## Clinical Diagnosis **Key Point:** This is acute post-streptococcal glomerulonephritis (APSGN) — the classic tetrad of gross haematuria, hypertension, oedema, and reduced renal function following pharyngitis, with low C3 complement and RBC casts on urinalysis. ## Management Strategy for Acute Nephritic Syndrome ### Immediate Priorities **High-Yield:** The cornerstone of APSGN management is **supportive care** in the acute phase, NOT immunosuppression. Most cases (>95%) resolve spontaneously within 2–4 weeks with conservative management. 1. **Fluid and electrolyte management** - Fluid restriction (typically 800–1000 mL/day) to manage oedema and hypertension - Monitor daily weight and urine output - Avoid hyperkalemia (restrict K^+^ intake if needed) 2. **Antihypertensive therapy** - Target BP control to reduce proteinuria and prevent hypertensive complications - First-line: ACE inhibitor or ARB (e.g., enalapril, losartan) - Add diuretics (furosemide) if oedema or fluid overload present 3. **Diuretics** - Indicated here: patient has periorbital oedema and mild ascites - Furosemide 40–80 mg daily, titrate based on response 4. **Monitoring** - Serial serum creatinine, electrolytes, and complement levels - Repeat urinalysis to track haematuria and proteinuria ### Role of Corticosteroids **Clinical Pearl:** Corticosteroids are **NOT indicated** in uncomplicated APSGN because the disease is self-limited and immune-mediated resolution occurs naturally. Steroids are reserved for: - Rapidly progressive glomerulonephritis (RPGN) with crescents - Severe renal impairment (Cr >3 mg/dL) or oliguria - Pulmonary haemorrhage or vasculitis This patient, while having elevated creatinine, does not meet criteria for aggressive immunosuppression at presentation. ### Role of Renal Biopsy **High-Yield:** Renal biopsy is **NOT routine** in APSGN. It is indicated only if: - No improvement in renal function after 2–3 weeks of conservative management - Persistent proteinuria or haematuria beyond 6 months - Atypical clinical features or diagnostic uncertainty This patient should be observed first; biopsy is deferred unless clinical course deteriorates. ### Why NOT Plasma Exchange or Cyclophosphamide? **Warning:** These aggressive therapies are reserved for RPGN with anti-GBM disease or ANCA-associated vasculitis, not APSGN. No clinical or serological evidence of systemic vasculitis is present. ## Management Algorithm ```mermaid flowchart TD A[Acute Nephritic Syndrome + APSGN features]:::outcome --> B[Admit for monitoring]:::action B --> C[Fluid restriction + Diuretics]:::action B --> D[Antihypertensives]:::action B --> E[Monitor Cr, K+, C3, UA]:::action F{Improvement in 2-3 weeks?}:::decision C --> F D --> F E --> F F -->|Yes| G[Continue conservative care, outpatient follow-up]:::outcome F -->|No| H[Consider renal biopsy]:::action H --> I{RPGN/Crescents?}:::decision I -->|Yes| J[Pulse methylprednisolone + Cyclophosphamide]:::action I -->|No| K[Continue supportive care]:::action ``` **Key Point:** Admission is appropriate because the patient has: - Significant hypertension (156/98) requiring close monitoring - Elevated creatinine (1.8) indicating acute kidney injury - Oedema and ascites requiring diuretic management - Risk of hypertensive encephalopathy or pulmonary oedema ## Summary Table: APSGN vs. RPGN Management | Feature | APSGN | RPGN | | --- | --- | --- | | **Corticosteroids** | Not routine; avoid unless severe | Pulse methylprednisolone + oral steroids | | **Immunosuppression** | None | Cyclophosphamide or rituximab | | **Plasma exchange** | Not indicated | Indicated if anti-GBM or ANCA | | **Diuretics/Antihypertensives** | Yes, mainstay | Yes, adjunctive | | **Renal biopsy** | Only if no improvement >2 wks | Early, to guide therapy | | **Expected outcome** | >95% recover completely | Depends on ANCA/anti-GBM status | [cite:Harrison 21e Ch 279] 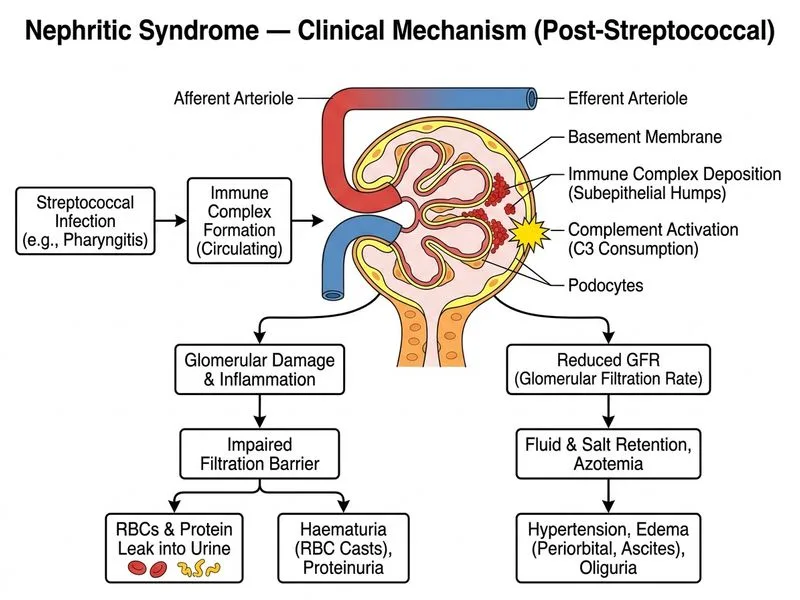
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.