## Management of Early Gestational Sac: Dating and Viability Assessment ### Clinical Context and Dating **Key Point:** At 5 weeks of gestation (by last menstrual period), the gestational sac should measure approximately 2–5 mm. A gestational sac of 8 mm at 5 weeks is larger than expected but still within the range of normal variation or early dating. ### Ultrasound Milestones and Yolk Sac Appearance | Gestational Age (LMP) | Expected GS Size | Yolk Sac | Fetal Pole | CRL | |----------------------|-----------------|----------|-----------|-----| | 4–5 weeks | 2–5 mm | Not yet visible | Absent | — | | 5–6 weeks | 5–10 mm | Visible (>3 mm) | May appear | — | | 6–7 weeks | 10–15 mm | Visible | Present | <5 mm | | 7–8 weeks | 15–20 mm | Visible | Present | 5–10 mm | **High-Yield:** The **yolk sac should be visible when the gestational sac measures 6–7 mm**. Its absence at a GS size of 8 mm raises the question of dating error or early pregnancy loss, but does not definitively establish either. ### Differential Diagnosis: Three Scenarios ```mermaid flowchart TD A[GS 8 mm, no yolk sac at reported 5 weeks]:::outcome --> B{Repeat scan in 7-10 days}:::decision B -->|Yolk sac appears, GS grows| C[Intrauterine pregnancy, dating error]:::action B -->|GS shrinks or no growth| D[Miscarriage/blighted ovum]:::urgent B -->|No intrauterine GS on repeat| E[Ectopic pregnancy or PUL]:::urgent ``` **Clinical Pearl:** The diagnosis of **pregnancy of unknown location (PUL)** or **ectopic pregnancy** cannot be made on a single scan showing an intrauterine gestational sac without a yolk sac. A follow-up scan is mandatory to establish the diagnosis. ### Why Repeat Ultrasound is the Gold Standard **High-Yield:** The **discriminatory zone** (hCG level above which an intrauterine gestational sac should be visible) is approximately 1000–2000 mIU/mL. However: 1. Dating by LMP can be off by 1–2 weeks 2. A single ultrasound cannot reliably distinguish between: - Early intrauterine pregnancy with dating error - Blighted ovum (anembryonic pregnancy) - Ectopic pregnancy with a pseudosac **Tip:** Serial ultrasound with assessment of **gestational sac growth rate** (should grow ~1 mm per day) and **appearance of yolk sac and fetal pole** is the standard of care for first-trimester viability assessment. ### Why Each Alternative is Wrong 1. **Methotrexate for ectopic pregnancy:** Ectopic pregnancy has NOT been diagnosed. An intrauterine gestational sac is present, which excludes ectopic pregnancy in the vast majority of cases (heterotopic pregnancy is rare, ~1 in 30,000). Methotrexate is contraindicated in confirmed intrauterine pregnancy. 2. **Immediate D&C for miscarriage:** Miscarriage has NOT been confirmed. A single ultrasound showing a small GS without a yolk sac does not establish fetal demise. D&C would be inappropriate and could terminate a viable pregnancy. 3. **CT scan for ectopic pregnancy:** CT is not indicated for first-trimester pregnancy assessment and exposes the patient to unnecessary radiation. Transvaginal ultrasound is the gold standard. ### Management Algorithm **Key Point:** The standard approach to a **small gestational sac without yolk sac** is: 1. Confirm intrauterine location 2. Measure gestational sac diameter and note absence of yolk sac 3. Obtain serum hCG (if not already done) 4. **Schedule repeat transvaginal ultrasound in 7–10 days** 5. Assess for: - Yolk sac appearance (confirms viability) - Fetal pole with cardiac activity (confirms viability) - Gestational sac growth (should grow ~1 mm/day) 6. If no growth or shrinkage, or no yolk sac/fetal pole by 7–8 weeks, diagnose miscarriage ### Reassurance and Counseling **Clinical Pearl:** Many early pregnancies present with dating uncertainty. A 1–2 week discrepancy between LMP dating and ultrasound is common and does not indicate pathology. Serial imaging resolves the uncertainty and guides management. 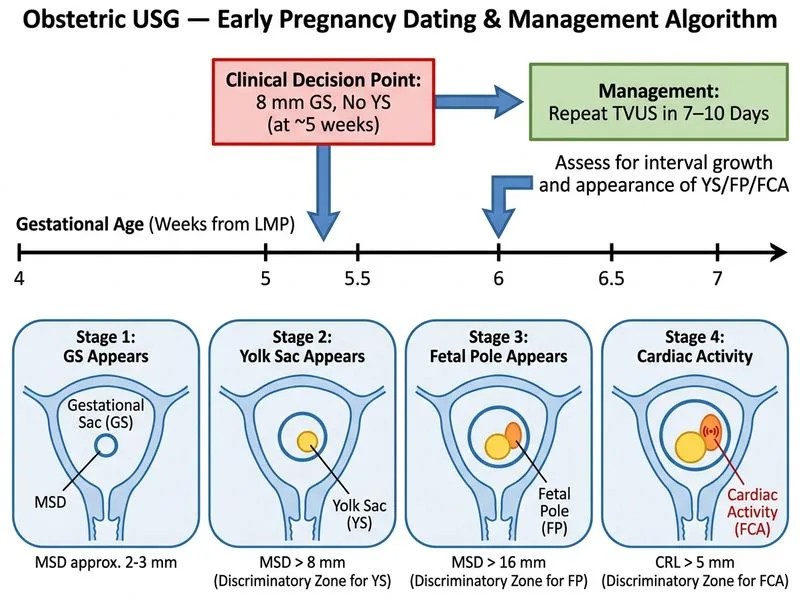
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.