## Diagnosis: Myelomeningocele **Key Point:** Myelomeningocele is the most common and severe form of open neural tube defect (NTD), characterized by herniation of both meninges AND neural tissue (spinal cord) through a vertebral defect. ### Clinical Features of Myelomeningocele | Feature | Myelomeningocele | Meningocele | Anencephaly | Encephalocele | |---------|------------------|-------------|-------------|---------------| | **Contents** | Meninges + spinal cord | Meninges only | Absent brain vault | Brain tissue + meninges | | **Neurological deficit** | Yes (paralysis, incontinence) | No or minimal | Incompatible with life | Variable | | **AFP elevation** | Marked | Mild–moderate | Severe | Moderate | | **Location** | Lumbosacral > thoracic | Lumbosacral | Occipital region | Occipital > frontal | | **Prognosis** | Guarded; lifelong disability | Good if closed early | Lethal | Fair–good | **Clinical Pearl:** The presence of **lower limb paralysis and sphincter dysfunction** is pathognomonic for myelomeningocele — it indicates spinal cord involvement. Meningocele does not cause neurological deficits because the cord is not herniated. ### Embryological Basis 1. **Neural tube closure defect** occurs between weeks 3–4 of gestation (primary neurulation). 2. **Failure of fusion** of neural folds in the midline → persistent communication between neural canal and amniotic cavity. 3. **Herniation of spinal cord** through the vertebral defect → exposure to amniotic fluid → further damage and scarring. 4. **Marked AFP leakage** into amniotic fluid and maternal circulation due to open defect. ### Why Markedly Elevated AFP? **High-Yield:** Open neural tube defects (anencephaly, myelomeningocele) cause **massive AFP leakage** from exposed fetal tissue into amniotic fluid and then into maternal serum. This makes **maternal serum AFP > 2.5 MoM (multiples of median)** a sensitive screening marker for open NTDs at 15–20 weeks gestation. ### Management Overview ```mermaid flowchart TD A[Prenatal diagnosis of myelomeningocele]:::outcome --> B{Gestational age?}:::decision B -->|< 24 weeks| C[Counseling + termination option]:::action B -->|≥ 24 weeks| D[Fetal MRI for assessment]:::action D --> E[Delivery planning]:::action E --> F[Postnatal neurosurgical closure within 48 hrs]:::action F --> G[Long-term: orthopedic, urological, rehabilitation care]:::action ``` **Mnemonic for NTD types: MACE** - **M**yeloMeningocele (cord + meninges) - **A**nencephaly (absent brain vault) - **C**erebral/spinal defects - **E**ncephalocele (brain herniation) **Key Point:** Folic acid supplementation (5 mg daily) **periconceptionally and throughout first trimester** reduces NTD risk by ~70%. This is why all women of reproductive age in India are advised folic acid supplementation. 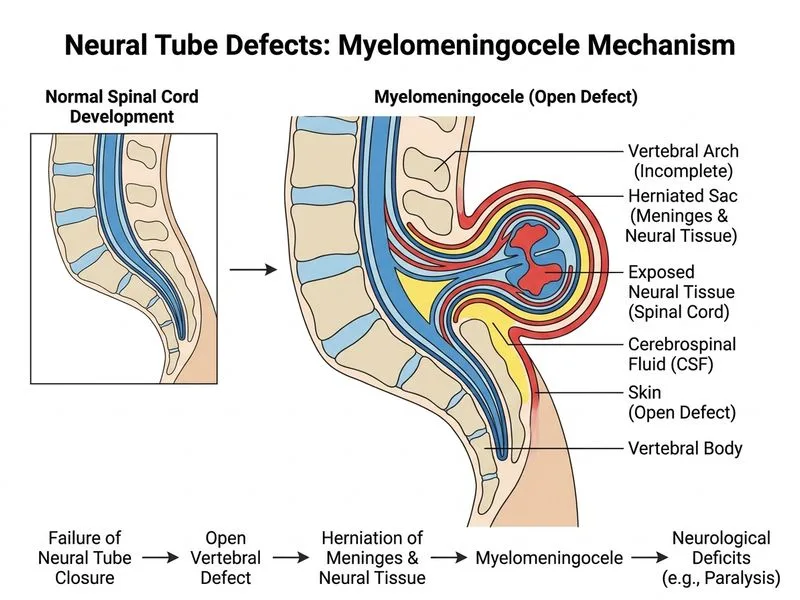
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.