## Distinguishing Features of Rh vs ABO Incompatibility ### Key Pathophysiology **Key Point:** Rh incompatibility requires prior sensitization (usually during previous pregnancy), whereas ABO incompatibility can occur in first-born infants because maternal IgG anti-A and anti-B antibodies are naturally present. ### Comparative Table | Feature | Rh Incompatibility | ABO Incompatibility | |---------|-------------------|--------------------| | **First-born involvement** | Rarely affected (needs prior sensitization) | Often affects first-born | | **Severity in first pregnancy** | Mild to moderate | Mild (usually self-limited) | | **Severity in subsequent pregnancies** | Progressively severe (hemolytic disease of fetus and newborn) | Remains mild | | **DAT result** | Strongly positive (IgG) | Weakly positive or negative (IgM does not cross placenta) | | **Jaundice onset** | Within first 24 hours (severe cases) | Usually after 24 hours | | **Kernicterus risk** | High if untreated | Low (milder disease) | ### Clinical Pearl **Clinical Pearl:** Rh incompatibility causes **severe hemolysis in subsequent pregnancies** because maternal IgG antibodies (from prior sensitization) cross the placenta and attack fetal RBCs. The **first-born is typically spared** unless the mother was previously sensitized (e.g., by transfusion or abortion). ### High-Yield Distinction **High-Yield:** The hallmark of Rh disease is **progressive severity with each pregnancy**, whereas ABO disease remains mild and self-limited. This is why severe HDN in the first-born strongly suggests ABO incompatibility, and severe disease in the second or third child suggests Rh incompatibility. **Key Point:** In ABO incompatibility, the first-born can be severely affected because natural IgG anti-A/anti-B exist from birth. In Rh incompatibility, the first-born is typically unaffected because sensitization has not yet occurred. 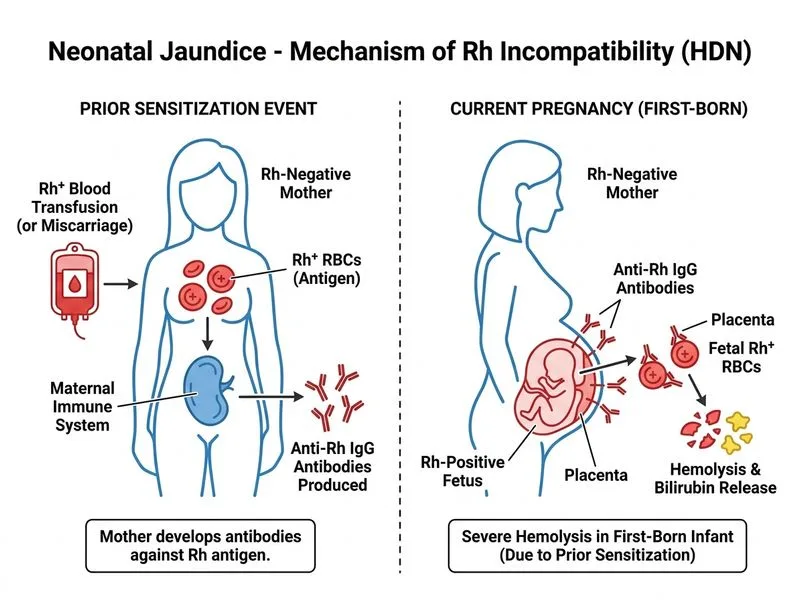
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.