## Assessment of Treatment-Resistant OCD ### Clinical Definition of Treatment Resistance **Key Point:** Treatment-resistant OCD is defined as inadequate response (typically <25% reduction in Y-BOCS score) after: - Adequate SSRI trial (≥12 weeks at therapeutic dose), OR - Trial of at least 2 different SSRIs at adequate doses and duration **High-Yield:** Before labeling OCD as "treatment-resistant," clinicians must systematically evaluate: 1. **Dosage adequacy** — Is the SSRI at therapeutic range? 2. **Adherence** — Is the patient taking the medication as prescribed? 3. **Trial duration** — Has sufficient time elapsed (≥12 weeks minimum)? 4. **Comorbidity** — Are depression, anxiety, or personality factors limiting response? ### Why Repeat Y-BOCS + Clinical Reassessment Is the Investigation of Choice **Clinical Pearl:** The first step in managing apparent treatment resistance is NOT neuroimaging but systematic clinical evaluation using the same validated outcome measure (Y-BOCS) to: - Confirm persistent severity objectively - Verify SSRI dose is adequate (e.g., sertraline 50–200 mg/day; some patients need 200+ mg) - Confirm ≥12 weeks of continuous therapy - Assess medication adherence and side effects - Identify comorbid conditions (depression, anxiety, personality pathology) that may impair response Once these factors are confirmed adequate, escalation to augmentation (e.g., antipsychotic add-on) or alternative therapies (intensive CBT/ERP, neurosurgical interventions) is justified. ### Neuroimaging in OCD: Research vs. Clinical Practice | Investigation | Role in OCD | Clinical Utility | |---|---|---| | fMRI | Research: maps hyperactivity in OFC-striatal circuits | Not routine; does not guide treatment decisions | | PET-FDG | Research: detects metabolic abnormalities | Not routine; expensive; does not change management | | Y-BOCS reassessment | Clinical: objective severity measurement & treatment monitoring | **Gold standard for assessing response & resistance** | | EEG | Research: investigates neural oscillations | Not diagnostic or prognostic in OCD | **Warning:** Neuroimaging (fMRI, PET) is valuable for understanding OCD neurobiology in research settings but does NOT guide clinical decision-making and should not be ordered in routine practice for treatment planning. Overreliance on imaging delays appropriate clinical escalation (dose optimization, augmentation, or intensive psychotherapy). ### Algorithm for Treatment-Resistant OCD ```mermaid flowchart TD A[OCD patient on SSRI with inadequate response]:::outcome A --> B[Repeat Y-BOCS assessment]:::action B --> C{Y-BOCS reduction ≥25%?}:::decision C -->|Yes| D[Continue current SSRI]:::action C -->|No| E{Adequate dose & duration?}:::decision E -->|No| F[Optimize SSRI dose or extend trial]:::action E -->|Yes| G{Adherence confirmed?}:::decision G -->|No| H[Address barriers to adherence]:::action G -->|Yes| I[True treatment resistance]:::outcome I --> J[Consider augmentation or switch SSRI]:::action J --> K[Add intensive CBT/ERP]:::action ``` **Mnemonic:** **DARE** — **D**osage, **A**dherence, **R**esponse duration, **E**valuation (reassess with Y-BOCS before escalating). 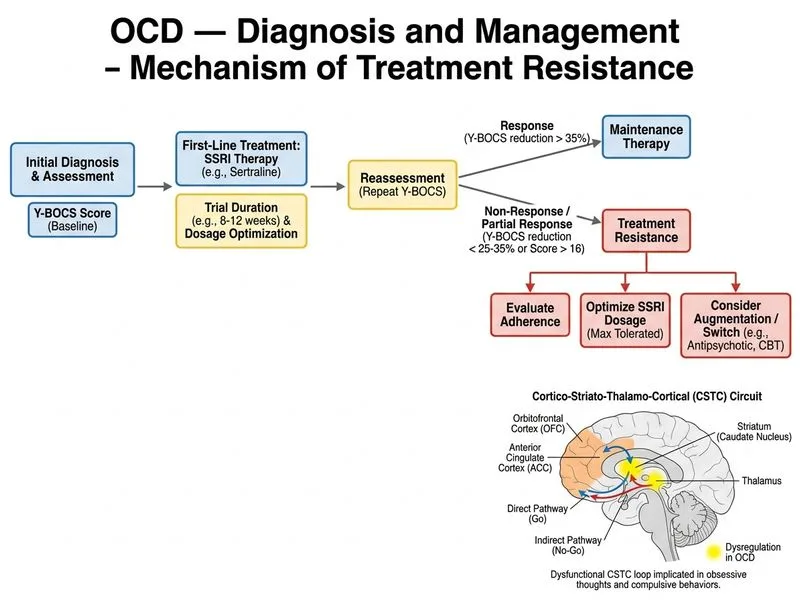
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.