## Clinical Diagnosis: ABO Incompatibility ### Key Distinguishing Features **Key Point:** ABO incompatibility is the most common hemolytic disease of the newborn (HDN) in developed countries, yet often presents mildly despite a positive DCT. | Feature | ABO Incompatibility | Rh Incompatibility | |---------|-------------------|-------------------| | **Maternal blood group** | O (has anti-A, anti-B IgG naturally) | Rh-negative (sensitized) | | **Antenatal ICT** | Often negative (natural antibodies) | Positive (from prior sensitization) | | **First affected infant** | Can be affected | Rarely affected (first pregnancy) | | **Severity** | Usually mild-moderate | Often severe | | **Peripheral smear** | Spherocytes common | Nucleated RBCs, polychromasia | | **Hydrops** | Rare | Common in severe cases | ### Why This Case Is ABO Incompatibility 1. **O-positive mother with B-positive baby** — classic ABO incompatibility scenario. O mothers naturally produce IgG anti-A and anti-B antibodies (from exposure to A and B antigens in environment/food). 2. **Negative antenatal ICT** — maternal natural antibodies are often not detected on routine ICT; they only become apparent when baby's RBCs are tested (positive DCT). 3. **Positive DCT on baby** — confirms IgG-mediated hemolysis (maternal antibodies coating fetal RBCs). 4. **Spherocytes on smear** — pathognomonic for ABO HDN; spherocytes result from partial destruction of RBC membrane by antibody-complement lysis. 5. **Mild-moderate hyperbilirubinemia at day 3** — typical presentation; rarely as severe as Rh disease. ### Pathophysiology ```mermaid flowchart TD A[O-positive mother]:::outcome --> B[Natural anti-A/anti-B IgG]:::outcome B --> C[Crosses placenta]:::outcome C --> D[Binds to B antigen on fetal RBCs]:::outcome D --> E[Complement activation + phagocytosis]:::action E --> F[Spherocyte formation + hemolysis]:::outcome F --> G[Unconjugated hyperbilirubinemia]:::outcome G --> H[Jaundice by day 2-3]:::outcome ``` ### Clinical Pearl **Clinical Pearl:** ABO incompatibility typically presents earlier (day 2–3) and more acutely than Rh disease (day 5–7), but is usually milder. The positive DCT with spherocytes is the diagnostic hallmark. ### High-Yield Facts **High-Yield:** - ABO incompatibility occurs in ~1 in 150 births but causes HDN in only ~1 in 3000 (most are asymptomatic). - Rh incompatibility is now rare in countries with RhIG prophylaxis but remains severe when it occurs. - Negative antenatal ICT does NOT rule out ABO incompatibility — always check baby's DCT. [cite:Nelson Textbook of Pediatrics 21e Ch 101] 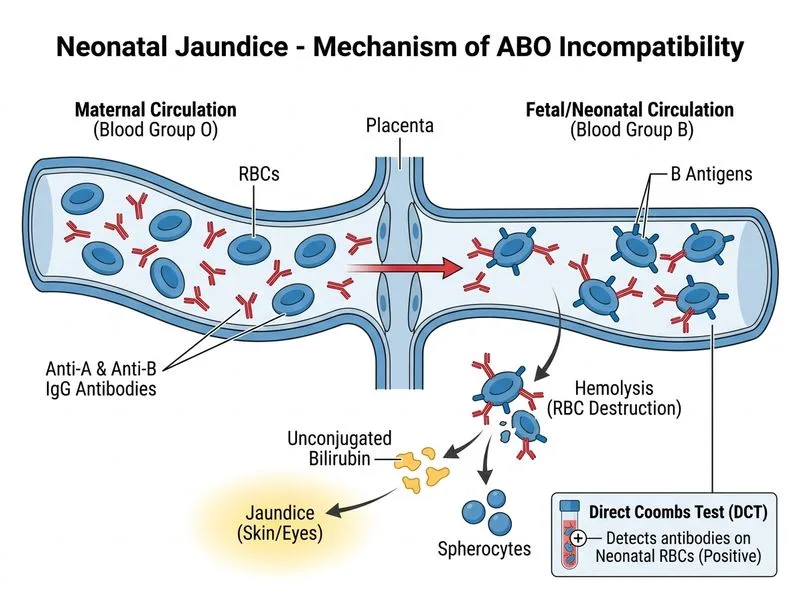
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.