## Distinguishing DPGN from Membranous Nephropathy ### Clinical Presentation Comparison | Feature | DPGN (Proliferative) | Membranous Nephropathy | |---------|---------------------|------------------------| | **Hematuria** | Present (active urinary sediment) | Absent or microscopic | | **Hypertension** | Common, often marked | Uncommon, late feature | | **Renal function** | May be impaired at presentation | Usually preserved initially | | **Proteinuria selectivity** | Non-selective | Selective | | **Complement levels** | Low (C3, C4) | Normal | | **Onset** | Acute or subacute | Insidious, chronic | | **Progression** | Rapid (weeks to months) | Slow (years) | ### Key Distinguishing Feature **Key Point:** Hematuria with hypertension is the hallmark discriminator of DPGN. The presence of active urinary sediment (RBC casts, dysmorphic RBCs) and elevated blood pressure reflects the proliferative, inflammatory nature of the disease and indicates glomerular injury beyond simple protein leakage. **High-Yield:** DPGN = **proliferation** → inflammation → hematuria + HTN. Membranous = **basement membrane thickening** → protein leak only → no hematuria, no HTN (until late). ### Why This Matters Clinically **Clinical Pearl:** A patient with nephrotic syndrome who also has hematuria and hypertension should immediately raise suspicion for a proliferative or secondary glomerulonephritis (DPGN, MPGN, lupus nephritis) rather than primary membranous disease. This distinction guides immunosuppressive therapy decisions. **Mnemonic:** **HYPE** = **H**ematuria + **Y**ellow (active sediment) + **P**roliferation + **E**levated BP → think DPGN, not membranous. [cite:Harrison 21e Ch 279] 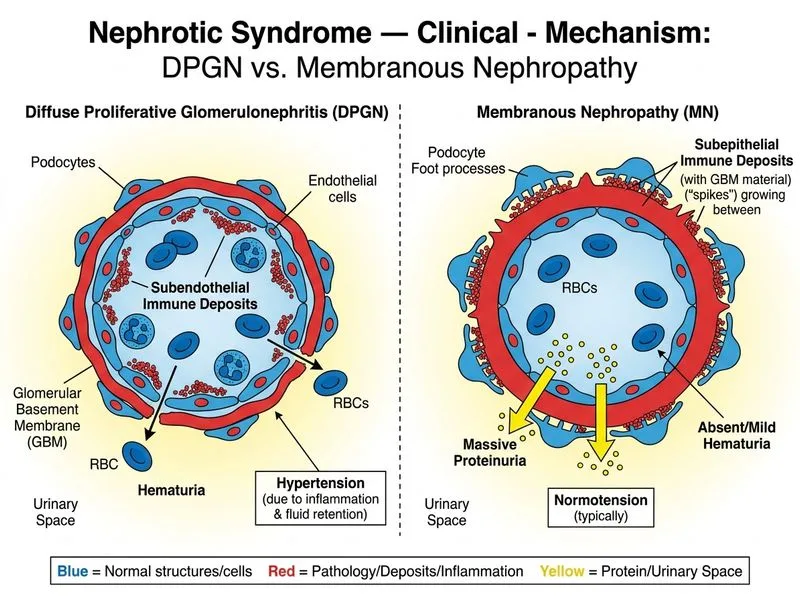
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.