## Clinical Diagnosis: Diabetic Nephropathy with Nephrotic Syndrome ### Clinical Context: Diabetic Kidney Disease **Key Point:** Diabetic nephropathy is the leading cause of chronic kidney disease and end-stage renal disease (ESRD) in developed countries. It typically progresses through five stages: normal kidney function with normal albumin excretion → microalbuminuria → overt proteinuria → declining GFR → ESRD. ### Diagnostic Features Supporting Diabetic Nephropathy | Feature | Finding | Significance | |---------|---------|---------------| | **Duration of diabetes** | 10 years | Sufficient time for diabetic kidney disease to develop | | **Renal function decline** | Cr 2.8, BUN 68 | Stage 3b–4 CKD; progressive renal dysfunction typical of DN | | **Nephrotic range proteinuria** | 6.5 g/24 h | Indicates glomerular damage and tubular dysfunction | | **Hypertension** | 158/94 mmHg | Both cause and consequence of diabetic nephropathy | | **Kidney size & echogenicity** | 9 cm, increased echo | Chronic kidney disease changes; DN causes glomerulosclerosis and fibrosis | | **Hematuria** | 2+ on urinalysis | Can occur in advanced DN; indicates glomerular injury | | **Hypoalbuminemia** | 2.4 g/dL | From proteinuria and malnutrition | | **Electrolyte abnormalities** | Na 132, K 5.8 | Hyponatremia (SIADH, volume overload); hyperkalemia (reduced GFR, RAS activation) | | **Complement levels** | C3, C4 normal | Rules out immune-mediated GN (post-infectious, lupus, MPGN) | | **Hyaline casts only** | Few casts | Non-specific; RBC casts would suggest active GN | ### Pathophysiology of Diabetic Nephropathy **High-Yield:** Diabetic nephropathy involves **hyperglycemia-induced glomerular injury** through multiple mechanisms: 1. **Hemodynamic changes** — afferent arteriole vasodilation → increased glomerular capillary pressure → hyperfiltration 2. **Metabolic injury** — advanced glycation end products (AGEs), protein kinase C (PKC) activation, oxidative stress 3. **Glomerular pathology** — nodular glomerulosclerosis (Kimmelstiel-Wilson lesions), basement membrane thickening, mesangial expansion 4. **Progressive fibrosis** — tubular atrophy, interstitial fibrosis, arteriosclerosis ### Clinical Pearl **Clinical Pearl:** The **classic triad of diabetic nephropathy** is: 1. Proteinuria (often nephrotic range in advanced disease) 2. Hypertension (present in >80% of diabetic patients with nephropathy) 3. Progressive decline in GFR The presence of diabetic retinopathy (not mentioned but often coexists) further supports the diagnosis, as ~95% of patients with diabetic nephropathy have concurrent retinopathy. ### Why Diabetic Nephropathy Is Most Likely 1. **Long-standing diabetes (10 years)** with classic progression to nephrotic-range proteinuria 2. **Progressive renal dysfunction** (Cr 2.8) — DN is the only diagnosis that causes both nephrotic syndrome AND declining GFR 3. **Hypertension** — both a cause and consequence of DN 4. **Bilateral kidney involvement** with increased echogenicity — consistent with chronic diabetic changes 5. **Normal complement levels** — excludes immune-mediated GN 6. **Absence of systemic features** — no mention of rash, arthritis, or other autoimmune manifestations ### Mnemonic: "DIABETIC KIDNEY" - **D**iabetes duration >5 years - **I**ncreased kidney echogenicity - **A**lbuminuria/proteinuria (nephrotic range) - **B**ilateral kidney involvement - **E**lectrolyte abnormalities (hypokalemia or hyperkalemia) - **T**ime-dependent progression (Stage 1→5) - **I**ncreased kidney size (early) → decreased (late) - **C**omplements normal (distinguishes from immune GN) - **K**idney function decline (progressive GFR loss) - **I**nterstitial fibrosis on biopsy - **D**iabetic retinopathy often coexists - **N**odular glomerulosclerosis (Kimmelstiel-Wilson) - **E**nd-stage renal disease risk - **Y**ears of hypertension ### Management Implications **High-Yield:** First-line therapy for diabetic nephropathy with proteinuria includes: - ACE inhibitors or ARBs (reduce intraglomerular pressure, slow progression) - Tight glycemic control (target HbA1c ~7%) - Blood pressure control (target <130/80 mmHg per KDIGO) - Diuretics for volume overload and edema - Statins for cardiovascular risk reduction 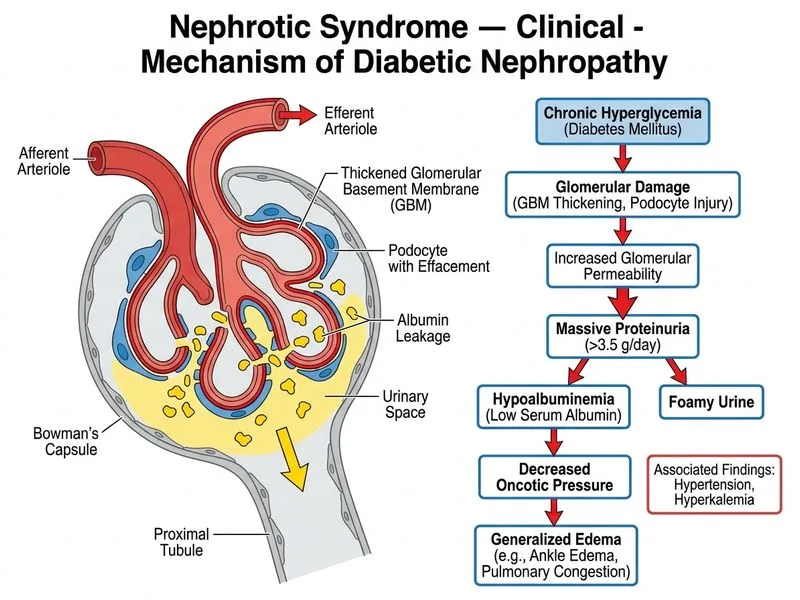
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.