## Diagnosis and Clinical Reasoning **Key Point:** This patient presents with obsessive-compulsive disorder (OCD) with harm obsessions and compulsive checking/reassurance-seeking. The critical diagnostic feature is that she recognizes the thoughts as intrusive, unwanted, and irrational—and she has NO actual intent to harm. This distinguishes OCD from psychotic disorders or genuine intent-based violence risk. ### Diagnostic Criteria Met | Feature | Present? | Significance | |---------|----------|-------------| | Intrusive, unwanted thoughts | Yes | Core obsession | | Anxiety/distress from thoughts | Yes | Obsessions cause significant distress | | Compulsive behaviors (checking, reassurance) | Yes | Rituals to neutralize anxiety | | Insight intact (recognizes as irrational) | Yes | Rules out psychosis; indicates good prognosis | | No actual intent or urge to harm | Yes | Differentiates from genuine violence risk | | Functional impairment (4-year duration) | Yes | Meets duration and severity criteria | **High-Yield:** OCD with harm obsessions is one of the most distressing presentations but carries **low actual violence risk** because patients have intact insight and ego-dystonic thoughts. Misdiagnosis as psychosis or personality disorder leads to inappropriate hospitalization and separation. ### Management Algorithm ```mermaid flowchart TD A[OCD with harm obsessions]:::outcome --> B{Insight intact?}:::decision B -->|Yes, ego-dystonic| C[First-line: SSRI + CBT-ERP]:::action B -->|No, psychotic| D[Antipsychotic + inpatient]:::action C --> E[Sertraline 50-200 mg daily]:::action C --> F[Exposure and Response Prevention]:::action F --> G[Habituation and anxiety reduction]:::outcome E --> H[Reassess at 4-6 weeks]:::decision H -->|Response| I[Continue + optimize ERP]:::action H -->|No response| J[Increase dose or switch SSRI]:::action ``` ### First-Line Treatment 1. **SSRI therapy** (sertraline, paroxetine, fluoxetine) - Sertraline starting dose: 50 mg daily, titrate to 100–200 mg over 4–6 weeks - Response typically takes 8–12 weeks (longer than depression) - Efficacy: ~60% response rate in OCD 2. **Cognitive-behavioral therapy with Exposure and Response Prevention (ERP)** - Gold standard psychological intervention - Patient is exposed to harm-related triggers (e.g., being alone with child, discussing harm scenarios) without performing reassurance-seeking or checking - Habituation reduces anxiety over repeated exposures - Combination SSRI + ERP is superior to either alone **Clinical Pearl:** Reassurance-seeking and checking are **safety behaviors** that maintain OCD by preventing habituation. The therapist must actively discourage these, even though the patient's anxiety temporarily worsens during ERP. **Warning:** Do NOT prescribe benzodiazepines as monotherapy—they provide short-term relief but worsen long-term prognosis by preventing habituation and creating dependence. ### Why Hospitalization and Child Separation Are Inappropriate - **No imminent safety risk:** Intact insight + no urge to harm = low violence risk - **Hospitalization reinforces avoidance:** Separating the child confirms the patient's fear that she is dangerous, worsening obsessions - **Evidence-based care:** Exposure-based therapy requires the patient to face feared situations (being with the child) in a controlled, supported manner - **Harm to child:** Unnecessary separation causes psychological trauma to the child and damages the therapeutic alliance **High-Yield:** OCD with harm obsessions is frequently mismanaged by well-meaning clinicians who hospitalize or separate families. This is a **common NEET PG trap question**—the correct answer prioritizes evidence-based OCD treatment, not avoidance. 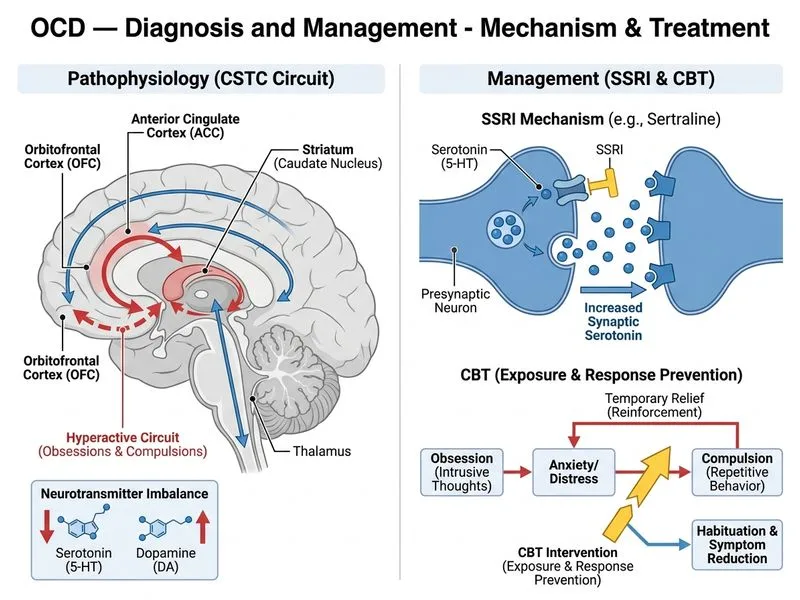
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.