## Clinical Diagnosis: Distal Cholangiocarcinoma This patient presents with **painless jaundice, weight loss, positive Courvoisier's sign (palpable gallbladder), and imaging evidence of a 2.5 cm hypoattenuating lesion at the distal CBD with periductal fibrosis**. The transition point at the distal CBD and normal pancreatic parenchyma on CECT confirm **resectable distal cholangiocarcinoma** (lower third of CBD). There are no distant metastases. **Key Point:** Distal cholangiocarcinoma (lower-third CBD) is anatomically distinct from hilar (Klatskin) and intrahepatic cholangiocarcinoma. Its surgical management follows the same principles as other periampullary malignancies. ## Surgical Management: Why Pancreaticoduodenectomy (Whipple) Is Correct For **resectable distal cholangiocarcinoma**, the standard of care is **Pancreaticoduodenectomy (Whipple procedure)**. This is supported by all major hepatobiliary surgery guidelines (NCCN, ESMO, and standard surgical oncology texts including Blumgart's Surgery of the Liver, Biliary Tract and Pancreas). ### Rationale for Whipple in Distal Cholangiocarcinoma: 1. **Anatomical necessity:** The distal CBD is intimately associated with the head of the pancreas, duodenum, and ampulla. Even when the pancreatic parenchyma appears normal on imaging, the distal CBD cannot be resected with adequate margins without removing the pancreatic head and duodenum en bloc. 2. **R0 resection:** Whipple provides the best chance of achieving negative (R0) margins — the single most important prognostic factor in cholangiocarcinoma. 3. **Regional lymphadenectomy:** Whipple allows en bloc removal of peripancreatic, periduodenal, and hepatoduodenal ligament lymph nodes, which are the primary nodal drainage of distal CBD tumors. 4. **Standard of care:** Blumgart, Sabiston, and Schwartz's Principles of Surgery all cite pancreaticoduodenectomy as the definitive curative resection for distal cholangiocarcinoma, regardless of whether the pancreatic parenchyma is directly invaded. ### Why the Other Options Are Incorrect: | Procedure | Why Incorrect Here | |---|---| | **Choledochoduodenostomy (CDD)** | Appropriate only for **benign** distal CBD strictures (e.g., chronic pancreatitis). Contraindicated in malignancy — does not achieve oncologic margins or lymphadenectomy. | | **Hepaticojejunostomy (HJ) with Roux-en-Y** | Appropriate for **proximal/hilar** cholangiocarcinoma or benign biliary strictures. For distal CC, it does not address the distal CBD tumor or regional lymph nodes adequately. | | **Percutaneous transhepatic drainage + palliative chemotherapy** | Reserved for **unresectable** disease (vascular invasion, distant metastases, poor performance status). This patient has resectable disease with no metastases. | **High-Yield:** The key distinction is that **distal cholangiocarcinoma = Whipple procedure**, regardless of whether the pancreatic head appears grossly normal. The distal CBD is anatomically inseparable from the pancreatic head for surgical purposes. This is analogous to ampullary carcinoma and pancreatic head carcinoma — all three periampullary tumors are treated with Whipple. **Clinical Pearl (Blumgart / Sabiston):** "Resectable distal cholangiocarcinoma is treated by pancreaticoduodenectomy (Whipple procedure). This provides en bloc resection of the distal bile duct, pancreatic head, duodenum, and regional lymph nodes, offering the only chance of cure." **Mnemonic:** **Distal CC → Whipple; Hilar CC → Hepatectomy ± biliary reconstruction; Intrahepatic CC → Hepatic resection** 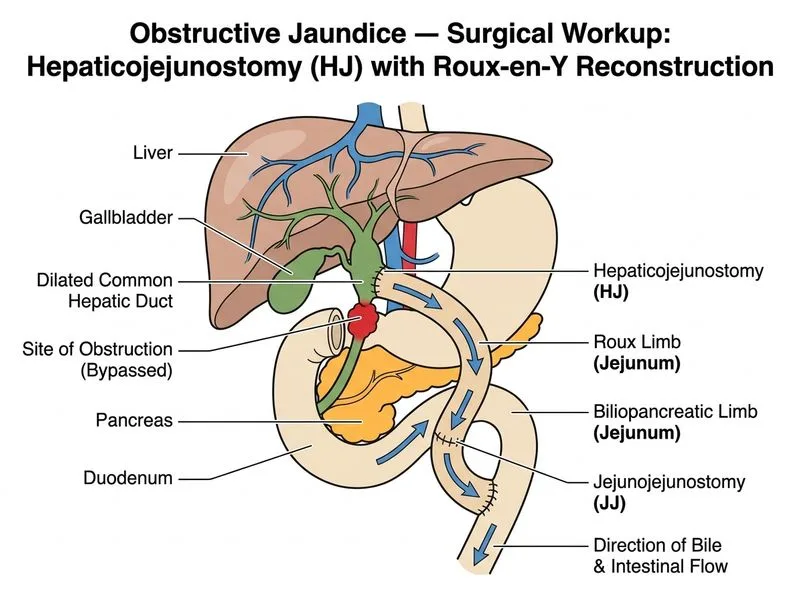
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.