## Clinical Diagnosis **Key Point:** This is lupus nephritis (LN) presenting as acute nephritic syndrome with rapid loss of renal function. The combination of SLE history, low complement, elevated anti-dsDNA, RBC and WBC casts, and acute AKI mandates urgent immunosuppressive therapy. ## Pathophysiology of Lupus Nephritis **High-Yield:** Lupus nephritis is immune complex-mediated glomerulonephritis. The presence of: - Low C3/C4 (complement consumption) - Elevated anti-dsDNA (active SLE) - RBC casts (glomerular bleeding) - WBC casts (glomerular inflammation) ...indicates **active proliferative lupus nephritis** (likely Class III or IV), which requires immediate immunosuppression to prevent irreversible renal damage. ## Management of Acute Lupus Nephritis ### Immediate Actions (Within Hours) 1. **Pulse methylprednisolone (IV)** - **Dose:** 500 mg IV daily for 3 consecutive days - **Rationale:** Rapid anti-inflammatory effect to reduce glomerular inflammation and halt complement-mediated injury - **Timing:** Do NOT delay for biopsy results; start immediately upon clinical diagnosis 2. **Oral prednisolone** - **Dose:** 1 mg/kg/day (typically 50–60 mg/day) after pulse therapy - **Taper:** Gradually reduce over weeks to months based on clinical response 3. **Renal biopsy** - **Timing:** Arrange within 1 week (not before starting therapy) - **Purpose:** Determine lupus nephritis class (I–VI) to guide long-term immunosuppressive choice - **Key Point:** Do NOT delay immunosuppression waiting for biopsy; clinical and serological evidence is sufficient to start therapy ### Concurrent Supportive Measures - **ACE inhibitor/ARB:** Continue or optimize dose for proteinuria reduction and renal protection - **Antihypertensives:** Target BP <130/80 mmHg - **Diuretics:** If oedema or fluid overload present ### Long-Term Immunosuppression (After Pulse Therapy) **High-Yield:** Biopsy class determines choice: | LN Class | Features | First-Line Immunosuppression | | --- | --- | --- | | **I–II** (Minimal/Mesangial) | Mild, often asymptomatic | Observation or low-dose prednisolone | | **III (Focal Proliferative)** | <50% glomeruli involved | IV methylprednisolone + Cyclophosphamide or MMF | | **IV (Diffuse Proliferative)** | >50% glomeruli involved; worst prognosis | IV methylprednisolone + Cyclophosphamide (preferred) or MMF | | **V (Membranous)** | Pure or mixed with proliferative | Prednisolone + Cyclophosphamide or MMF | | **VI (Advanced Sclerotic)** | Irreversible; >90% sclerosis | Supportive care; immunosuppression unlikely to help | **Clinical Pearl:** For Class IV (diffuse proliferative) LN, **IV cyclophosphamide** is the gold standard induction therapy: - **Regimen:** 500–1000 mg/m² IV monthly for 6 months (NIH protocol) - **Alternative:** Mycophenolate mofetil (MMF) 2–3 g/day if cyclophosphamide contraindicated (e.g., fertility concerns, severe infection risk) ## Why Immediate Immunosuppression? **Warning:** Delaying immunosuppression in Class III/IV LN risks: - Rapid progression to ESRD - Irreversible glomerular scarring - Loss of renal function within weeks This patient's 1-week rise in creatinine from 0.9 to 2.1 mg/dL signals aggressive disease requiring urgent intervention. ## Management Algorithm ```mermaid flowchart TD A[SLE + Acute Nephritic Syndrome]:::outcome --> B{Clinical + Serological evidence of LN?}:::decision B -->|Yes: Low C3/C4, high anti-dsDNA, RBC/WBC casts| C[Start IV Methylprednisolone 500 mg daily x 3 days]:::action B -->|No: Atypical presentation| D[Arrange urgent renal biopsy first]:::action C --> E[Start Oral Prednisolone 1 mg/kg/day]:::action E --> F[Arrange renal biopsy within 1 week]:::action F --> G{Biopsy Class?}:::decision G -->|Class I-II| H[Continue prednisolone, taper slowly]:::action G -->|Class III-IV| I[Add IV Cyclophosphamide or MMF]:::action G -->|Class V| J[Prednisolone + Cyclophosphamide/MMF]:::action G -->|Class VI| K[Supportive care, consider dialysis]:::action I --> L[Monitor renal function, proteinuria, complement]:::action J --> L H --> L ``` ## Why NOT Delayed Biopsy? **Clinical Pearl:** In suspected Class III/IV LN with rapid renal deterioration, **do NOT wait for biopsy before starting immunosuppression**. The clinical and serological picture (low complement, high anti-dsDNA, RBC casts, acute AKI) is diagnostic enough. Biopsy is performed after therapy initiation to confirm class and guide long-term management. ## Summary: APSGN vs. Lupus Nephritis Management | Feature | APSGN | Lupus Nephritis | | --- | --- | --- | | **Immediate corticosteroids** | Not routine | Yes, IV pulse + oral | | **Immunosuppression** | None | Cyclophosphamide or MMF | | **Renal biopsy timing** | Deferred unless no improvement | Early (within 1 week), after starting therapy | | **Expected outcome** | >95% recovery | Depends on class; Class IV has worst prognosis | | **Complement levels** | Low C3 (recovers) | Persistently low C3/C4 (active disease marker) | [cite:Harrison 21e Ch 279; Robbins 10e Ch 20] 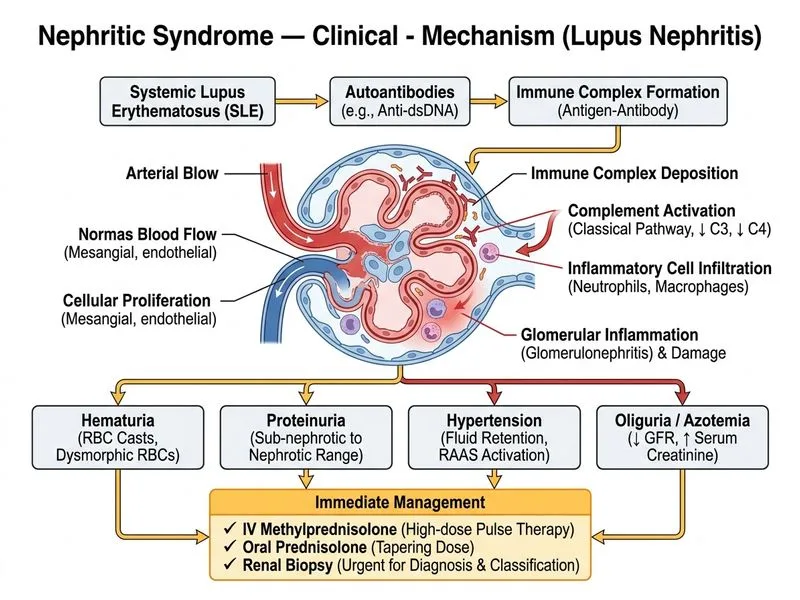
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.