractures, not intracapsular. It does not address the failed fixation or poor bone quality. | | **Skeletal traction** | After a failed ORIF attempt, traction is futile. It delays definitive treatment, increases infection risk, and leads to poor outcomes (non-union, AVN, prolonged immobility). | | **Conservative management** | A displaced intracapsular fracture cannot be managed non-operatively. This leads to malunion, non-union, and severe functional disability. | **Mnemonic: FAILED ORIF + POOR BONE = HEMIARTHROPLASTY** — Do not persist with fixation; convert to arthroplasty. ### Decision Tree for Intracapsular Femoral Neck Fracture ```mermaid flowchart TD A[Displaced Intracapsular NOF Fracture]:::outcome --> B{Patient age & bone quality?}:::decision B -->|Young/good bone| C[Attempt ORIF with cannulated screws]:::action B -->|Elderly/poor bone| D[Consider hemiarthroplasty]:::action C --> E{Fixation stable?}:::decision E -->|Yes| F[Proceed with ORIF]:::action E -->|No| G[Convert to hemiarthroplasty]:::action D --> H[Proceed with hemiarthroplasty]:::action G --> I[Cemented prosthesis]:::action H --> I I --> J[Early weight-bearing & mobilization]:::action J --> K[Good functional outcome]:::outcome ``` ### Hemiarthroplasty vs. Total Hip Arthroplasty | Feature | Hemiarthroplasty | Total Hip Arthroplasty | |---|---|---| | **Indication** | Displaced intracapsular NOF (most common) | Preexisting osteoarthritis of hip | | **Operative time** | Shorter | Longer | | **Blood loss** | Less | More | | **Dislocation rate** | ~10% | ~2–5% | | **Acetabular wear** | Yes (long-term issue) | No | | **Preferred in NOF** | Yes, standard | Only if OA present | [cite:Campbell's Operative Orthopaedics 13e Ch 56; Rockwood & Green's Fractures in Adults Ch 53] 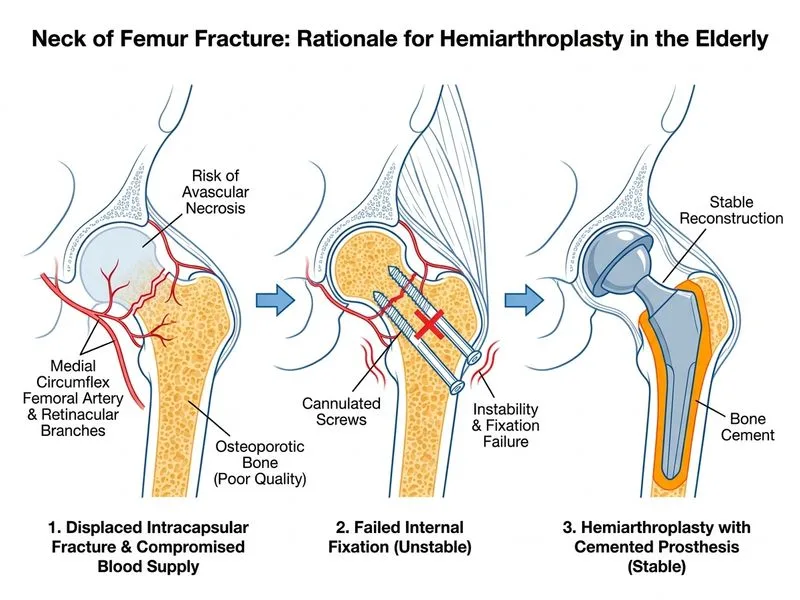
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.