## Clinical Assessment **Key Point:** This patient has severe, treatment-resistant OCD (inadequate response to adequate SSRI dose and duration). The obsessions are harm-related (aggressive intrusions), and compulsions are safety-checking behaviors. Diagnosis is clear; the challenge is optimizing treatment. ## Definition of Treatment Resistance **High-Yield:** Treatment-resistant OCD is defined as: - Inadequate response (< 25% reduction in Yale-Brown Obsessive-Compulsive Scale [Y-BOCS] score) after - ≥ 8–12 weeks of SSRI at therapeutic dose (fluoxetine 60 mg is adequate) - With documented compliance This patient meets criteria: 3 months on fluoxetine 60 mg with minimal improvement. ## Management Algorithm for Treatment-Resistant OCD ```mermaid flowchart TD A[OCD diagnosed]:::outcome --> B[SSRI at therapeutic dose<br/>for 8-12 weeks]:::action B --> C{Adequate response?}:::decision C -->|Yes| D[Continue SSRI<br/>+ CBT/ERP]:::action C -->|No| E[Treatment-resistant OCD]:::outcome E --> F{Optimize current SSRI?}:::decision F -->|Increase dose or<br/>extend duration| G[Reassess at 12 weeks]:::action F -->|Switch to<br/>clomipramine| H[Clomipramine trial<br/>100-150 mg/day]:::action G --> I{Response?}:::decision H --> I I -->|Yes| J[Continue + CBT/ERP]:::action I -->|No| K[Add augmentation agent]:::action K --> L[Antipsychotic:<br/>risperidone, aripiprazole]:::action L --> M{Response?}:::decision M -->|Partial| N[Consider intensive CBT/ERP]:::action M -->|No| O[Consider specialist referral<br/>or advanced options]:::action ``` **Clinical Pearl:** Switching from one SSRI to another or to clomipramine is reasonable before augmentation, as response rates vary between agents (30–50% switch response). ## Options for Treatment-Resistant OCD | Strategy | Evidence | Timeline | Notes | | --- | --- | --- | --- | | **Switch to clomipramine** | Strong | 8–12 weeks at therapeutic dose | 30–50% of SSRI non-responders respond | | **Augment with antipsychotic** | Strong | 4–6 weeks (risperidone, aripiprazole) | Add to current SSRI; low-dose risperidone 2–6 mg/day | | **Intensive CBT/ERP** | Strong | 16–20 sessions over 8–12 weeks | Gold standard; should accompany pharmacotherapy | | **Increase SSRI dose** | Weak | 4–6 weeks | Fluoxetine 60 mg is already adequate; higher doses show minimal additional benefit | | **Augment with other agents** | Weak | Variable | Augmentation with clonazepam, lamotrigine, or N-acetylcysteine has limited evidence | ## Most Appropriate Next Step **High-Yield:** The best next step is **augmentation with a low-dose antipsychotic (risperidone 2–4 mg/day or aripiprazole 10–15 mg/day) added to the current fluoxetine**, with concurrent referral for intensive CBT/ERP. **Rationale:** 1. Fluoxetine 60 mg is already at therapeutic dose; further dose escalation offers minimal benefit 2. Switching to clomipramine is a reasonable alternative, but augmentation has faster onset and strong evidence 3. Risperidone or aripiprazole augmentation has FDA support and robust evidence in treatment-resistant OCD (response rate ~60%) 4. **CBT/ERP is essential:** Medication alone is insufficient; intensive behavioral therapy with exposure and response prevention should be initiated concurrently **Warning:** Do NOT simply increase fluoxetine beyond 60 mg or add benzodiazepines as first-line augmentation. Antipsychotics have the strongest evidence. ## Expected Outcomes - **With augmentation + CBT/ERP:** 50–70% achieve significant improvement (≥35% Y-BOCS reduction) - **Timeline:** 4–6 weeks for antipsychotic effect; 8–12 weeks for full CBT/ERP benefit **Clinical Pearl:** Harm-related obsessions (like this patient's fear of harming his daughter) often respond well to ERP, as the feared outcome (actual harm) is extremely unlikely, making habituation achievable. [cite:Harrison 21e Ch 385; American Psychiatric Association Practice Guidelines for OCD] 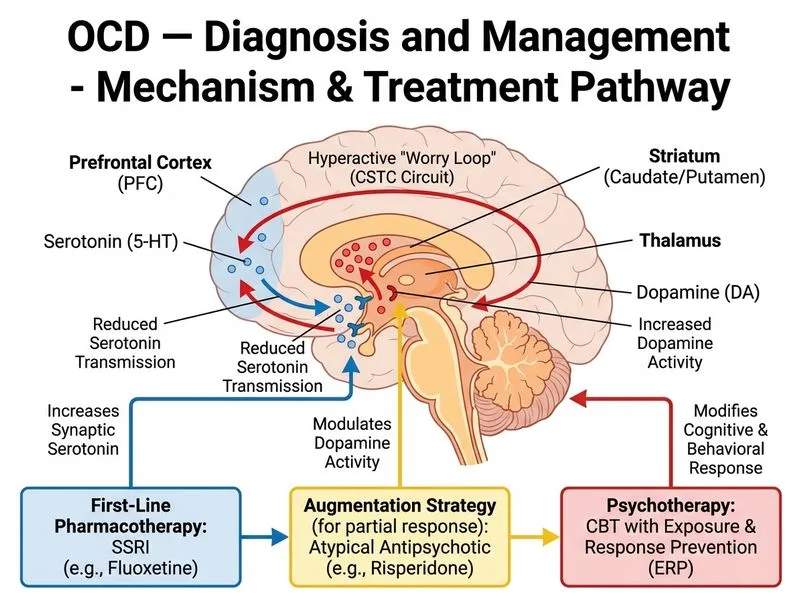
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.