## Dating and Viability Assessment in First Trimester **Key Point:** According to current ACOG/RCOG/SRU guidelines, an MSD ≥16 mm with no embryo (fetal pole) visible on transvaginal ultrasound is diagnostic of a **failed pregnancy (anembryonic pregnancy / blighted ovum)**. Similarly, an MSD ≥8 mm with no yolk sac is also diagnostic of failure. These thresholds were updated (from the older >25 mm cutoff) to reduce false-positive diagnoses of miscarriage while still allowing definitive diagnosis when criteria are clearly met. ### Updated Diagnostic Criteria for Pregnancy Failure (ACOG/SRU 2012 Consensus) | Finding | Diagnostic Threshold (TVS) | Interpretation | |---|---|---| | No yolk sac | MSD ≥ 8 mm | Failed pregnancy | | No embryo (fetal pole) | MSD ≥ 16 mm | Failed pregnancy (anembryonic) | | No cardiac activity | CRL ≥ 7 mm | Embryonic demise | | No embryo at follow-up | MSD growth <1 mm/day over 7–10 days | Failed pregnancy | **High-Yield:** In this vignette, MSD = 18 mm with **no yolk sac and no fetal pole** on transvaginal ultrasound. This **exceeds both thresholds** (≥8 mm without yolk sac AND ≥16 mm without fetal pole), meeting definitive criteria for anembryonic pregnancy. A diagnosis of failed pregnancy can be made on a **single scan** when these thresholds are clearly exceeded. ### Why the Other Options Are Incorrect - **Option A (Ectopic):** An intrauterine gestational sac is already documented; ectopic pregnancy is effectively excluded. Pelvic MRI is not indicated. - **Option B (7–8 weeks normal):** An MSD of 18 mm corresponds to ~9–10 weeks, not 7–8 weeks. At 7–8 weeks, MSD would be ~8–12 mm. Labeling this as "early normal" is factually incorrect. - **Option C (Repeat in 1 week):** While repeat ultrasound is appropriate when findings are equivocal, the MSD of 18 mm here **clearly exceeds** the diagnostic threshold for anembryonic pregnancy. Delaying diagnosis is not warranted when criteria are definitively met. The older threshold of >25 mm has been superseded. **Clinical Pearl:** The 2012 SRU/ACR/ACOG consensus statement lowered the diagnostic threshold for anembryonic pregnancy to MSD ≥16 mm (no embryo) and MSD ≥8 mm (no yolk sac) on transvaginal ultrasound, replacing the older >25 mm cutoff. These conservative thresholds were chosen to avoid false-positive diagnoses while still permitting definitive diagnosis when clearly exceeded. **Management:** Once anembryonic pregnancy is diagnosed, options include expectant management, medical management (misoprostol), or surgical evacuation (uterine aspiration). Immediate evacuation is one valid option, though shared decision-making with the patient is standard practice. *Reference: Doubilet PM et al. "Diagnostic Criteria for Nonviable Pregnancy Early in the First Trimester." NEJM 2013; 369:1443–1451. Also: ACOG Practice Bulletin No. 200.* 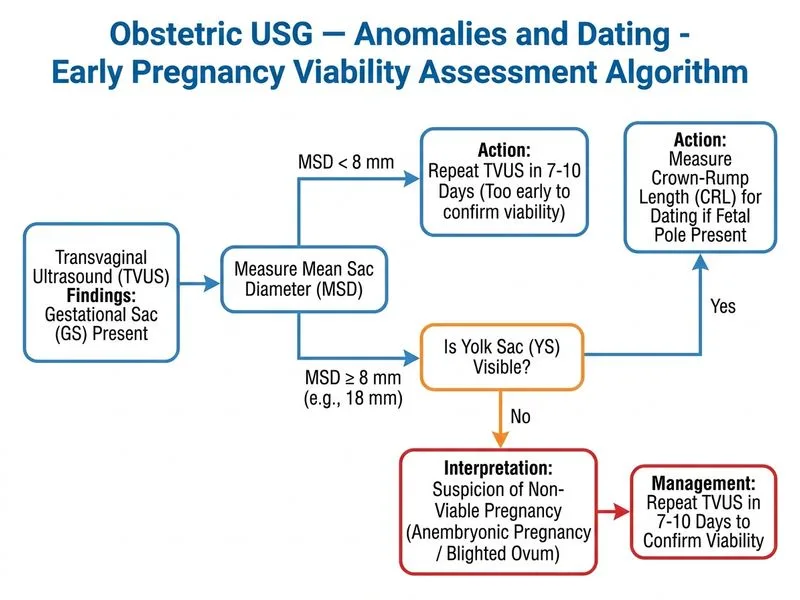
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.