## Diagnosis: Hemolytic Disease of Newborn (HDN) Due to Rh Incompatibility ### Clinical Reasoning **Key Point:** The combination of **Rh-negative mother with Rh-positive infant**, **positive family history** (first child had jaundice), **elevated reticulocyte count (4.2%)**, **microspherocytes on smear**, and **strongly positive DAT (3+)** is pathognomonic for **Rh incompatibility**. ### Pathophysiology of Rh Incompatibility 1. **Sensitization:** First pregnancy (Rh-negative mother, Rh-positive fetus) → fetomaternal hemorrhage at delivery → maternal IgG anti-D antibodies develop (usually no hemolysis in first child). 2. **Second pregnancy:** IgG anti-D crosses placenta → binds to fetal RBCs → hemolysis → jaundice, anemia, hydrops (if severe). 3. **Mechanism:** IgG antibodies (unlike ABO IgM) cross the placenta and cause **extravascular hemolysis** in the fetal spleen. ### Diagnostic Criteria for Rh Incompatibility | Feature | Finding | Significance | |---------|---------|---------------| | **Maternal blood group** | A Rh-negative | Sensitized in first pregnancy | | **Infant blood group** | A Rh-positive | Antigen target for maternal antibodies | | **Birth history** | First child had jaundice | Classic pattern: mild in first, severe in second | | **DAT (Coombs)** | 3+ (strongly positive) | IgG-coated RBCs; confirms immune hemolysis | | **Hemoglobin** | 13.8 g/dL (low-normal) | Mild anemia from hemolysis | | **Reticulocyte count** | 4.2% (elevated) | Compensatory RBC production | | **Blood smear** | Microspherocytes | Characteristic of immune hemolysis | | **Bilirubin** | 16 mg/dL at day 5 | Exceeds phototherapy threshold | ### Why IVIG + Phototherapy? **High-Yield:** IVIG (intravenous immunoglobulin) is the **first-line medical intervention** for HDN due to Rh incompatibility because: 1. **Mechanism:** IVIG blocks Fc receptors on macrophages in the spleen → reduces RBC destruction → slows bilirubin rise. 2. **Efficacy:** Reduces need for exchange transfusion by ~50%. 3. **Dose:** 0.5–1 g/kg IV over 2–4 hours; can repeat if bilirubin continues to rise. 4. **Timing:** Most effective if given within first 48 hours of life. **Phototherapy** is concurrent management: - Converts unconjugated bilirubin to water-soluble **photoisomers** → urinary excretion. - At day 5, bilirubin of 16 mg/dL is **above phototherapy threshold** (typically 14–15 mg/dL for a term infant at day 5). ### Exchange Transfusion Indications **Warning:** Exchange transfusion is reserved for: - Bilirubin rising despite IVIG + phototherapy. - Signs of **acute bilirubin encephalopathy** (lethargy, hypotonia, high-pitched cry, seizures). - **Severe anemia** (Hb <7 g/dL) with hydrops. This infant does not yet meet criteria for exchange transfusion, but IVIG + phototherapy are indicated **now** to prevent further hemolysis and bilirubin rise. ### Prevention in Future Pregnancies **Clinical Pearl:** Rh-negative mothers should receive **anti-D immunoglobulin (RhoGAM)**: - **Antenatally:** 500 IU (100 μg) at 28 weeks (or 1500 IU at 34 weeks in some protocols). - **Postnatally:** Within 72 hours of delivery of an Rh-positive infant; dose adjusted for fetomaternal hemorrhage volume. This prevents sensitization in future pregnancies. 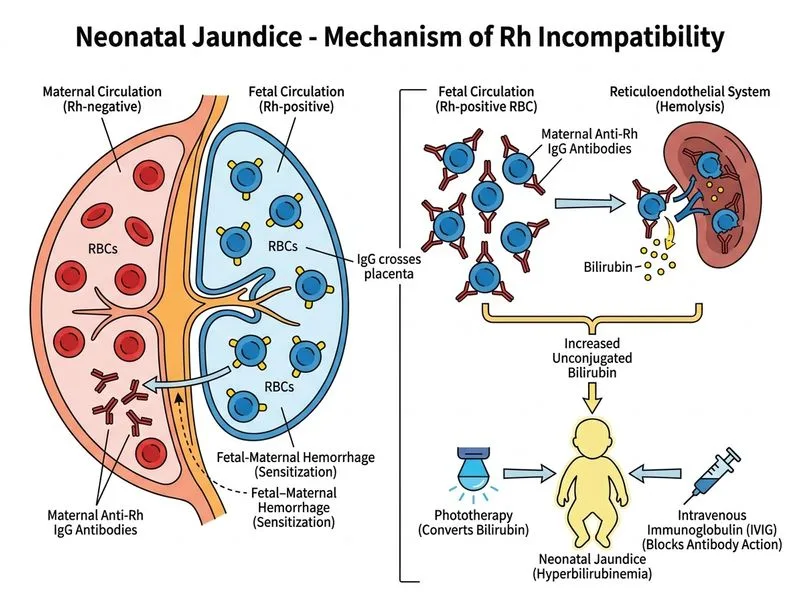
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.