## Mechanism of Physiological Jaundice **Key Point:** Physiological jaundice results from a combination of immature hepatic conjugation capacity and increased enterohepatic circulation of bilirubin in the newborn. ### Pathophysiology 1. **Immature UDP-glucuronosyltransferase (UGT1A1)** — The neonatal liver has only 1% of adult enzyme activity at birth, reaching adult levels by 2–4 weeks of age. 2. **Increased enterohepatic circulation** — Neonates have: - High intestinal β-glucuronidase activity - Sterile gut (lack of bacteria to convert bilirubin to urobilinogen) - Increased reabsorption of unconjugated bilirubin from the intestine ### Timeline & Clinical Features - Appears after 24 hours of life (rarely in first 24 hours) - Peaks at 3–5 days of life - Resolves by 1–2 weeks in term infants - Does NOT cause kernicterus if managed appropriately **High-Yield:** Physiological jaundice is **unconjugated** hyperbilirubinemia; conjugated bilirubin remains normal. ### Why Other Options Are Wrong | Mechanism | Why Not Physiological Jaundice | |-----------|--------------------------------| | Hemolysis | Occurs in pathological jaundice (ABO/Rh incompatibility, G6PD deficiency); RBC lifespan is normal in physiological jaundice | | Biliary atresia | Causes **conjugated** (direct) hyperbilirubinemia, not unconjugated; presents later with acholic stools | | Hepatocellular injury | Seen in TORCH infections, syphilis; causes mixed hyperbilirubinemia with elevated transaminases | **Clinical Pearl:** Early feeding (within 2 hours of birth) and adequate breastfeeding reduce enterohepatic circulation and lower peak bilirubin levels by 10–15%. 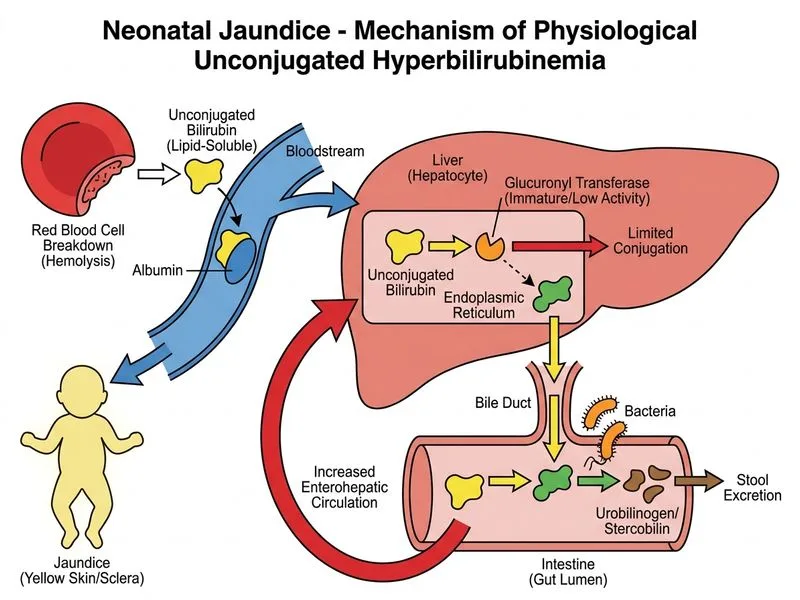
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.