## Breastfeeding Jaundice vs Breast Milk Jaundice ### Pathophysiological Distinction **Key Point:** The discriminating feature is the presence or absence of inadequate milk transfer and poor weight gain. | Feature | Breastfeeding Jaundice | Breast Milk Jaundice | | --- | --- | --- | | **Timing of onset** | Days 2–5 (early) | Days 5–14 (late) | | **Cause** | Inadequate milk intake due to poor latch, infrequent feeding, or maternal factors | Reduced intestinal reabsorption of bilirubin (β-glucuronidase in milk, reduced enterohepatic circulation) | | **Weight loss** | Excessive (>10% by day 3–5) | Mild to moderate | | **Feeding assessment** | Poor latch, inadequate transfer, few wet diapers | Good latch, adequate transfer, adequate output | | **Milk production** | May be delayed or insufficient | Adequate or abundant | | **Management** | Improve breastfeeding technique, increase frequency, consider supplementation | Continue breastfeeding (safe), monitor bilirubin, phototherapy if indicated | | **Prognosis** | Resolves with improved feeding | Self-limited, resolves by 3–4 weeks | ### Clinical Pearl **Clinical Pearl:** Breastfeeding jaundice is a **preventable** problem caused by inadequate milk transfer — it reflects a failure of the breastfeeding process itself. Breast milk jaundice is a **physiological** phenomenon caused by substances in human milk that increase bilirubin reabsorption — it occurs despite adequate feeding and is not a failure of breastfeeding. ### High-Yield Mnemonic **Mnemonic:** **BFJ vs BMJ** — - **BFJ** = **B**ad **F**eeding (poor latch, inadequate transfer, weight loss >10%) - **BMJ** = **B**reast **M**ilk (good feeding, mild weight loss, late onset) ### Management Implications **High-Yield:** - Breastfeeding jaundice requires **intervention on feeding** (lactation support, increased frequency, possible supplementation) - Breast milk jaundice can be managed with **continued breastfeeding** alone (phototherapy if bilirubin exceeds threshold) [cite:Park 26e Ch 11] 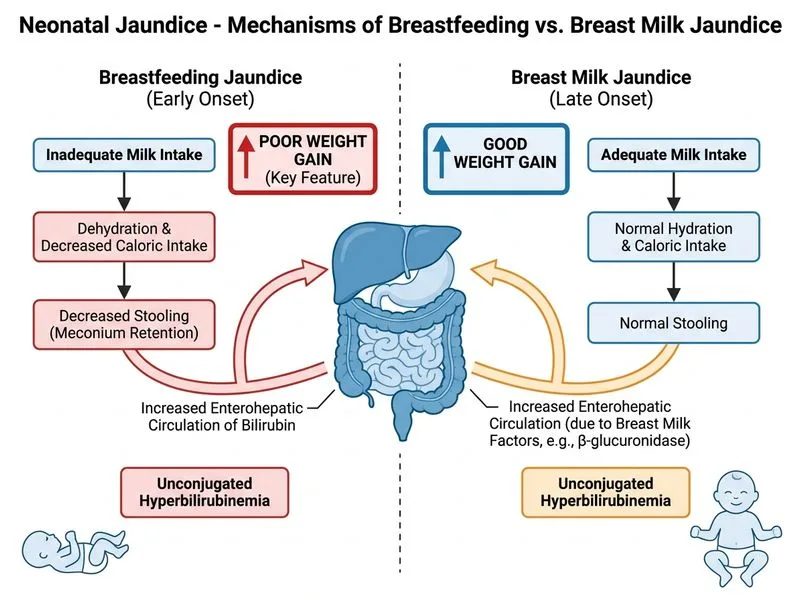
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.