## Clinical Context This is a case of prenatally diagnosed open neural tube defect (spina bifida) detected on second-trimester ultrasound with biochemical confirmation (elevated maternal AFP). The fetus has exposed neural tissue, indicating a severe defect. ## Management Algorithm for Prenatally Diagnosed NTD ```mermaid flowchart TD A[Open NTD diagnosed prenatally]:::outcome --> B{Detailed imaging & counseling done?}:::decision B -->|No| C[Detailed fetal ultrasound + MRI<br/>Assess severity & prognosis<br/>Genetic counseling]:::action B -->|Yes| D{Parental decision}:::decision D -->|Continue pregnancy| E[Multidisciplinary planning<br/>Delivery at tertiary center<br/>Postnatal surgery arranged]:::action D -->|Terminate| F[Counseling & support<br/>Arrange safe termination<br/>Karyotype if desired]:::action C --> D ``` ## Why Detailed Counseling & Imaging is the Next Step **Key Point:** Once an open NTD is suspected on screening ultrasound, the immediate priority is **confirmatory detailed imaging and comprehensive parental counseling** regarding prognosis, functional outcomes, and management options — NOT empirical treatment or emergency intervention. **High-Yield:** The standard of care for prenatally diagnosed open NTD is: 1. Confirm diagnosis with high-resolution ultrasound ± fetal MRI 2. Assess severity (level of lesion, presence of hydrocephalus, Chiari malformation) 3. Provide genetic counseling and discuss prognosis 4. Discuss all options: continuation with planned tertiary delivery, termination of pregnancy, or in-utero repair (in select centers) 5. If continuation chosen: arrange delivery at a center with pediatric neurosurgery capability **Clinical Pearl:** Elevated maternal AFP + ultrasound findings of open NTD = diagnosis is already confirmed. Amniocentesis is not needed for diagnosis confirmation; it may be offered for karyotyping if there are other anomalies or parental preference, but it is NOT the immediate next step. ## Why Folic Acid Supplementation Alone is Insufficient Folic acid supplementation at this stage (16 weeks, defect already formed) cannot reverse an established neural tube defect. Folic acid's role is in **primary prevention** (periconceptional period). Once the defect is present, management is counseling and delivery planning. ## Why Amniocentesis is Not First-Line While karyotyping may be offered to rule out associated chromosomal abnormalities (e.g., trisomy 13, 18), it is **not** the immediate next step. The diagnosis is already established by imaging. Amniocentesis carries a small risk of miscarriage and should follow detailed counseling. ## Why Corticosteroids & Planned Cesarean Section Alone Are Premature These interventions assume the pregnancy will continue and are part of the **delivery plan**, but they come **after** detailed counseling and parental decision-making. Administering corticosteroids before the parents have been fully counseled about prognosis and options is not appropriate. ## Summary Table: Management Sequence | Step | Timing | Rationale | |------|--------|----------| | Detailed ultrasound + MRI | Immediately after diagnosis | Assess severity, level, associated anomalies | | Genetic counseling | Before parental decision | Discuss prognosis, outcomes, options | | Parental counseling | Before parental decision | Discuss continuation, termination, in-utero repair | | Karyotyping (if desired) | After counseling | Rule out chromosomal abnormalities | | Delivery planning | If pregnancy continues | Arrange tertiary center, neurosurgery team | | Corticosteroids | If pregnancy continues, at 24 weeks | Fetal lung maturity | **Key Point:** Counseling and informed decision-making are the cornerstone of management for prenatally diagnosed NTDs. The parents must understand the prognosis (motor/sensory loss, bowel/bladder dysfunction, hydrocephalus, Chiari malformation) and available options before any further intervention. 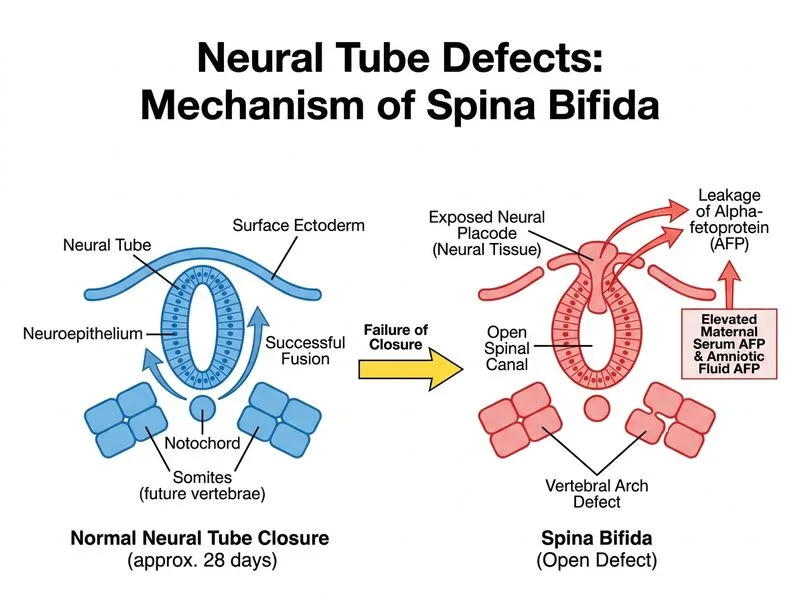
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.