## Distinguishing ABO from Rh Hemolytic Disease ### Key Immunological Difference **Key Point:** The nature of maternal antibodies is the fundamental discriminator between ABO and Rh incompatibility. | Feature | ABO Incompatibility | Rh Incompatibility | | --- | --- | --- | | **Maternal antibodies** | Naturally occurring IgM (non-immune) | Immune IgG (sensitization required) | | **Placental transfer** | Minimal (IgM too large) | Efficient (IgG crosses placenta) | | **First pregnancy affected?** | Yes (natural IgM present) | No (needs prior sensitization) | | **Severity in 1st pregnancy** | Usually mild | Usually absent | | **Severity in subsequent pregnancies** | Similar mild course | Progressively severe | | **DAT result** | Often weakly positive or negative | Usually strongly positive | | **Hydrops fetalis** | Rare | Common (if untreated) | ### Clinical Pearl **Clinical Pearl:** ABO incompatibility can affect the first-born because mothers naturally have IgM anti-A or anti-B antibodies from environmental exposure (cross-reactivity with bacteria). These IgM molecules are too large to cross the placenta efficiently, resulting in mild hemolysis. Rh incompatibility requires prior sensitization (usually during delivery of an Rh-positive baby), so it spares the first-born but becomes progressively severe in subsequent pregnancies as maternal IgG titers rise. ### Why This Matters **High-Yield:** This immunological distinction explains why: - ABO jaundice is typically mild and self-limited - Rh disease worsens with parity (unless mother is given anti-D prophylaxis) - Rh disease can present as severe hemolytic anemia or hydrops in utero [cite:Park 26e Ch 11] 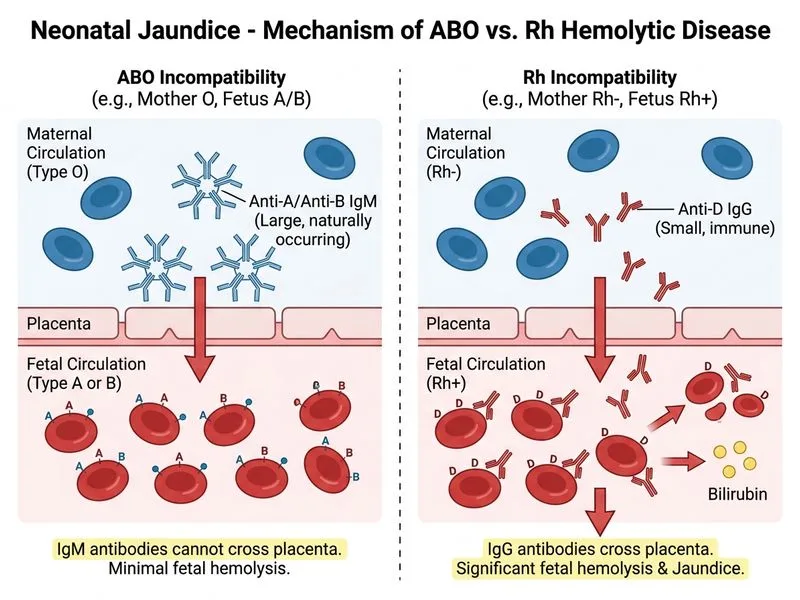
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.