## Hypercoagulability in Nephrotic Syndrome **Key Point:** Nephrotic syndrome is a hypercoagulable state due to selective urinary loss of anticoagulant proteins (antithrombin III, protein C, protein S) combined with increased hepatic synthesis of procoagulant factors. ### Pathophysiology of Thrombosis in Nephrotic Syndrome ```mermaid flowchart TD A[Nephrotic Syndrome<br/>Proteinuria >3.5 g/day]:::outcome --> B[Selective Loss of<br/>Small Plasma Proteins]:::action B --> C[Loss of Anticoagulants:<br/>Antithrombin III<br/>Protein C & S<br/>Plasminogen]:::urgent A --> D[Liver Responds to<br/>Hypoalbuminemia]:::action D --> E[Increased Synthesis of<br/>Procoagulants:<br/>Fibrinogen<br/>Prothrombin<br/>Factor V & VIII]:::action C --> F[Imbalance: ↓ Anticoagulation<br/>+ ↑ Coagulation]:::urgent E --> F F --> G[Hypercoagulable State]:::outcome G --> H[Thrombotic Complications:<br/>DVT, PE, RVT]:::urgent ``` ### Selective Urinary Loss of Anticoagulant Proteins | Protein | Molecular Weight | Normal Plasma Level | Urinary Loss in NS | Clinical Consequence | |---------|------------------|-------------------|-------------------|----------------------| | Antithrombin III | 58 kDa | 20–30 mg/dL | Marked loss | ↓ Factor IIa, IXa, Xa inhibition | | Protein C | 62 kDa | 4 mg/dL | Marked loss | ↓ Inactivation of Va, VIIIa | | Protein S | 69 kDa | 25 mg/dL | Marked loss | ↓ Cofactor for protein C | | Plasminogen | 92 kDa | 10–20 mg/dL | Moderate loss | ↓ Fibrinolysis | **High-Yield:** The loss of anticoagulant proteins (molecular weight 58–92 kDa) is **selective** — these are preferentially filtered in nephrotic proteinuria, whereas larger procoagulants (fibrinogen, prothrombin) are retained and actually synthesized in excess by the liver. ### Hepatic Compensation and Procoagulant Synthesis - **Trigger:** Hypoalbuminemia and oncotic pressure changes trigger hepatic synthesis of acute-phase reactants. - **Result:** Increased production of fibrinogen, prothrombin (Factor II), Factor V, Factor VIII, and von Willebrand factor. - **Net effect:** Unopposed procoagulant activity due to loss of natural anticoagulants. **Clinical Pearl:** Antithrombin III levels are the most sensitive marker of hypercoagulability in nephrotic syndrome. Levels <60% are associated with significantly increased thrombotic risk, particularly for renal vein thrombosis (RVT). ### Clinical Manifestations of Hypercoagulability 1. **Renal vein thrombosis (RVT):** Most common in membranous nephropathy; presents with flank pain, hematuria, acute kidney injury. 2. **Deep vein thrombosis (DVT):** Occurs in ~5–10% of nephrotic patients. 3. **Pulmonary embolism (PE):** Complication of DVT; life-threatening. 4. **Arterial thrombosis:** Less common but reported (stroke, MI). **Mnemonic:** **ANTI-LOSS** = **ANTIcoagulants LOSS** in nephrotic syndrome → hypercoagulability. Remember: anticoagulants are lost (bad), procoagulants are made (worse). ### Why This Mechanism, Not Others - ~~Decreased platelet count~~ — Platelet counts are typically normal or elevated in nephrotic syndrome; thrombocytopenia is not a feature. - ~~Increased fibrinolytic activity~~ — The opposite occurs; fibrinolysis is **impaired** due to loss of plasminogen and increased synthesis of fibrinolysis inhibitors (PAI-1). - ~~Reduced hepatic synthesis of vitamin K–dependent factors~~ — Hepatic synthesis is actually **increased**, not decreased. Vitamin K deficiency is not a mechanism in nephrotic syndrome. 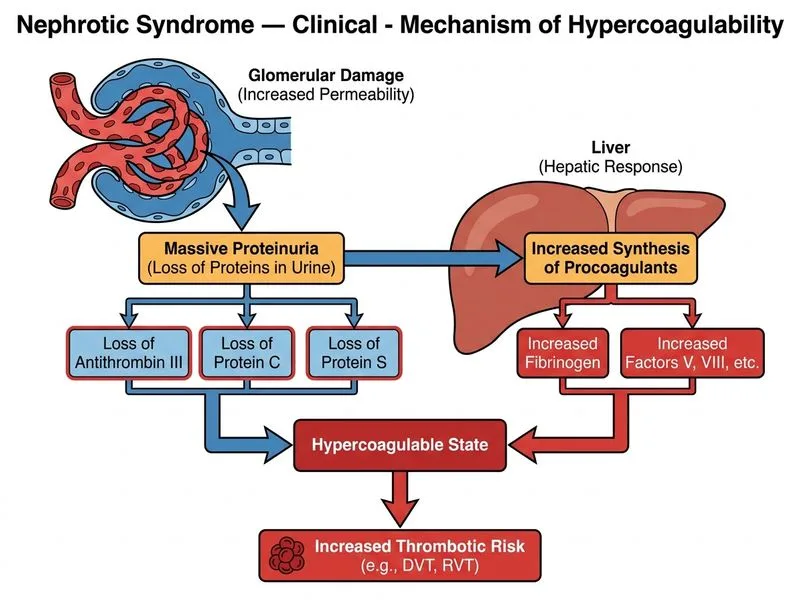
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.