## Clinical Diagnosis and Management: Rh Incompatibility with Hydrops Fetalis ### Clinical Presentation Analysis **Key Point:** This case represents severe Rh incompatibility (erythroblastosis fetalis) with hydrops fetalis—a medical emergency requiring immediate exchange transfusion. ### Diagnostic Features | Feature | Finding | Significance | |---------|---------|-------------| | **Maternal Blood Group** | O negative | Rh-negative mother (sensitized) | | **Infant Blood Group** | B positive | Rh-positive antigen on RBCs | | **Coombs Test** | Strongly positive | Heavy IgG coating of RBCs | | **Antenatal History** | Polyhydramnios at 28 weeks | Marker of fetal compromise | | **Clinical Signs** | Hydrops (edema, ascites, hepatosplenomegaly) | Severe hemolysis with cardiac failure | | **Hemoglobin** | 9.2 g/dL (low) | Significant anemia from hemolysis | | **Reticulocyte Count** | 12% (elevated) | Compensatory erythropoiesis | | **Bilirubin Level** | 22 mg/dL at day 5 | Exceeds exchange threshold | | **Direct Bilirubin** | 0.8 mg/dL (low) | Unconjugated hyperbilirubinemia | ### Pathophysiology of Rh Disease **High-Yield:** Rh incompatibility develops when: 1. Rh-negative mother becomes sensitized (usually during first pregnancy or delivery) 2. Maternal IgG anti-D antibodies develop and cross placenta in subsequent pregnancies 3. Antibodies bind to fetal D antigen on RBCs 4. Hemolysis occurs in fetal circulation → anemia, hyperbilirubinemia, hydrops 5. Severe cases cause fetal/neonatal death without intervention **Mnemonic: HYDROPS** — **H**emolysis, **Y**ellowness (jaundice), **D**istress (respiratory), **R**eticulocytosis, **O**edema, **P**leural effusion, **S**plenomegaly ### Why Exchange Transfusion Is Indicated **Clinical Pearl:** Exchange transfusion is the definitive treatment for severe neonatal jaundice with hemolysis because it: 1. **Removes bilirubin** — exchanges 80–90% of circulating bilirubin 2. **Removes sensitized RBCs** — eliminates RBCs coated with maternal antibodies 3. **Corrects anemia** — replaces destroyed RBCs with healthy donor RBCs 4. **Prevents kernicterus** — rapidly lowers unconjugated bilirubin before it crosses blood-brain barrier 5. **Treats hydrops** — improves cardiac output and tissue perfusion ### Blood Selection for Exchange Transfusion in Rh Disease **Key Point:** In Rh incompatibility, use **Rh-negative, type O blood** because: - **Rh-negative:** Lacks D antigen, so maternal anti-D antibodies cannot bind and cause further hemolysis - **Type O:** Universal donor RBCs; lacks A and B antigens, avoiding transfusion reactions - **Crossmatched:** Blood is crossmatched against both maternal and infant serum - **Fresh:** Preferably less than 5 days old to ensure optimal RBC survival and function ### Exchange Transfusion Procedure ```mermaid flowchart TD A[Severe Jaundice + Hemolysis]:::outcome --> B{Bilirubin exceeds exchange threshold?}:::decision B -->|Yes| C[Prepare for exchange transfusion]:::action C --> D[Obtain Rh-negative, type O blood]:::action D --> E[Establish umbilical venous catheter]:::action E --> F[Withdraw 5-10 mL blood aliquots]:::action F --> G[Infuse donor blood aliquots]:::action G --> H[Repeat until 2 blood volumes exchanged]:::action H --> I[Post-exchange monitoring]:::action I --> J[Check bilirubin at 4-6 hours]:::action J --> K{Bilirubin rebounding?}:::decision K -->|Yes| L[Repeat exchange if needed]:::action K -->|No| M[Continue phototherapy]:::action M --> N[Discharge when safe]:::outcome ``` ### Why Other Options Are Inadequate **Phototherapy alone (Option A):** - Insufficient for bilirubin level of 22 mg/dL at day 5 - Cannot remove sensitized RBCs or correct anemia - Risk of kernicterus in severely hemolyzed infants - Hydrops fetalis requires urgent intervention beyond phototherapy **IVIG followed by phototherapy (Option C):** - IVIG is adjunctive therapy, not primary treatment for severe Rh disease - May be used to reduce hemolysis rate, but does not replace exchange transfusion - Indicated when phototherapy alone is insufficient but not as first-line in hydrops - Slower onset of action than exchange transfusion **Packed RBC transfusion (Option D):** - Does not remove bilirubin or sensitized RBCs - Increases viscosity and worsens cardiac strain in hydrops - May precipitate hyperkalemia and cardiac arrhythmias - Not appropriate for unconjugated hyperbilirubinemia ### High-Yield Clinical Pearls **High-Yield:** - **Rh disease is preventable:** Antenatal RhIG (500 IU/kg at 28 weeks) reduces sensitization risk - **Postnatal RhIG:** Given to unsensitized Rh-negative mothers within 72 hours of delivery - **Hydrops fetalis:** Indicates severe fetal compromise; intrauterine transfusion may be needed prenatally - **Exchange transfusion threshold:** Varies by postnatal age and risk factors; use nomogram - **Kernicterus risk:** Highest in hemolytic disease due to rapid bilirubin rise and RBC destruction ### Prognosis and Follow-up **Clinical Pearl:** With appropriate exchange transfusion: - Bilirubin levels drop rapidly (by 50% or more) - Anemia improves as donor RBCs circulate - Hydrops may resolve over hours to days - Long-term prognosis is excellent if kernicterus is prevented - Subsequent pregnancies require antenatal monitoring and possible intrauterine transfusion [cite:Nelson Textbook of Pediatrics 21e Ch 101] 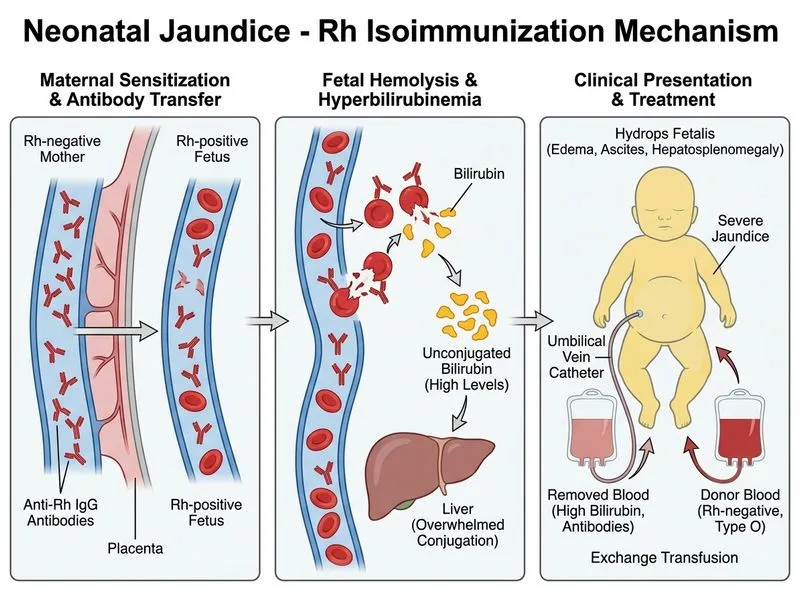
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.